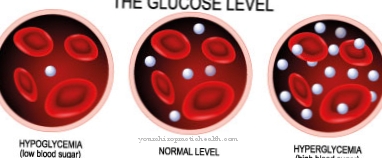
Diabetics can not only suffer from high blood sugar, but also low blood sugar. If the level is extremely low and therefore unconsciousness occurs, experts speak of one hypoglycemic shock (colloquial: hypoglycaemia). This can be life threatening.
What is hypoglycemic shock?

© feelartfeelant - stock.adobe.com
In diabetics, the blood sugar level can fluctuate greatly for various reasons. If the value falls below 40 to 50 mg / dl, there is acute danger. This happens when there is too much insulin in the blood.
Since the brain needs glucose to maintain vital functions, such a condition can be extremely dangerous. If the patient passes out, it is a coma. But hypoglycaemia announces itself in advance:
Those affected are pale, sweaty, have cravings, may have seizures, tremors, are restless and possibly mentally conspicuous, which can be expressed in agitation, confusion or hallucinations. The pulse beats faster and the blood pressure is increased. If a hypoglycemic shock occurs, action must be taken even more quickly than in the case of a diabetic coma.
causes
The question is: How does such a dangerous hypoglycaemia come about? One possibility is that a diabetic has overdosed his blood sugar lowering medication or insulin.
Hypoglycemic shock can also occur if those affected eat too little (especially carbohydrates) or exercise too much without adjusting their insulin or medication administration. For this reason, an optimal dose adjustment is essential. Excessive alcohol consumption, on the other hand, can also become critical for people without diabetes. Because the liver is busy breaking down alcohol, it may not be able to produce enough glucose (grape sugar) and the brain will become deficient.
Even then, hypoglycaemia occurs. But even with excessive consumption of foods with a high glycemic index, which trigger high levels of insulin, the blood sugar level can drop rapidly as a result.
Symptoms, ailments & signs
Hypoglycemic shock is characterized by the sudden onset of a coma. It is a life-threatening condition that needs immediate treatment. Treatment consists of giving glucose in the form of grape sugar or, if unconscious, in the form of an infusion. In addition to the coma, there is a tendency to convulsions and increased reflex readiness.
In addition, there is profuse sweating and damp and pale skin. In addition, palpitations often occur. In contrast to a diabetic coma, however, the symptom of complete dehydration is absent. Since the coma in a hypoglycemic shock does not otherwise differ from a diabetic coma, a distinction can only be made between the two disease states by means of the signs that occur.
Very low blood sugar levels are found in laboratory tests. In addition, the hypoglycemic shock is heralded by various symptoms that occur even with moderate hypoglycaemia. These are symptoms that can also occur with other diseases. In connection with diabetes, however, they provide valuable information about possible impending unconsciousness.
These signs include sudden restlessness, food cravings, difficulty concentrating, dizziness, nervousness, visual disturbances, panic, tremors or palpitations. In addition, there are perceptual disorders, difficulty speaking, tingling, cold sweats, soft knees and a furry taste in the mouth. Symptoms resolve immediately after the administration of glucose.
Diagnosis & course
Life-threatening hypoglycemia can last for hours and days. This is the clinical problem. It is first announced by symptoms of the autonomic nervous system and the central nervous system.
Cravings, sweating, nausea, tremors, vomiting as well as headaches, poor concentration, increased irritability and confusion are the first signs. If the blood sugar level drops even further, primitive forms of expression such as smacking, grimacing and grasping can occur.
This is followed by speech disorders, double vision, seizures, paralysis and breathing and circulatory problems. Finally, hypoglycemic shock occurs in the form of unconsciousness. The victim falls into a coma. The symptoms progress very quickly. For this reason, diabetics need to watch themselves closely. The blood sugar level must be checked at the first signs.
Complications
Typically, this shock comes with a number of different ailments and symptoms. The affected person suffers primarily from vomiting and severe nausea. There is a general feeling of illness and the patient usually feels tired and exhausted. Physical stress or sporting activities are no longer possible, so that there is a strong reduction in the quality of life.
Furthermore, there is tremor all over the body and sweating. The affected person also often suffers from disorders of coordination and concentration. The patient may also subsequently become unconscious if symptoms are severe. If the shock is left untreated, death usually also occurs. If it comes to unconsciousness, the patient can be injured if he falls.
The shock is usually treated by importing glucose and leads to a positive course of the disease relatively quickly. There will be no further complications if treatment is quick and early. However, the patient can suffocate if he loses consciousness and no other person is helping.
When should you go to the doctor?
Mild hypoglycemic shock usually goes away on its own as soon as a small meal with enough carbohydrates is consumed. In contrast, severe hypoglycaemia must always be treated by a doctor. If the person is still conscious, their glucose or an appropriate emergency medication can be administered. The measures must be repeated every 15 minutes until the blood sugar level is stable again or a doctor arrives.
If you are unconscious, call the emergency services immediately. Until professional help is available, the person concerned must be given the necessary active ingredient (e.g. glucagon or glucose) intravenously. Hypoglycemic shock must always be discussed with the responsible doctor. The medical history is necessary to determine the cause of the hypoglycaemia and to adjust the therapy accordingly. In addition, if necessary, the doctor may prescribe a stronger drug to prevent future seizures. A disturbed perception of hypoglycaemia may also be the cause, which must be recognized and treated with medication.
Doctors & therapists in your area
Treatment & Therapy
If hypoglycemic shock is imminent, countermeasures should be taken immediately. If the blood sugar level turns out to be too low, the person concerned has to take glucose immediately.
One possibility is to place one to four tablets of glucose between your teeth and cheek. The glucose slowly dissolves and gets into the bloodstream. The patient, who is still conscious, may also consume other high-carbohydrate foods that raise blood sugar levels quickly. Sugary drinks like fruit juices are also an option. Light drinks, on the other hand, should be avoided because they lead to even more insulin being released and thus further reduce the blood sugar level.
If these measures are not sufficient, an intravenous glucose infusion is indicated. This applies when the patient is already unconscious because the swallowing reflex no longer works and aspiration can occur. It is also possible for the emergency doctor or rescue service to deliver glucagon intramuscularly, optionally also into the subcutaneous fatty tissue. The latter, however, does not work with excessive alcohol consumption. If hypoglycemia occurs, an emergency doctor must be notified immediately. Glucose infusions or intramuscular delivery of glucagon should only be performed by specialists.
prevention
So that threatening hypoglycaemia does not occur in the first place, the best prevention is to adjust the insulin and medication administration exactly to the needs of the body. This applies when a patient eats less and exercises more as part of a diet or consumes less in everyday life and moves more.
Both the type and amount of food and exercise are factors that a patient should keep in mind. Eating too little, eating too much, or eating with a high glycemic index are not good options for those affected.
A diabetic should therefore constantly monitor his blood sugar level in order to be able to intervene quickly before the blood sugar level drops too low. He should also be very careful when administering insulin or medication. For fear of the consequences of diabetes, many sufferers tend to inject more than necessary. The exact dose adjustment of insulin or medication is therefore best carried out by a doctor.
Aftercare
Hypoglycemic shock is associated with type 2 diabetes mellitus. Follow-up care is closely linked to lifelong medical care. For the patients, this means that they have to attend regular check-ups with their doctor after they have stopped taking their medication. Here the blood values are checked to follow the development.
Patients can also measure their values themselves and improve their health by making certain changes in their lifestyle. Switching to a balanced diet is a very important point in this context. Appropriate training, i.e. participation in a nutrition course, may help.
With more health awareness and a nutritionist, diabetes patients can eat more vitamins and less fat. This gradually leads to a better body feeling. In addition to the nutritional advice, which should be renewed occasionally, there are also other appointments. The ophthalmologist should be visited once a year and the podiatrist will also determine any deterioration early on.
This prevents the diabetes from causing visual problems or problems with the feet. The disease itself can neither be stopped nor cured, but the process can be slowed down. The right way of life helps, which the patient should discuss with the doctor and a nutritionist.
You can do that yourself
In the case of slight hypoglycaemia, it is sufficient in most cases if the person concerned consumes plenty of glucose and carbohydrates. A glass of lemonade or a few crackers will balance blood sugar levels and ease the discomfort.
Hypoglycemic shock must definitely be treated by a doctor. An emergency doctor is urgently needed. Insulin should not be injected in this situation. If the person concerned is conscious, he should sit down, put his legs up and drink enough water (at least one liter per hour).Physical exertion must be avoided for the time being. In addition, blood sugar levels should be checked every two hours. If the blood sugar level does not return to normal after six hours, the person concerned must be taken to the hospital. In the event of unconsciousness or vomiting, first aid must be given immediately until the emergency doctor arrives. The diabetic must be brought into the stable lateral position and non-fixed dentures must be removed. If available, glucagon should be injected.
After a hospital stay, the person concerned has to take it easy for a few days. In addition, the cause of the hypoglycemic shock should be determined so that further complications can be avoided in the future.





.jpg)

.jpg)


.jpg)