As Insulin release or insulin secretion is the secretion of the vital hormone insulin by the pancreas (pancreas).
What is the insulin release?

Insulin is only produced in the beta cells of the islets of Langerhans located in the pancreas, from which its name is derived. The release of insulin is stimulated by an increased glucose content and, to a lesser extent, by free fatty acids and some amino acids, as well as by gastrointestinal hormones.
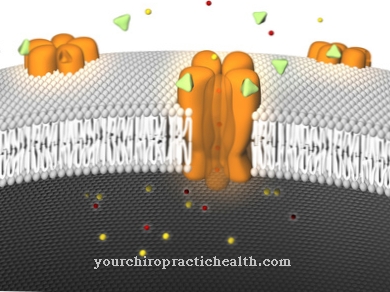
The trigger causes more adenosine triphosphate (ATP) to be formed in the beta cells, which leads to a blockage of potassium-dependent channels. This enables calcium ions from the extracellular space to penetrate better into the beta cells and activate insulin release.
Insulin vesicles then fuse with the cell membrane of the beta cell and empty into the extracellular space (process of exocytosis). Insulin begins to be released.
Insulin is not released evenly, but in bursts. The beta cells release insulin into the blood approximately every 3 to 6 minutes.
Function & task
Insulin ensures that the body's cells absorb glucose from the blood for energy conversion. In this function as a link between sugar and cells, the insulin ensures that the blood sugar level remains within the normal range and does not increase.
It is the only hormone that is able to lower blood sugar levels. Its counterpart, glucagon, and, in moderation, cortisol, adrenaline and the thyroid hormones increase the sugar content in the blood.
When the body eats foods rich in carbohydrates, it converts them into sugar, which increases blood sugar levels. In response to this, the beta cells release more insulin. This helps the glucose from the blood to get through the cell walls into the cell interior, whereupon the glucose content in the blood plasma is reduced. The glucose is then either stored in the body's cells as glycogen or immediately converted into energy.
The glycogen is stored inside the cell until there is an acute need for energy. Then the body falls back on the glycogen stores and converts them into the energy it needs.
The central step of this conversion, called glycolysis, takes place in ten individual steps. During this, the glucose is split into lactic acid and ethanol with the help of the nucleotide adenosine triphosphate and prepared for further energy conversion.
The liver and muscle cells in particular can absorb and store large amounts of glucose. They respond particularly well to the action of insulin, as their cell membranes become more permeable and more accessible to glucose when there is increased insulin release.
In contrast, nerve cells take up glucose from the blood independently of the insulin release. If the insulin-dependent cells take in more glucose when the insulin level is increased, the nerve cells can experience an undersupply of glucose, since in this case too little glucose remains for them. In the case of severe hypoglycaemia (low blood sugar levels) there is therefore the risk that the glucose-dependent nervous system can be damaged.
If the blood sugar level falls below a value of around 80 mg / dl, the aforementioned opponents adrenaline, glucagon or cortisol are used to increase blood sugar. The body's production of insulin is greatly reduced during this time.
Illnesses & ailments
Diabetes mellitus is the generic term for various disorders in the body's handling of insulin. In type 1 diabetes, the body is no longer able to produce insulin itself. The immune system destroys the insulin-producing beta cells and ultimately leads to an insulin deficiency.
The glucose in the blood can then no longer get into the cells and they are lacking as an energy supplier. After a certain period of time, there is a lack of energy in the body's cells, an increase in blood sugar, a loss of nutrients and water and an over-acidification of the blood.
Type 1 diabetes is usually treated with artificially manufactured insulin preparations that are administered subcutaneously in the form of syringes or with the help of an insulin pump. The exact cause of type 1 diabetes has not yet been clarified. One now assumes a multifactorial process in which both genetic and environmental influences are involved.
In type 2 diabetes, the body can still produce the insulin itself, but this can only have a limited effect due to the insulin resistance in the cells.
Type 2 diabetes often develops over a long period of time. It can take several years for absolute insulin resistance to be achieved and an actual diagnosis of type 2 diabetes. In the beginning, the body can compensate for the decreased processing of insulin in the cells by increasing insulin production. However, the longer the disorder persists, the worse the pancreas can keep up with production and the blood sugar can no longer be regulated. Eventually, type 2 diabetes becomes manifest.
Type 2 diabetes is also said to have multifactorial causes. In contrast to type 1, however, obesity is the first possible trigger for him. A freshly manifested type 2 diabetes is therefore often first tried to be treated with a diet. However, genetic factors can also be the cause of type 2. In this case, or if type 2 diabetes persists after weight loss, it is treated with tablets.
Another, but much rarer disease associated with insulin is so-called hyperinsulinism. Here too much insulin is produced due to overproduction of the beta cells. Frequent low blood sugar levels (hypoglycaemia) are the result.







.jpg)

.jpg)


.jpg)