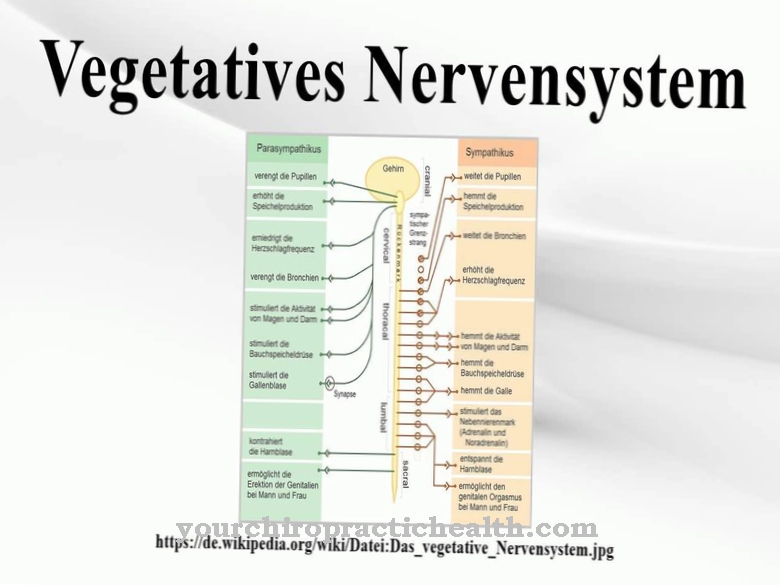
Esophageal varices are varicose veins in the esophagus, which are usually associated with advanced hepatic insufficiency. Around 50 percent of cirrhosis of the liver are associated with esophageal varices, which in turn have an increased risk of life-threatening bleeding (30 percent).
What are esophageal varices?
As Esophageal varices varicose veins or enlargements (varices) of the submucosal veins of the esophagus (esophagus) are called, which are usually due to portal hypertension as a result of progressive liver damage (including liver cirrhosis).
As a result of the impairment of the liver, the blood can no longer flow unhindered from the liver to the heart, so that it looks for alternatives via the veins of the esophagus. Bag-like enlargements develop, so-called varicose veins or varices.
In many cases, esophageal varices are discreet or with few symptoms and, in addition to the characteristic symptoms of liver cirrhosis (including ascites, signs of liver skin such as lacquer lips and tongue, expansion of the arterial vessels of the skin), manifest themselves in the form of a feeling of fullness and / or pressure in the upper abdomen and splenomegaly ( Dilation of the spleen) as an indicator of portal hypertension.
In addition, esophageal varices are associated with gastric varices and gastropathia hypertensiva (enlargement of the gastric mucosal veins) in some patients.
causes
Esophageal varices result in most cases from portal hypertension (increased portal vein pressure). Increased pressure in the portal vein is usually caused by cirrhosis of the liver (advanced liver disease), which can be caused by alcohol abuse or hepatitis.
Esophageal varices develop in about half of all those affected by cirrhosis. As a result of the damage, a portal congestion forms in the liver, as the blood is no longer able to flow freely. As a result, bypass circuits, so-called portocaval anastomoses, manifest themselves in the area between the portal vein and the inferior vena cava, which includes both hemorrhoids and esophageal varices.
In addition, cardiac insufficiency and thromboses or tumors in the area of the splenic vein, the inferior vena cava (inferior vena cava) and / or the portal vein can lead to esophageal varices.
Symptoms, ailments & signs
Varicose veins in the area of the esophagus do not draw attention to themselves in the early stages with any complaints. Occasionally a slight taste of blood is noticeable in the case of minor injuries caused by choked saliva. If esophageal varicose veins tear severely, those affected complain of sudden nausea. At the same time, they suddenly vomit large amounts of blood.
The gushy sputum is often mixed with black stomach contents (breaking coffee grounds). Such an outbreak of complaints is considered a medical emergency. A fast heartbeat tries to compensate for the unexpected loss of blood. Without the support of companions, those affected are threatened with unconsciousness.
There is a high risk of death for the patient due to a potential circulatory collapse if emergency measures are not taken. Moderate bleeding initially leads to a decrease in performance. Pallor and breathing problems occur as a result. If the blood gets into the digestive tract, it causes discomfort in the stomach area in many people.
Feelings of pressure and fullness are added. Contact with stomach acid causes the next bowel movement to turn black. The tarry stool is considered a sure warning sign of a cause of bleeding in the digestive tract. Since esophageal varices often arise as a complication of portal hypertension, people suffer from very specific signs of this underlying disease.
These include ascites (ascites), clearly protruding veins in the area of the navel and changes in the skin (banknote skin). Visibly enlarged blood vessels manifest themselves in fine or flat red discoloration on the face, upper body, hands and feet. Distinctive features include the lacquer lip or the lacquer tongue.
Diagnosis & course
Usually will be Esophageal varices diagnosed on the basis of an endoscopic examination of the esophagus (esophagogastroduodenoscopy), which enables conclusions to be drawn about the characteristics of the esophageal structures and the specific stage of the disease.
In the first stage there are ectasias (sac-like enlargements) of the affected veins, which disappear with endoscopic air insufflation. In the second stage, varices manifest themselves, about 1/3 of which protrude into the lumen (interior) of the esophagus and do not spread even with air insufflation. The third stage is characterized by an increasing narrowing of the esophageal lumen (up to 50 percent).
In addition, damage to the epithelium can become noticeable through reddish spots. In the fourth stage, the lumen of the esophagus is completely filled by the variceal cords and a large number of mucosal erosions can be detected. If left untreated, esophageal varices can perforate and lead to life-threatening bleeding, which, even with treatment, has a mortality rate of about 30 percent.
Complications
Most esophageal varices have thin vessel walls. Bleeding as a result of vascular tears is therefore a possible complication, regardless of the therapy. It mainly affects patients with larger circumventive circuits.
Minor bleeding manifests itself in the form of symptoms such as black discolored stool (tarry stool), while larger vascular tears as a result of high blood loss manifest themselves through life-threatening shock and prompt emergency medical treatment. In order to prevent life-threatening bleeding, the treating physicians estimate the willingness of varicose veins in the esophagus to bleed using endoscopic findings and the pressure gradient in the portal vein area.
From an endoscopic point of view, abnormalities such as so-called “cherry red spots” indicate an increased risk of bleeding and encourage preventive measures such as the administration of beta-blockers. With regard to the pressure gradient, the same applies to values from 12 mmHg, with greatly increased pressure values speaking in favor of combined treatment approaches with beta-blockers and nitrate. These preventive treatment steps are not suitable for treating acute bleeding. Specialists treat acute events at success rates of up to 90 percent by shutting down the affected arteries with agents such as Polydocanol or Histoacryl.
Although endoscopic treatment does not always prevent varicose vein bleeding in the esophagus, the risk of second bleeding after untreated first bleeding increases to up to 80 percent. In patients with concomitant liver cirrhosis, varicose vein bleeding in the esophagus is often associated with further complications such as hepatic coma if there is no therapy for the liver disease in addition to varicose vein treatment. The highest risk of life-threatening complications arises with esophageal varices for patients with untreated coagulation disorders.
When should you go to the doctor?
Since the esophageal varices are located as pathological veins in the lower third of the esophagus, the disease is only recognizable in the advanced stages by pain and stinging in the upper abdomen. The patient suffers from persistent nausea. In addition, there is a constant feeling of pressure and fullness in the stomach area. Slight bleeding of the varices leads to a decline in performance and permanent states of exhaustion. The patient has a permanent subliminal taste of blood in the mouth. His saliva is bloody.
The patient's face shows an unspecific pallor. It is not uncommon for patients to suffer from ascites and abnormal liver skin signs. The skin and eyes are yellow in color. The patient is prone to bleeding or bruising very quickly. Esophageal varices become clearly visible through gush-like vomiting of blood. The stool is tarry and black. The patient tends to be drowsy or even unconscious. The pulse is greatly increased. These are life-threatening warning signs. The collapse of the cycle threatens. Medical help should be given as quickly as possible and emergency measures initiated.
Treatment & Therapy
As part of causal therapy, Esophageal varices the underlying condition will always be treated. In addition, various endoscopic surgical procedures are available for the treatment of esophageal varices.
As part of sclerotherapy, a so-called sclerosant (hardening agent) is injected into the varices using an endoscope. As a result, the varice closes so that no more blood can flow into it and the tissue dies. With the help of obliteration therapy, which is usually used for bleeding varices, the affected section of the vein is obliterated (blocked) by a liquid tissue adhesive that hardens immediately after the injection into the affected vein.
Another surgical measure is the so-called ligature procedure, in which the varices to be ligated are sucked in by means of a cap attached to the endoscope and then wrapped around with a rubber ring or thread. As a result of this constriction, thromboses develop, which lead to tissue death. In addition, a balloon-like probe (e.g. Sengstaken-Blakemore probe, Linton probe) can be used in advance to stop the bleeding.
The blood flow in the affected area can also be reduced by using somatostatin or vasopressin. General measures after perforation of esophageal varices include continuous monitoring of vital functions, if necessary intubation, preventive antibiotic therapy due to the risk of sepsis, and intravenous volume administration.
As a prophylactic measure, drug (beta blockers, spironolactone, nitrates) or surgical (shunt surgery) therapy can be indicated to avoid recurrence and / or bleeding of the esophageal varices.
prevention
The manifestation of Esophageal varices can be prevented through consistent and early therapy of the underlying disease. If there is cirrhosis of the liver, strict abstinence from alcohol should be observed to avoid esophageal varices.
You can do that yourself
People who have been diagnosed with esophageal varices should pay particular attention to their food consumption in everyday life. Food that contains solid or sharp elements in any form should not be eaten.
In the case of fish, rusks or crispbread, the components of the food can lead to complications when swallowing. When eating stone fruit, you should also make sure that the pips are removed beforehand. Not only raw foods but also processed products such as cakes should be checked before ingestion.
While eating, all components of the food should be sufficiently ground in the mouth through the buying process. Do not swallow large amounts of food. Damage to the vessel walls of the esophagus could occur at any time. Since this can lead to heavy bleeding within a short time, a life-threatening condition can develop within a few minutes.
Foreign objects such as toys, objects or coins should not be put into the mouth. There is a risk that these can unintentionally get into the throat and be swallowed. If the person concerned wears braces or dentures, they should be checked daily to ensure that they are firmly in place. If there is loosening, a doctor must be consulted immediately.



.jpg)


.jpg)


.jpg)







.jpg)