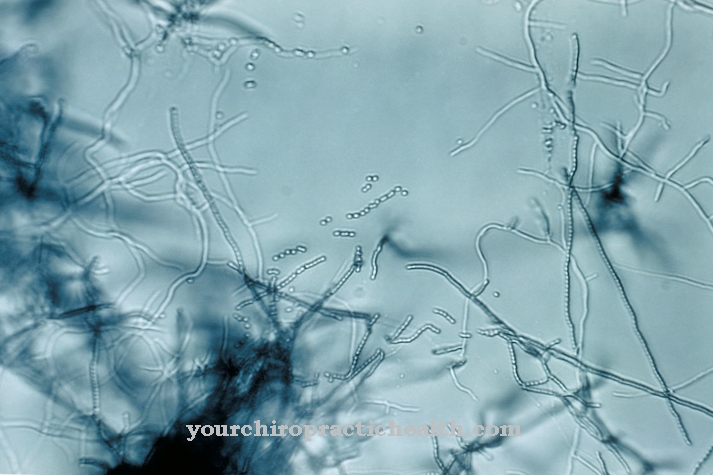
Plasmodium is a unicellular, cell wallless parasite that can attack mammals, birds and reptiles and belongs to the class of Apicomplexa (formerly: Sporozoa). Of the approximately 200 known species, 4 are relevant for humans as the causative agent of malaria. What all plasmodia species have in common is that they undergo an obligatory host change between mosquito and vertebrate, which at the same time includes a change between sexual and asexual reproduction.
What are plasmodia?

Plasmodium, which has no cell wall, is a unicellular parasite with a cell nucleus and is therefore counted among the eukaryotes (formerly also eukaryotes). The name Plasmodium is owed to the fact that in Plasmodia two cell nuclei are present after division, but the cytoplasm of the two cells is not separated from each other, but rather forms a coherent plasma space.
Of around 200 known species of Plasmodia, 4 have a special position as human malaria pathogens. All types of plasmodia undergo an obligatory host change between mosquitoes and vertebrates. The change of host also includes a change between sexual and asexual reproduction.
In humans, who act as intermediate hosts, the malaria vector is the female Anopheles mosquito. The Anopheles mosquito transmits the pathogen in the form of sporozoites that are found in its saliva. On the mosquito side, the sporozoites represent the end stage of the gametocytes with which the mosquito previously infected itself with the ingested human blood.
The four types of plasmodia that cause malaria in humans are Plasmodium falciparum (malaria tropica), Plasmodium vivax, (malaria fertiana), Plasmodium ovale (malaria tertiana) and Plasmodium malariae (malaria quartana). It is currently being discussed whether Plasmodium knowlesi, which can be found in Southeast Asia, should also be counted among the malaria pathogens that are dangerous to humans. The Plasmodium knowlesi was previously known to cause malaria in macaques.
Malaria develops flu-like symptoms with attacks of fever and, in the case of tropica malaria, is severe if left untreated. The individual plasmodia species are mostly specific and “species-faithful” with regard to the intermediate carrier (mosquito) and ultimate host (vertebrate).
Occurrence, Distribution & Properties
With the exception of Antarctica, plasmodia are native to all continents. However, the occurrence of malaria pathogens relevant to humans is now limited to tropical and subtropical areas. The plasmodia that cause malaria were also found in southern Europe and North America until the 19th century.
In tropical and subtropical regions, the annual death rate is 1.0 to 1.5 million. Estimates of the number of people suffering from malaria worldwide vary widely and are therefore between 250 and 500 million. The plasmodia are transmitted exclusively by the Anopheles mosquito. A direct transmission from person to person is practically impossible because the sexual part of the development cycle that takes place in the mosquito is missing. However, there are a few known cases in which contaminated blood transfusion needles caused direct transmission of the pathogen.
The development cycle of the individual plasmodia species is a little different, but basically follows the following development scheme: The Anopheles mosquito transfers the plasmodia in the form of sporozoites, which are initially washed into the liver with the blood and there are lodged in liver cells. In the liver cells they grow into schizonts through asexual division processes, which at a later stage differentiate into a multitude of still diploid merozoites that attack the erythrocytes (red blood cells) and multiply there through further divisions.
The time in which the sporozoites have settled in the liver cells is usually symptom-free. Some of the diploid merozoites develop into haploid micro- and macrogametocytes through meiosis, which can be ingested by a blood-sucking Anopheles mosquito via its proboscis. In the intestine of the mosquito, the gametocytes, which have differentiated into complete gametes, are united to form a diploid zygote. In the mosquito's intestinal wall, it grows into an oocyst in which, through mitotic divisions, up to 10,000 infectious, diploid sporozoites grow. After the oocyst has burst, some of the sporozoites enter the mosquito's saliva and form a new reservoir of infection.
The incubation period from infection with sporozoites to the onset of malaria is about 7 to 50 days, depending on the pathogen and without malaria prophylaxis.
Illnesses & ailments
With the exception of tropical malaria, in which the fever attacks occur at irregular intervals, other pathogens have a clear rhythm. In quartana malaria, this is four days. A day with a fever attack is followed by two fever-free days before the fever sets in again. The regular fever attacks go back to the development of the plasmodia in the erythrocytes, which almost simultaneously flood the body and cause the symptoms.
Plasmodium ovale and Plasmodium vivax, both of which are causative agents of malaria tertiana, can form hypnozoites during their liver stage, which can last unnoticed and without symptoms for several months - in individual cases even several decades - before another episode of malaria is triggered.
The best protection against malaria consists in addition to chemical prophylaxis, which should be tailored to the prevailing pathogens in the relevant region, in protection against the female Anopheles mosquito. At night, a mosquito net over the bed can provide effective protection and during the day it is advisable to wear clothes with long sleeves and long trouser legs that are impregnated with Permithrin or another mosquito-repellent substance. The uncovered parts of the body should be treated with creams or sprays, which also have a mosquito-repellent effect.