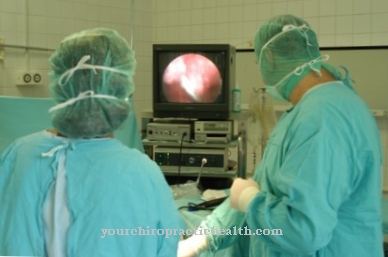
A Skin graft Is used for burns, chemical burns or ulcers to cover damaged skin. The skin used comes from the same patient. It is usually taken from the thigh, stomach or back. The aim is to treat wounds that, due to their size, do not heal through conservative measures.
What is the skin graft?

Skin grafting is the most common plastic surgery procedure. In order for the wound to be treated in this way, on the one hand it must be free of all bacteria and other pathogens, and on the other hand skin areas should be available that are suitable for a transplant. Healthy tissue is a prerequisite.
Numerous operations have shown that the result is most aesthetically perceived when the transplanted skin is as close as possible to the actual injury. If operations and other medication can no longer resolve the wound, a skin graft must be carried out within a short time window. This can prevent infections from developing.
Normally, the body is able to heal any damage to the skin on its own. However, once the wound has reached a certain size, it is a process that takes a long time and is susceptible to bacteria. The skin itself is an important part of the human body. On the one hand, it is the largest organ and, on the other hand, it protects the organism from heat, dirt and pressure.
Function, effect & goals
There are different methods of transplanting skin areas. Full-thickness skin and split-thickness skin transplants are used particularly frequently. Both are initially based on donor tissue from the same person who has a large-scale injury. If this does not have healthy areas of skin, cells from other people can also be transplanted.
In such a case, it is a question of foreign skin grafts. At the latest when 70 percent of the skin surface is damaged, it is no longer possible to remove your own skin areas. The skin has several layers: upper skin (epidermis), leather skin (dermis) and subcutaneous tissue (subcutis). Doctors remove the epidermis and dermis as part of a full-thickness skin transplant. The skin appendages remain intact. These are, for example, hair follicles and sweat glands. In comparison to split-thickness skin grafts, areas are removed that are relatively thick.
After the tissue has been removed, the wound must be closed. In most cases, a suture is used for this. The healing of the extraction region often results in scarring. It is not suitable for any further skin grafting after the first removal. Full-thickness skin grafts are particularly used for wounds that are small and deeply seated. The result is perceived as better than that of a split-thickness skin graft, both aesthetically and functionally. The split-thickness skin graft is limited to the epidermis and the upper dermis. Their thickness is approximately 0.25 to 0.5 millimeters. In the case of a split-thickness skin graft, the region of the removal usually heals within 2 to 3 weeks. The same area can be used for several operations at the same time; no scar develops in the further healing process.
Whilst full-thickness skin grafts are only suitable for wounds that are free of bacteria and have a good blood supply, the existence of such requirements is not mandatory for a split-thickness skin grafting. Another method is to grow your own skin. Some cells are taken from the patient. On this basis, a flap of skin can be grown in a laboratory. Such a procedure takes about 2 to 3 weeks and can therefore not be used in acute accidents that require quick action.
During the operation itself, the healthy area of skin is fixed with clips, sutures or fibrin glue. In order for the wound secretion to drain, the tissue must be cut through in some places. The operation ends with the application of a compression bandage and immobilization. This is particularly important to enable the skin to grow together properly.
Risks, side effects & dangers
Transplants obtained from the recipient pose no risk of rejection. However, there are some risks that need to be considered. After an operation, bacteria or other pathogens can accumulate in the area of the newly sewn area and trigger an infection. Infections can occur with autologous skin transplants as well as with foreign skin transplants.
Bleeding during or after the operation cannot be ruled out. In addition, healing disorders or delayed growth can arise. These usually develop if the wound was not adequately supplied with blood during the operation. If the attending physician has not applied or sutured the transplant optimally, this can result in further growth delays because the contact between the skin and the transplant may be broken. After healing is complete, the occurrence of numbness in the transplanted area cannot be excluded.
If a large-area transplant has been carried out, the patient's movement may be restricted by the scarring. Furthermore, the lack of hair growth can be observed in some cases. How high the individual risk is ultimately depends on several factors. These include above all the age of the patient as well as all secondary diseases and conditions that cause more or less good wound healing. Accordingly, the risk is increased, especially in people over 60 and young children. Further caution applies to diabetics, immune disorders, anemia and chronic infections.


















.jpg)

.jpg)