The autoimmune disease, which is also called Type 1 diabetes mellitus It is known that with 400,000 people in Germany, significantly fewer people suffer from diabetes mellitus type 2.
What is Type 1 Diabetes Mellitus?
© designua - stock.adobe.com
Even if type 1 diabetes melltius cannot be cured, the advanced medicine enables patients to lead a long life with a high quality of life.
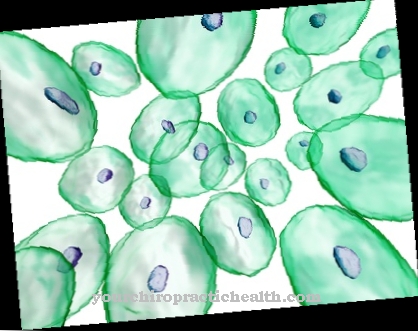
In the autoimmune disease diabetes mellitus type 1, the body's immune system turns against and destroys the pancreatic cells that produce insulin. The insulin production can no longer be continued and the hormone is absent within a very short time.
This process can have fatal consequences, because the hormone insulin is responsible for breaking down the sugar that was absorbed into the blood through food and using it for energy production. When the insulin cells are destroyed, the sugar builds up in the veins, causing the blood sugar level to skyrocket.
causes
The cause of an autoimmune disease such as type 1 diabetes mellitus is usually an autoimmune reaction (destruction of the insulin cells in the pancreas).
The reason why the immune system turns against the B cells to produce insulin is still unclear. It has so far been assumed that certain hereditary factors play a role in this process. However, this assumption has not been sufficiently proven, which is why researchers also include the environmental factors in their investigations under which an autoimmune reaction can be triggered.
According to this, the outbreak of type 1 diabetes mellitus can be significantly favored by early contact with cow's milk and some viruses.
Symptoms, ailments & signs
If around 80 percent of the beta cells in the pancreas are destroyed, the body no longer has enough insulin available to transport the sugar into the cells as an energy supplier. The first symptoms become noticeable within days or a few weeks.
The sugar that remains in the blood due to the lack of insulin is excreted by the body in the urine. An increased urge to urinate and a constant feeling of thirst are therefore typical symptoms of type 1 diabetes. In addition, the disturbed fluid balance can be reflected in dry, itchy skin as well as visual disturbances and headaches.
Since less and less sugar gets into the cells, the body falls back on the fat reserves. This can lead to rapid weight loss, but also to sweet cravings. Fatigue, weakness and difficulty concentrating are other complaints.
In addition, diabetes has an impact on the immune system, which leads to an increased susceptibility to infections and poorer wound healing. In type 1 diabetes, the urine and breath have a sour, fruity smell of acetone.
Acute symptoms are life-threatening disturbances of consciousness. The progressive lack of sugar in the cells can lead to a diabetic coma (hyperacidity), which is heralded by nausea, vomiting and deep breathing (acetone odor). Too high an insulin dose in the case of type 1 diabetes that has already been diagnosed can in turn end in diabetic shock (hypoglycaemia), which is accompanied by sudden hunger, sweating, paleness and palpitations.
course
The autoimmune disease type 1 diabetes mellitus is particularly dangerous because it is only gradually noticeable. Mostly it starts in early childhood. The symptoms can only appear years later, although the antibodies that destroy the insulin cells are detectable in the blood years before the first symptoms appear. The disease can be detected by simply measuring the sugar concentration.
With the rise in blood sugar level and evidence of glucose in the urine, the first symptoms of type 1 diabetes mellitus can also become noticeable. These would include urination, thirst, fatigue, itching, weight loss, acetone odor, gastrointestinal problems and diabetic coma.
If the body has become over-acidic due to the strong loss of fluid and a rising ketone level, this is noticeable through deep breaths to release carbon dioxide. In this condition, the patient must get medical help immediately, as the increasing dehydration of the brain causes the patient to become comatose.
If there is no therapy, the patient falls into a diabetic coma due to the lack of fluids and hyperacidity. The disease then has to be monitored in the intensive care unit and is therefore life-threatening.
When should you go to the doctor?
A doctor must be consulted as soon as at least one sugar coma (hyperglycaemia) has occurred. The same applies if you have frequent low blood sugar (hypoglycaemia). However, a general practitioner should be contacted as soon as an elevated glucose level is detected.
This is particularly advisable for children who are overweight. The development of type I diabetes mellitus can still be averted through proper nutrition and healthy weight loss. Which doctor will perform treatment depends on what caused the disease.
If there are reversible causes, a general practitioner can oversee the treatment. However, if the disease suddenly occurs e.g. due to traumatic experiences, an internist specializing in diabetes should be consulted. Only a specially trained specialist can make an exact diagnosis. The latest findings show that there is also a non-adjustable type I with mixed forms.
If it is suspected, a medical professional should be seen who is familiar with it. It is often necessary to change doctors several times. Do not shy away from this, as otherwise wrong tips and negative effects such as Weight gain and deterioration in health are to be feared.
Doctors & therapists in your area
Treatment & Therapy
If the symptoms of type 1 diabetes mellitus are recognized in good time, an adequate therapy can be used to alleviate the symptoms and restore the accustomed quality of life. Various forms of therapy are used for treatment and must be continued for a lifetime.
With conventional insulin therapy, the patient has to inject one short and one long-acting insulin preparation twice a day. Meals depend on the dose of insulin injected. To be on the safe side, the patient must undergo regular blood tests and examinations.
The intensified insulin therapy offers type 1 diabetes mellitus patients a certain amount of flexibility, because by injecting two long-acting doses, the patient can freely choose the time of his meals.
Modern insulin pump therapy makes it easier to dose the injected amount, which is injected directly into the belly fat through the catheter. Because of this, this form of therapy is particularly suitable for small children.
Outlook & forecast
Type 1 diabetes mellitus is incurable. The patients have to be looked after by a doctor for the rest of their lives, have their blood sugar level checked regularly and are dependent on the supply of insulin.
The complications that can be caused by poorly controlled diabetes are decisive for the course of the disease. Overall, women and men have an increased risk of dying prematurely from these complications compared to the normal population.
Consequential damage to the cardiovascular system such as heart attack or stroke are among the most common complications of diabetes mellitus. They make a significant contribution to reducing the life expectancy of diabetics. Another complication that can shorten life is kidney failure in diabetic nephropathy.
Good kidney function has been shown to improve the patient's prognosis. Particularly in younger years, with diabetes not yet optimally controlled, the derailment of blood sugar and its consequences are a possible cause of death. This leads to over-acidification of the blood due to a lack of insulin (diabetic ketoacidosis), which can quickly be fatal.
Overall, however, the life expectancy for type 1 diabetics has increased steadily over the last few years and decades thanks to improved medication, close controls and targeted training for those affected.
prevention
In contrast to type 2, there is no preventive measure for type 1 diabetes mellitus. But a measurement of the antibodies and the sugar concentration in the blood can predict whether someone will develop type 1 diabetes mellitus.
You can do that yourself
Type 1 diabetes mellitus is a genetic autoimmune disease that leads to the gradual destruction of insulin-producing cells in the pancreas. This means that if the disease is not recognized, the blood sugar level gradually rises to values above the norm due to the insulin deficiency and can cause consequential damage.
Self-help measures initially consist of attentive self-observation in the event that further cases of type 1 diabetes are known in the family. If symptoms occur, such as increased thirst for no apparent reason, frequent urination, weight loss and general exhaustion, it is advisable to have the blood sugar concentration measured and, if suspicion is confirmed, to arrange for a detailed examination.
If type 1 diabetes has already been diagnosed, the most important goal is to optimally adjust the blood sugar level via insulin therapy in order to avoid consequential damage to the blood vessels, in the retina, to the coronary arteries and especially in the kidneys or to heal the course of existing damage as far as possible, but at least stop. As an accompanying and supportive measure, it is recommended to set the blood pressure to the lowest possible values, especially to support kidney function.
Since type 1 diabetes, as a genetically caused disease, cannot be cured, lifelong insulin therapy is recommended, which consists of a combination of a long-acting and a short-acting insulin and is applied directly to the belly fat.















.jpg)

.jpg)