The Basal cell carcinoma, short Basalioma is a semi-malignant skin cancer that almost always occurs locally and does not tend to form metastases. However, if left untreated, basalioma can grow and damage surrounding tissue, bones, or cartilage.
What is a basalioma (basal cell carcinoma)?
.jpg)
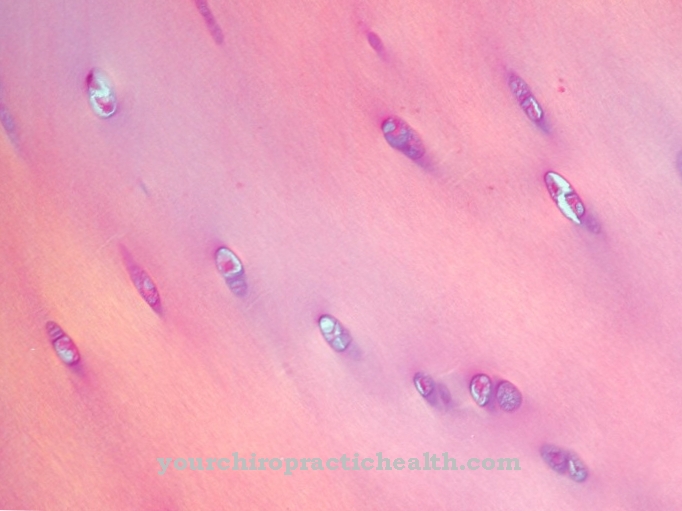
The basalioma develops from the basal cells of the epidermis and can take various forms. The skin-colored change is typical of the basalioma.
The pigmented basalioma, however, occurs less often. The skin tumor usually appears as a lump, but can also assume the shape of a hemisphere, crater-shaped with a raised edge or grow like a scar.
Basaliomas usually develop in sun-exposed areas such as the head, face, neck and décolleté. Basaliomas are extremely rare on the trunk and limbs.
Fair-skinned people have an increased risk of developing basal cell carcinoma. While in the past decades the basalioma often only appeared in people over 60 years of age, more and more younger people are developing this form of skin cancer.
causes
The cause of a basalioma is primarily the change in leisure behavior. This includes regular visits to solariums and vacation trips to countries with intense solar radiation. Excessive sunbathing promotes the formation of sunburns and, as a result, skin tumors.
In Germany, about 0.1 percent of the population will develop basal cell carcinoma in their lifetime.
When exposed to intense sunlight, the UV rays damage the DNA of the skin cells and a basalioma can form. The indirect effect of excessive sun exposure is the weakening of the immune system, which in turn can promote the development of skin tumors.
A certain genetic predisposition and certain skin diseases such as psoriasis, hypersensitivity to light, a tendency to sun allergies, etc. are also possible causes for the formation of a basalioma.
Symptoms, ailments & signs
_2.jpg)
In most cases, the basalioma arises in a location that has already been damaged by the skin. So-called sun damage is particularly typical here. The affected skin area, which has mostly been exposed to the sun for years and has also suffered sunburn, takes on a pink-red to light red color.
This is the preliminary stage of a basalioma, which can still be treated well under the supervision of a dermatologist. Regeneration is only possible in very few cases, but the formation of a basalioma can be delayed or prevented. If the basalioma develops from the existing skin damage, this is usually not noticeable for the person concerned, but can only be determined by the doctor with a special lamp.
A tissue sample must be taken for a final diagnosis. Basalioma itself does not cause any direct symptoms such as pain or inflammation. A scaly crust on its surface can be observed in some cases. If the existing basalioma continues to be exposed to the sun, it can become more reddened and develop a slightly bloody surface, as can be seen, for example, when a mosquito bite heals.
Signs of the formation of a basalioma can basically be any noticeable change in the skin in one or more places. Regular check-ups with a dermatologist are advisable to prevent major damage.
Diagnosis & course
Basaliomas grow very slowly, usually over years. They form superficial skin changes like small nodules that are initially hardly noticed. If the basalioma is left untreated, it will continue to grow. The nodule can grow inwards in the middle, whereby only a raised edge remains visible, which itself consists of lots of small nodules that look like strung on a string of pearls.
The ulcer-like basalioma, on the other hand, looks like a small non-healing skin lesion that may be covered with scabs. If you take a closer look, you can see the blood vessels that feed the skin tumor in all forms of basal cell carcinoma.
The less common pigmented basalioma has a reddish-brown color that can sometimes appear very dark. In this case, it is essential to distinguish it from the dangerous black skin cancer, which often looks like a dark mole. Basaliomas are usually not sensitive to pain.
The clear diagnosis of a basalioma is made after the microscopic-histological examination. In order to determine the spread of the skin tumor, the affected skin area and its surroundings are treated with a special cream. The tumor cells can then be made visible with a special lamp.
Complications
Since basal cell carcinoma is a cancer, the various complications of a tumor occur. In most cases, the diagnosis is made relatively late because the basal cell carcinoma develops over a number of years and is hardly visible from the outside.
However, if it spreads strongly, lumps on the skin can occur, which are often covered with scabs. In most cases, the carcinoma can be demarcated relatively easily from a mole. If the black spots appear in an unfavorable place, psychological problems can also arise due to optical restrictions.
Basal cell carcinoma is usually treated by removal. The tissue is usually removed without complications, although healthy tissue around the tumor is also removed. Other methods of tumor removal can be used in hard-to-reach places.
In most cases, a new formation of the basal cell carcinoma cannot be prevented, so that the patient may have to undergo another surgical procedure to remove it. Since the tumor only occurs locally, no further tissue is damaged, so there are no further complications. Basal cell carcinoma does not reduce life expectancy.
When should you go to the doctor?
If a basalioma is not treated, this complaint can, in the worst case, lead to the death of the patient. For this reason, any unclear areas on the skin or any noticeable areas on the skin must always be examined by a dermatologist. This can prevent complications in later years. As a rule, the patient should then consult a doctor if certain abnormalities occur on the skin. Pigment spots can change in color, shape or size.
If at least one of these changes is present, a doctor must be consulted in any case. If the basalioma is detected, the disease progresses positively and the life expectancy of the person affected is not reduced. The person concerned is dependent on the use of sun protection in order to avoid further discomfort. A dermatologist should always be consulted with a basal cell carcinoma or other changes on the skin. In acute emergencies, the hospital can also be visited directly. As a rule, various preventive examinations can also be carried out in order to avoid skin cancer.
Doctors & therapists in your area
Treatment & Therapy
There are various options available for treating basal cell carcinoma, depending on the size and spread of the carcinoma. In most cases, the basal cell carcinoma is surgically removed under local anesthesia. A few millimeters of healthy tissue around the tumor are also removed to make sure that all of the extensions of the basalioma have been removed.
If the basalioma is in an unfavorable place, radiation therapy can also be used. Cryotherapy (freezing with liquid nitrogen) or phototherapy (treatment of the tumor with light-sensitive substances) also promise good therapeutic success.
The chances of recovery from the basal cell carcinoma are very good, with the fewest recurrences (neoplasms) to be expected after surgical removal.
Outlook & forecast
If the basal cell carcinoma is diagnosed and treated early, the patient has good prospects of recovery. The doctor removes the skin lesions in an operation or radiation therapy. The treatment takes place routinely and is finished within a few hours. After the subsequent wound healing, the patient is usually considered to be healed. Without removing the basal cell carcinoma, it can spread unhindered in the organism. It damages surrounding healthy tissue and in the worst case can form metastases.
Older people are more likely to suffer from basal cell carcinomas than younger ones. Nevertheless, the number of sick people in young or middle adulthood is increasing significantly. The prognosis improves if the person concerned takes adequate measures to protect against direct sunlight. The older the patient and the longer they expose their skin to UV radiation, the worse the chances of recovery.
Even if a basal cell carcinoma is completely removed in a single procedure, new carcinomas can form on the skin at any time. In order to improve the chances of recovery, medical treatment should take place as soon as possible if the basaliomas form. This also reduces the risk of complications and wound infections. In addition, with regular participation in preventive examinations for skin cancer, the appearance of skin changes can be detected very early.
prevention
Particularly fair-skinned people should avoid excessive sun exposure and visits to tanning beds as a prevention against basalioma. Sunscreens with a high sun protection factor provide a certain level of protection from harmful UV rays when you are outdoors.
In families in which basaliomas occur more frequently, all family members should regularly examine themselves for suspiciously changed skin areas or take the examination by the dermatologist, the costs of which are fully covered every two years by the health insurance for patients over 35 years of age.
Aftercare
After the surgical removal of a basalioma, the operated skin area must be kept dry and clean for a few days. In general, the affected area is protected by a bandage that should only be changed by a doctor. The sutures are removed one to two weeks after the operation if the wound has healed satisfactorily.
If severe pain occurs during the healing phase, the attending physician can prescribe a pain reliever. Smoking delays wound healing and should be avoided in the initial period after the operation. Light exercise is possible once the wound has healed well; Competitive sports and other vigorous physical exertion can often only be resumed after about three months in the case of larger surgical wounds.
In the first three to six months after the operation, the operated area must not be exposed to direct sunlight, otherwise noticeable pigment disorders can occur. Even after this, sufficient sun protection must be ensured.
If the patient tends to develop basal cell carcinoma, all parts of the body exposed to the sun must be well protected from UV rays by using sunscreens with a high sun protection factor. Regular self-checks of the skin are very important in order to detect recurrence or recurrence of skin tumors at an early stage. In addition, follow-up examinations should be carried out by the treating dermatologist once or twice a year.
You can do that yourself
Basalioma is a disease in which there are some possibilities for those affected to help themselves. This applies first of all to the time after the operation. Since basaliomas are to be removed as large as possible, i.e. in healthy areas, the focus is on regeneration of the affected area after the operation.
Here the patient can actively contribute by following the doctor's rules of conduct very precisely so that the wish can heal quickly and no complications such as inflammation occur. If you experience psychological problems related to white skin cancer, it is advisable to seek advice from a support group or consult a psychologist.
Self-help in everyday life also means avoiding the occurrence of a new basal cell carcinoma. Consistent sun protection (e.g. scalp and face protection with a hat), on which the treating dermatologist provides comprehensive advice, is important. This also means that the patient informs himself exactly about the appearance of the basalioma (and also of the malignant melanoma), regularly examines his body with regard to changes in the immune system and observes the regular pre- and follow-up examinations with his doctor.
In addition to preventive measures, the patient can do a lot to calm down after the operation and any further treatments. If you want to do something good for yourself, pay attention to a healthy diet, enough drinking, adequate sleep and relaxation through methods such as yoga.

.jpg)




.jpg)

.jpg)


.jpg)