Many people will immediately raise their hands defensively when they hear or read the sentence nutrition and diet in liver disease, believing that a diet is nothing more than prohibitions. This is not infrequently due to the fact that the doctor has so far usually put a large number of foods on a prohibited list in the case of illnesses instead of first naming what is allowed and also showing the possibilities of variety in the diet menu.
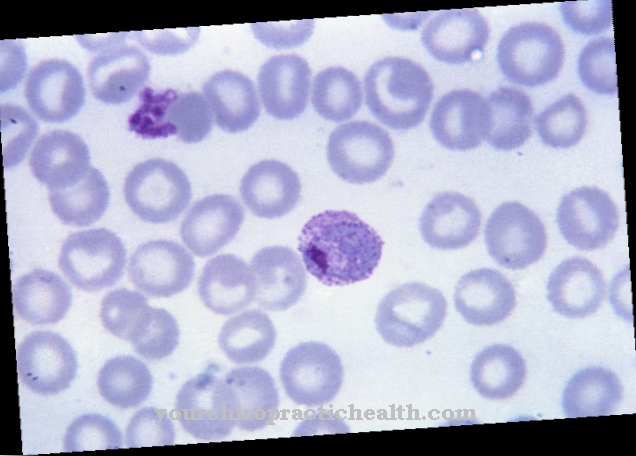
Jaundice as a typical liver disease

Liver diseases occur extremely frequently, but with precise knowledge of the metabolic processes in the liver and the ways in which they can be influenced, we can avoid or at least greatly reduce the consequences of this type of disease that were previously feared.
Nutritional treatment plays an important role in this. It should therefore be our task here to awaken the reader's understanding and attention to easy-to-use food preparation for liver disease.
Among the liver diseases, epidemic jaundice (viral hepatitis) is of great importance today. Children show an increased susceptibility to this infectious disease.However, this disease is usually mild in very young people, while in adults it often affects the function of the liver cells to a greater or lesser extent.
However, this fact does not justify trivializing jaundice in children, but requires the same careful attention to medical and dietary measures as in adults.
Course of liver disease
In the first 14 days of epidemic jaundice, the sick person feels particularly uncomfortable and often has severe symptoms in the gastrointestinal tract. The appetite is also noticeably reduced. In this acute state, the liver needs special care.
Of all foods, proteins, such as meat and sausage, also milk and cheese, as well as eggs and fats (butter, margarine, oils, lard) place a considerable strain on the liver's metabolic activity, because it is this which has to convert the proteins for the human organism. On the other hand, the carbohydrates in the food do not burden them at all.
We therefore prefer a high-carbohydrate diet for the first 14 days of the illness (often shorter, very rarely longer). This mainly means starchy products, the type of which can be changed. Oat flakes, wholemeal flours, brown rice, muesli, but also pasta, semolina and corn starch can be used, although we prefer wholegrain products because of their higher vitamin and mineral content.
All of these products can be opened up to such an extent by appropriate technical preparation in the kitchen that they only put little strain on the digestive tract. The action of carbohydrate-splitting agents (ferments) on the food begins in the mouth, which significantly relieves the strain on the stomach and intestines. Starch turns into glucose or glucose in the intestine.
Fructose split and absorbed. These types of sugar, which flow from the intestine to the liver via the bloodstream, have a nourishing and protective effect on the liver. Because of this protective effect on the liver cells, which applies equally to vitamins and minerals, grape sugar is often used to sweeten food and drinks.
Nutrition & Diet for Liver Diseases
In terms of kitchen technology, these foods are cooked in plenty of liquid, water or vegetable broth prepared without fat. In conjunction with cereal products, fruit soups and porridges can also be prepared.
Raw vegetables, a grated apple - also in connection with soaked raw oat flakes or muesli -, freshly obtained raw fruit and vegetable juices, which can also be added to cooked dishes, should be given. The fresh food is not only very digestible, but also supports the liver in resuming its full metabolic capacity.
Of the breads, the very well-tolerated crispbread made from whole grain products should be enjoyed, but stale rolls, roasted stale white bread and rusks are also possible. Bee honey, artificial honey, jam and jellies can be used as a spread.
We recommend the different types of tea as a drink. Black tea promotes blood circulation in the liver and is therefore very medically justifiable. Coffee, on the other hand, must be decidedly rejected because of its irritating effect on the stomach and intestinal walls. Alcohol must also be avoided because of its damaging effects on liver cells. The total amount of fluid should be limited to about one liter during the acute period of illness (including soups, etc.), as the liver also has a strong influence on the body's water balance.
Nutrition tips
Seasoning the food is, however, an art in itself, as we have to advise against salt when the liver is inflamed, as any inflammation in the body worsens. Therefore, only parsley and herbs of all kinds should be used. Here are some nutritional tips:
1. Breakfast:
Tea sweetened with grape sugar or malt coffee. Rusks, toast or crispbread with jam or jelly.
2. Breakfast:
A plate of oatmeal soup or muesli with fruit juice or whole grain flour soup.
Having lunch:
Barley gruel or semolina with apple compote or vegetable broth with rice. Muesli with apple for dessert.
Afternoon:
Rose hip tea with grape sugar, crispbread, rusks, toast with jam or jelly.
Dinner:
Stock semolina soup or whole wheat porridge.
Protein is important

After these pretty tough days, you can slowly switch to a mainly protein-rich diet. First and foremost, the protein of animal origin, i.e. milk, eggs, meat, is of particular importance, as they are carriers of the essential amino acids. These in turn represent the building blocks of our human protein substances and are therefore particularly important for the body's defense functions against all infectious diseases.
The more protein the blood contains, the better our body can protect itself from such diseases. But the liver cells themselves always need a certain amount of protein. As soon as this nutrient is withheld from her for a long time, she reacts very sensitively.
The goal of the jaundice sufferer's diet change that is now beginning is to provide him with a protein amount of 1.5 grams per kilogram of body weight. In other words, for a person weighing around 60 kilograms, this means 100 to 120 grams of pure protein. When putting together a protein-rich menu, it is not entirely without calculation, because every food only provides a certain amount of the necessary daily protein requirement:
An egg, for example, 10 to 14 grams and 100 grams of meat around 20 grams. But since today there are consultation options in the hospital or at the doctor for the sick person himself, the doctor or the dietician will be happy to help you with the quantity calculations. The specified amount of 100 to 120 grams of protein does not only have to be of animal origin. Some proteins of vegetable origin, grain and soy products can also be used.
Nutrition & diet
In terms of kitchen technology, there are a few things to consider with this food: the liver does not tolerate fried food at all at this time, as the liver disease also severely hampers the activity of the gallbladder and all dishes that contain roasted and fat have the highest demands on bile production and supply of bile.
The transition from the very low protein to the high protein diet must be gradual. It is therefore advisable to first prepare all soups and porridges used so far with a little milk, the proportion of which can be increased from day to day. Because protein-containing drinks can also be enjoyed, such as sour milk and butter milk, yoghurt and mixed milk drinks. The raw, uncooked or even boiled pure milk is usually poorly tolerated because of the insufficient gastric juice formation.
Quark as a protein supplier
Quark is particularly important because it can be prepared in a variety of ways and thus add variety to the menu. Quark is known to be the carrier of the most important amino acids and is therefore particularly beneficial for the liver. The daily menu should always contain around 100 grams of white cheese.
Eggs, mixed with food as raw as possible, should also be used. To do this, however, they would have to be as fresh as possible. Meat is best tolerated as scraped meat and can also be processed with raw egg yolk. Other full-fledged protein carriers are lean types of fish and meat that may not yet be fried.
In addition to cooking or cooking in your own juice, there is another way of cooking that makes the food particularly tasty: steaming, i.e. cooking with hot and humid air.
You can't do without fat
A few more words about fat as a component of food itself and as an ingredient in preparation: The main types of fat are oils (content of unsaturated fatty acids and vitamins), raw and heated, and butter. The latter is well tolerated because of its favorable melting point in the intestinal tract and is also important for the liver because of its vitamin content and as a carrier of so-called short-chain fatty acids. The total amount of fat per day should not exceed 50 to 60 grams.
Here, too, the transition from the low-fat diet to the specified amounts should only take place very slowly in the first 14 days. You should also consider that especially in sausage types, such as tea sausage and fine liver sausage, a not inconsiderable amount of fat is hidden, which must be taken into account.
If this is not taken into account, the patient is often surprised that he has complaints in overuse and that his recovery is only taking very slow steps. It is therefore best if the patient does not consume any sausage at all in the first weeks and months after the illness.
The seasoning of the food is almost the same as with the diet at the beginning of the illness. You get used to low-salt dishes very quickly if you use herbs, tomato juice or tomato paste and yeast flakes for seasoning.

















.jpg)