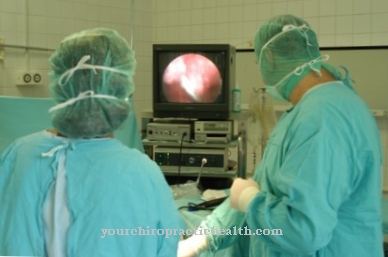
The Intensive care deals with the diagnosis and therapy of life-threatening diseases and conditions. It is closely linked to emergency medicine, as intensive medical measures are used to maintain vital functions. The primary concern is to preserve the patient's life, with the diagnosis being secondary for the time being.
What is intensive care medicine?

In Germany, intensive care medicine has not been clearly delimited until now, as it did not include a separate specialist area, but was assigned to the various sub-areas of anesthesia, surgery, internal medicine, neurosurgery, neurology, pediatrics and cardiac surgery. There is now an “interdisciplinary specialist in anesthesia and intensive care medicine”.
The health sector has a growing number of intensive care centers for intensive therapy, anesthesia, intensive care and intermediate care. They operate under the specialist name “Clinic for Anesthesia and Intensive Care”. The nurses have the specialist training "nurse for anesthesia and intensive care medicine".
Treatments & therapies
The three main aspects of intensive care medicine are monitoring, ventilation and invasive procedures. The monitoring records the vital functions of the patient by creating and recording their physical data. This includes the monitoring of cardiac activity, blood pressure, oxygen saturation in various compartments, intracranial pressure (ICP), central nervous pressure (CVP) and pulmonary artery pressure (PAP).
The laboratory controls are closely meshed and immediately recognize malfunctions, to which the medical professionals can react quickly. The ventilation is connected to the airway protection. It is done through tracheotomy or endotracheal intubation. Invasive procedures are the prerequisite for creating access to body cavities and vessels. They are used in organ replacement procedures such as dialysis, extracorporeal oxygenation and continuous monitoring. The intensive medical doctors and nursing staff work in the intensive care unit, in anesthesia, pain therapy, emergency medicine, intermediate care, in the ambulance service and in the emergency room.
Patients who show a life-threatening condition or whose condition is expected to become threatening are admitted to the intensive care unit. Not only serious illnesses lead to intensive medical monitoring and therapy, but also conditions following highly invasive operations. In general, a favorable prognosis must be given, since the goal is to restore vital functions and the associated health, or to achieve a largely autonomous state for the patient. Terminal conditions and diseases do not lead to the intensive care unit, but to palliative medicine.
Intensive care medicine treats elementary disorders of breathing, the electrolyte balance, hemostasis (blood clotting), various states of shock (septic, anaphylactic, hypovolemic, cardiological) and severe disorders of consciousness. Also for complex clinical pictures such as poisoning, general infections, head trauma, peritonitis, inflammation of the pancreas, neurological diseases (e.g. stroke, severe meningitis, cerebral bleeding, myastic crises, subarachnoid hemorrhage, delirium tremens), heart disease, multiple organ failure and kidney disease and lung failure are the responsibility of the intensive care physicians.
Diagnosis & examination methods
All imaging and endoscopic procedures (x-rays, ultrasound, magnetic resonance imaging, CT) are used to confirm the diagnosis. Intensive care medicine is not synonymous with device medicine. Rather, doctors and medical specialists from different medical professions work together to care for patients. In addition to treatments and therapies that are also known from normal wards, intensive care medicine uses a large number of modern devices to implement its treatment concept.
So that the intensive care physicians can monitor the vital functions of their patients such as heart rate, oxygen content, breathing, brain activity, circulation and the activity of other organs, they are connected to monitoring devices (monitors). The vital functions are recorded by measuring sensors in the form of electrodes and sensors, which forward this data to the monitoring monitor via wiring. There the recorded data is evaluated and displayed as a curve. The monitoring devices have acoustic and optical alarm signals. For safety reasons, these intensive medical devices react to the smallest changes. In addition, there is regular and personal monitoring by the doctors and nursing staff.
Infusion lines are further important instruments in intensive medical care, as many patients require medication or artificial nutrition. This supply takes place via the infusion therapy. So that the appropriate medication can be administered, the physicians insert a catheter into the patient's vein. The nutritional solutions and medication are supplied to the organism via plastic pipes. Patients who cannot ingest their food on their own are fed through a gastric tube. These feeding tubes are inserted into the stomach through the esophagus. Many intensive care patients need a urinary catheter for urine drainage at times. The urine is passed through the catheter into a thin plastic tube, which ensures that the urine is safely drained into a collecting basin. Ventilators help the patient breathe.
The patient is connected to the ventilator via a tube (ventilation hose) that is placed through the mouth into the windpipe. In this way, the oxygen from the ventilator reaches the lungs. The patient cannot speak during this pulmonary supply.However, if he is conscious and approachable, communication via sign boards or sign language is possible. Hemodialysis and hemofiltration devices (artificial kidneys) are used in patients with impaired kidney function. They replace the disturbed natural kidney function and enable the necessary blood washing. These devices remove waste products, excess fluids, drug residues and other pollutants from the body. The connection between the device and the patient's blood circulation is made via catheters which feed the blood into the device for cleaning and from there back to the patient.
These invasive monitoring methods are supplemented by the non-invasive monitoring of the cardiovascular system by means of EKG and blood pressure monitoring as well as the measurement of body temperature and oxygen saturation. This must be distinguished from the invasive measuring methods of central venous pressure, arterial blood pressure measurement and pulmonary artery catheters. Laboratory machines also help doctors collect frequently required values such as acid-base status, blood gases, hemoglobin and electrolytes in point-of-care testing.
Intensive care physicians use analgesics (painkillers), antiarrhythmics (trachycardiac arrhythmias), antidotes (antitoxin, antidote), infectious narcotics, catecholamines (adrenaline, dopamine), relaxants, sedatives (relaxing drugs), antihypotonic drugs (antihypertensive drugs), local anesthetics (against low Blood pressure) and antispasmodics / vagolytics (Buscopan, atropine sulfate). Patients in intensive care facilities are exposed to a ten times higher risk of infection than patients in normal wards. Favoring factors are age, the underlying disease, concomitant diseases, poor nutritional status and impaired consciousness.
On the therapy side, a large number of measures can break the patient's immune barrier. Therefore, there are extremely high demands on a sterile and aseptic environment. For this reason, the stations are equipped with a lock system in which staff and possibly permitted visitors change their clothes.
Medical personnel wear a face mask to ward off droplet infections and special area clothing. The hands represent the largest reservoir of transmission and must therefore be one hundred percent sterile. Patients with an attacked immune system are taken to special isolation wards. All devices used must also be completely sterile and germ-free.














.jpg)

.jpg)