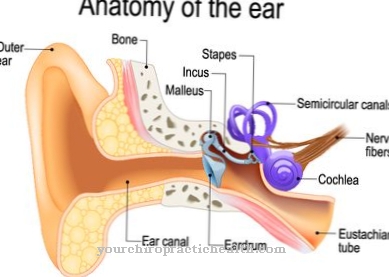
With the non-invasive Brain stem audiometry the neurologist or ear, nose and throat doctor carries out an objective measurement of hearing performance under auditory stimulation based on impulses from the auditory nerve tract, which can be followed up to the middle brain stem.
This method is one of the few methods for the objective assessment of hearing performance that can also be carried out on small children or otherwise unwilling patients. The test method is used in particular for the differential diagnosis of cochlear and retrochlear damage to the hearing, in assessments and as part of the ERA, a hearing screening in newborns.
What is brain stem audiometry?

The brain stem audiometry is also under the term BERA (brainstem evoked response audiometry) and is a non-invasive method for hearing testing. It is a neurological and ENT medical examination method that is primarily intended to help with the differential diagnosis of hearing disorders.
In principle, with the method under acoustic stimulation, the brain waves are measured to assess the objective hearing ability. The impulses of the auditory nerve tracts are tracked through a targeted transmission of stimuli to the middle brain stem and registered and recorded as individual waves. The evaluation of the measurement data relates to the latency period of the waves, which can, under certain circumstances, provide information about the origin of hearing damage. The recorded data from brain stem audiometry are therefore mostly used for differential diagnosis in the case of hearing disorders, but can also be collected during a general hearing screening.
Function, effect & goals
The ear, nose and throat specialist or neurologist uses brain stem audiometry primarily for differential diagnosis. A disturbed hearing function, which can be recognized by disturbed brain waves, could, for example, indicate hearing damage from multiple sclerosis or a tumor on the auditory nerve.
The most common tumors of this type are, for example, the acoustic neuroma and the cerebellar bridge angle tumor. In terms of differential diagnosis, BERA can be used to distinguish between cochlear and retrochlear damage to the hearing. Another area of application for the objective test procedure is the appraisal system. With BERA, hearing thresholds can be recognized entirely without the assistance of the patient and can thus also be determined for children who defend themselves against the test.
Even the hearing screening of newborns can be carried out using brain stem audiometry. The basic principle of BERA is ultimately always the graphic representation of electrical potentials in wave form. Five to six waves are recorded during the exam. This recording only occurs when acoustic stimuli are successfully processed. The potentials shown thus illustrate normal or disturbed activity of the auditory pathway. Electroencephalography (EEG) derives the potentials during acoustic stimulation with a latency time of greater than or equal to 10 ms between the center of the vertex and the mastoid.
To do this, three adhesive electrodes are attached to the patient's head. He wears an electrode on both sides behind the ear and a neutral electrode on the middle of the forehead. The acoustic stimulation takes place by means of clicks that are given via headphones at regular intervals of 20 seconds. The response potential is derived and added up via the electrodes, while other EEG signals are filtered out. Ultimately, only the brainstem's response to the acoustic click signals is displayed.
The waves I, III and V can usually be clearly recognized and are therefore suitable for determining an absolute latency to an acoustic stimulus. In addition, a so-called inter-peak latency is recorded. This is a latency difference between multiple waves that can provide information about retrocochlear processes. In adults, for example, inter-peak latencies with latency times greater than or equal to 4.4 ms in waves I to V provide an indication of retrochlear damage from MS or tumors. For small children, a delayed latency period is generally considered the norm.
Risks, side effects & dangers
Since BERA does not require the patient's assistance and can even be carried out in an anesthetized state, this method is one of the few hearing measurement methods that can also be performed on unwilling patients such as children.
The BERA is often used as one of three components of the ERA (Evoked response audiometry) and is completed by ECochG and CERA. While the former measures the potentials of the cochlea and auditory nerves, the latter measures the potentials of the cerebral cortex. With an extensive hearing screening, all hearing-relevant potentials are recorded with ECochG, CERA and BERA. For adults, brainstem audiometry is usually not associated with any additional precautions.
Before the measurement, however, the patient must take part in an extensive discussion that is intended to ensure that the measurements are correct. In this conversation, patients are given precise rules of conduct for the period of measurement. For example, if you do not lie relaxed or move more, this can significantly falsify the results. Newborns and children usually have to be anesthetized for the measurement, as they rarely behave completely calmly.
Patients who are otherwise unwilling are also anesthetized. As a rule, complications are not to be expected. When anesthetized during the measurement, however, there is always a risk, as the anesthesia itself is slightly risky. After the measurement, no special precautions need to be taken and the patient can go home.Depending on the evaluation findings, however, additional diagnostic procedures may be indicated in the following weeks that further secure or exclude a possible diagnosis.
You can find your medication here
➔ Medicines for earache and inflammation






.jpg)

.jpg)


.jpg)