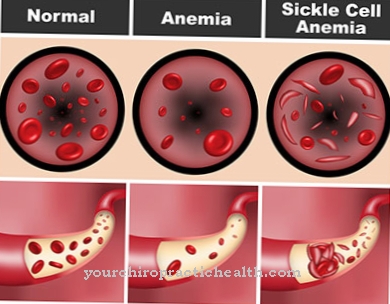
A pathological protrusion of the eyeball is called a Exophthalmos and can be traced back to many different causes. As a rule, exophthalmos is not an independent disease, but rather an accompanying symptom of an underlying disease.
What is exophthalmos?

© Neyro - stock.adobe.com
Exophthalmos is a pathological protrusion of one or both eyeballs (Bulbus oculi) from the orbit (eye socket), which can be attributed to different causes. Accordingly, an exophthalmos does not represent an independent clinical picture, but a secondary symptom of an underlying disease that is divided into six stages or degrees depending on the severity.
As the eyeball protrudes, its mobility is restricted and it is difficult or impossible to close the eyelids (grade I). In the further course chemosis (conjunctival edema) and photophobia (grade II) develop, while the bulging of the eyeball becomes prominent (grade III).
In addition, exophthalmos can manifest itself on the basis of double vision or blurred vision as a result of impairment of the orbital nerves and eye muscles (grade IV), xerophthalmia (desiccation of the cornea) and / or lagophthalmos (desiccation of the eyeball) as well as inflammation and ulceration (ulceration) of the cornea (grade V). With pronounced involvement of the optic nerve (optic nerve), an exophthalmos can lead to visual defects or even loss of vision.
causes
An exophthalmos can be traced back to various causes as a secondary symptom of the individual underlying disease. Endocrine exophthalmos is caused by autoimmune diseases such as Graves' disease or Hashimoto's thyroiditis, in which autoimmune-induced processes can lead to inflammation of the orbital adipose tissue and swelling of the retrobulbar (behind the eyeball) structures, so that the eyeball is pushed forward .
As a result of trauma, the orbital arteries and veins may short circuit, causing the eyeball to pulsate and protrude (unilateral exophthalmus pulsans). Blunt trauma can lead to exophthalmos via a retrobulbar hematoma.
In addition, an orbital phlegmon (bacterial inflammation of the eye socket), which is associated with a diffuse inflammation of the orbit and swelling of the orbital structures, as well as orbital tumors (including hemangioma, neuroblastoma, retinoblastoma) can push the eyeball forward due to their growth, so that a Exophthalmos arises.
Genetically determined or acquired varicose veins (varicose veins) in the orbital area can cause a so-called exophthalmos intermittens through blood congestion. In addition, myopia (pronounced nearsightedness), dyscrania (skull malformations) as well as aneurysms and thromboses of the cerebral veins can trigger exophthalmos.
You can find your medication here
➔ Medicines for eye infectionsSymptoms, ailments & signs
First and foremost, the exophthalmos results in strongly protruding eyeballs. These have a very negative effect on the aesthetics of the person concerned, so that many patients with exophthalmos also suffer from depression or other psychological complaints and moods. The quality of life of the person affected is significantly reduced by the disease.
Often times, the disease also leads to pain in the eyes and various visual disorders. It comes to a veiled vision or double vision. In general, the disease also has a negative effect on the eyesight of those affected, so that the patients are dependent on glasses in their everyday life. The eyes of the person affected appear very dry due to the exophthalmos, whereby the cornea in particular dries out.
The cornea can also become inflamed. If this inflammation is not treated, the affected person can become completely blind. Whether the disease can be treated easily or not, however, depends very much on the underlying disease. As a rule, the causal disease is also associated with various symptoms and complaints, although no general statement can be made about this. However, the life expectancy of the patient is not negatively affected by the disease.
Diagnosis & course
In the course of a clinical examination of the eyes, the extent of the exophthalmos and a possible difference between the sides, which enables initial indications of the cause, can be determined.
With the help of an exophthalmometer, the progression of the protrusion can be determined. The orbital structures as well as any inflammation or tumors can be made visible through imaging methods such as computer and resonance tomography as well as sonography and X-ray examinations. A blood analysis with determination of the thyroid values (including thyroxine, TRH, autoantibodies) or inflammation markers (including leukocytes, C-reactive protein) enables conclusions to be drawn about a thyroid disease or existing inflammation (orbital phlegmon).
In addition, arteriovenous short circuits can be diagnosed as part of an auscultation (diagnostic recording of the pulse-synchronous noise). Course The prognosis and course of an exophthalmos depend largely on the underlying disease and its therapeutic success.
When should you go to the doctor?
An exophthalmos must always be examined and treated by a doctor. This disease does not heal itself, so that a doctor must be consulted in any case. The doctor should then be seen if the person has eye pain. Protruding eyeballs can also indicate exophthalmos and should be examined. Various visual disorders, such as double vision or blurred vision, can also indicate this disease.
If these visual problems occur suddenly and cannot be alleviated by visual aids, an examination must be carried out by a doctor. Dry eyes can also indicate the disease. Inflammation of the cornea is also a symptom of exophthalmos and must also be examined. As a rule, the ophthalmologist is consulted with this disease.
If it is an emergency, the nearest hospital can also be approached. Further treatment of the disease is also carried out in a hospital. Most of the time there is a positive course of the disease and no further complaints. In most cases, the life expectancy of the patient is also not negatively affected.
Doctors & therapists in your area
Treatment & Therapy
In the case of exophthalmos, the therapeutic measures are based on the underlying disease causing it and aim to avoid complications such as malignant exophthalmos, corneal ulcerations, conjunctivitis or glaucoma (glaucoma).
If the exophthalmos is preceded by an orbital phlegmon or an abscess (accumulation of pus in the tissue), these can be treated with antibiotics. If necessary, these should be opened for relief and emptied as part of a surgical procedure. Retrobulbar adipose tissue and tumors, which, as they grow, push the eyeball forward, can also be surgically removed.
In some cases, tarsorrhaphy may also be necessary. Here, the eyelid fissure is surgically reduced with the help of a temporal suturing of the lower and upper eyelids in order to ensure that the eyelids close and accordingly to avoid damage to the cornea or the eyeball (e.g. drying out).
In order to avoid drying out and structural impairment of the cornea, we also recommend consistent eye care and artificial moistening of the eyes with synthetic tear fluid. If an exophthalmos results from underlying diseases such as Graves' disease or a thyroid disease, these must be treated appropriately and specifically in order to induce permanent regression of the protrusion.
Outlook & forecast
The prognosis of an exophthalmos always depends on the underlying disease and the right treatment. In some cases, the exophthalmos can completely regress if the underlying disease is treated successfully. Among other things, abscesses behind the eyeballs are treated with antibiotics and sometimes surgically.
Tumors in the eye socket must be surgically removed. If an overactive thyroid in Graves' disease is responsible for the protruding eyeballs, this must be treated as a matter of priority. However, the eyes should also be artificially moisturized and cared for to avoid dehydration.
Without these measures, corneal ulceration can occur. In severe cases, the optic nerve is also affected. This can lead to visual failure or even complete loss of vision. Conjunctivitis, increased intraocular pressure (glaucoma) or even a malignant exophthalmos can occur as further complications.
Malignant exophthalmos is characterized by a painful and progressive protrusion of the eyeballs. As a result, the eyelid closure is disturbed. The cornea dries out very badly. If left untreated, exophthalmos seldom resolves on its own. Most of all, irreversible eye damage then occurs.
With successful treatment of the underlying disease and intensive eye care at the same time, an exophthalmos can heal without consequences. Eye care consists primarily of moistening the eyes with artificial tear fluid.
You can find your medication here
➔ Medicines for eye infectionsprevention
Exophthalmos cannot always be prevented. However, underlying diseases such as Graves' disease or thyroid diseases should be treated consistently in order to minimize the risk of developing an exophthalmos.
Aftercare
Follow-up care options are in most cases not available to those affected by exophthalmos. In any case, the disease must be treated correctly by a doctor, as it severely restricts the everyday life of the person affected and also significantly reduces the patient's quality of life. To prevent further complications, early treatment of the exophthalmos is very important.
However, the underlying disease should also be treated in order to completely alleviate the complaint. The treatment itself is mostly supported with the help of antibiotics. Those affected should ensure that these medications are taken correctly and regularly. Side effects or other interactions with other drugs may also have to be taken into account, although a doctor should be consulted.
When taking antibiotics, alcohol should be avoided so as not to weaken their effect. Furthermore, many patients are dependent on artificial humidification of the eyes in order to treat the symptoms of exophthalmos. The eyes should be moistened regularly to prevent the cornea from drying out. Most of the time, the disease can be treated relatively well without reducing the patient's life expectancy.
You can do that yourself
In most cases, it is unfortunately not possible to help yourself with this disease. It is also not possible to prevent the disease in all cases.
This is especially the case if the complaint and a complication or a sequela of another illness are involved. The underlying disease must be properly treated and treated. As a rule, an ophthalmologist should always be consulted in order to avoid further complaints or visual impairment.
Since the disease itself is treated with the help of antibiotics, these drugs must be taken as directed. Other drugs or alcohol that may decrease the effectiveness of the antibiotic should not be taken. Care should also be taken to care for the eyes and skin, as these dry out in many cases. Different ointments and creams can be used, which lead to the desired success.
In the case of a tumor there is unfortunately no possibility of self-help. If thyroid disease is suspected, appropriate diagnosis and therapy are necessary. Furthermore, surgical interventions that cannot be replaced by self-help options may also be necessary.

.jpg)
.jpg)