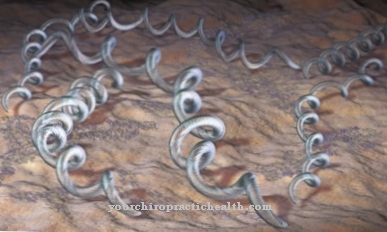
A thrombosis respectively Blood clots is a disorder or blockage of a blood vessel. Above all, thromboses develop in the legs or veins in older people after long periods of sitting or insufficient movement.
What is thrombosis?

Under one thrombosis one understands the formation of a blood clot, the so-called thrombus, within a blood vessel. This leads to a narrowing or even clogging of the vessels. Thrombosis is most common in the deep veins of the legs and pelvis.
The blood clots in the superficial veins are less common. These are varicose veins and they are usually harmless. Thrombosis is the most common vascular disease.
Arterial thrombosis is less common. It leads to a disruption of the blood flow to the affected organ or body area, so that there is a lack of oxygen here.
causes
Cause of a thrombosis can be the slowdown in blood flow. This can happen by immobilizing the legs in particular, for example after an operation, after giving birth or by sitting for a long time, for example in a car, train or plane.
Changes in blood composition can also lead to thrombosis. It is worth mentioning the warm season when the person concerned drinks too little and wears high-heeled shoes. Another possible cause of a thrombosis can be changes in the vessel wall due to inflammation, injuries or deposits.
Special factors such as the intake of estrogens, the consumption of nicotine (smoking) or infections can significantly increase the likelihood of developing a thrombosis. Frequent and regular fatty meals can also cause deposits on the vessel walls. This in turn also increases the risk of a blood clot.
However, half of all thrombotic diseases can be traced back to a disease-related and hereditary disorder of blood coagulation, also known as APC resistance.
Symptoms, ailments & signs
A thrombosis can cause a wide variety of symptoms, although the symptoms depend on the blood vessel affected. Sometimes symptoms don't appear or the clot takes a while to cause discomfort. Basically, a feeling of heaviness or a feeling of tension in the foot or leg indicates a thrombosis.
The leg, lower leg or ankle swell, the skin is warm and can also turn bluish or reddish in color. You may experience pulling pains that resemble sore muscles. There is swelling, which gets worse as the disease progresses. It is noticeable that the symptoms subside as soon as those affected put their legs up.
However, this does not improve the disease itself. If the vein is blocked and the blood can no longer flow out properly, it sometimes also flows through veins that are located on the surface. These then emerge on the shin as so-called "warning veins" and are very clearly visible.
If a thrombosis develops in a vein in the arm, the symptoms described will occur in this part of the body. If the symptoms are not treated, breathing problems or chest pain may occur and some people cough up blood, which is a sign of pulmonary embolism.
Course of disease
The course of the disease thrombosis is difficult to determine in some cases. After the clot has narrowed the blood vessel, it can continue to enlarge and eventually clog the vessel completely.
In particular, there is a risk that the thrombus will loosen and get into the lungs. Here it can become lodged and lead to a pulmonary embolism, i.e. the blockage of a blood vessel in the lungs. This can even lead to the death of the person concerned. If the thrombosis does not resolve, a new blood circulation can form here to bypass the blockage. Symptoms can include swelling of the legs, a feeling of heaviness or pain in the calf.
Complications
Thrombosis can be associated with various complications. Following the blood clot, a vein is often left behind, which is partially or even completely closed. As a result, a build-up of blood builds up within the affected limb. Due to the increased venous pressure, varicose veins, brownish discoloration on the lower leg and chronic swellings develop after a few years.
It is not uncommon for this to cause an ulcer in the ankle region, which is known in medicine as a leg ulcer. Doctors refer to these sequelae as post-thrombotic syndrome. Embolism is one of the most serious and feared complications of thrombosis. It is caused due to part or all of the blood clot peeling off.
The blood washes away the clot so that it penetrates veins and the right heart to the lungs, where it causes a pulmonary embolism. Pulmonary embolism particularly affects patients with deep vein thrombosis. This complication has different degrees of severity.
Another serious effect of thrombosis is sepsis (blood poisoning). With this consequence, bacteria settle in the blood clot and spread with the blood throughout the patient's body. As a countermeasure, antibiotics are usually administered.
Chronic venous insufficiency is another complication. This is a permanent weak vein. It is noticeable through the development of varicose veins, edema (water retention in the tissue) and skin inflammation.
When should you go to the doctor?
A doctor should be consulted in the event of circulatory disorders, abnormalities in the heart's activity or acute irregularities in the organism. Feelings of tension in the limbs, a feeling of heaviness or discoloration of the skin are indications of a health impairment. Since a thrombosis can develop into a life-threatening condition for those affected, a doctor's visit must be made as soon as the first discrepancies arise. Problems with breathing and chest pain are considered warning signals of the organism.
A stabbing sensation in the heart area should be examined and treated immediately by a doctor. In the event of an acute health-threatening condition, an emergency service must be alerted immediately. A sudden drop in internal forces, severe dizziness, unsteady gait and disturbances of consciousness are emergency signals from the body. Until a rescue team arrives, people present must take first aid measures to ensure the survival of the person concerned. Swelling, unsteady gait and impaired mobility are further signs of a health irregularity.
A visible formation of veins, for example on the legs or arms, should be presented to a doctor. It is already a first indication of the presence of a disease of the blood circulation. The formation of varicose veins, water retention and general irregularities in the blood flow should also be discussed with a doctor at an early stage. Action is required in the event of headaches, dysfunction or sensitivity disorders.
Treatment & Therapy
Treatment for a blood clot depends on the size, location, and age of the blood clot thrombosis. In any case, the first goal should be to prevent the thrombus from enlarging. This is achieved through the administration of heparin and other blood thinners, among other things.
It is still possible to restore blood flow and eliminate the thrombosis in this way within the first ten days. This is achieved through drug treatment. In more severe and older cases of the disease, surgery must be carried out. This can be a thrombectomy or a bypass.
During a thrombectomy, the clot is removed from the vessel. If the thrombosis is treated with a bypass operation, the clogged area of the blood vessel is only bridged and the blood flow is enabled again in this way.
Since there is a further risk of thrombosis, after a thrombosis a long-term drug treatment with blood-thinning agents takes place. The use of thrombosis stockings is also recommended and the patient should exercise regularly.
Aftercare
Once the plug is removed, the danger is over for the time being. But the risk of developing a new blood clot may still exist. The medical approach is to reduce blood clotting, with the result that platelet clumping is reduced to a minimum. For this reason, thrombosis patients are often given tablets that inhibit blood clotting.
Such drugs can usually be prescribed for months or years - patients should take them consistently. The ingestion of blood-thinning medication is associated with the slightest restriction in life. However, it should always be borne in mind that the blood clots less well as a result.
So if you get injured, you should expect wounds not only to bleed more violently, but also for longer. Blue spots could also appear more quickly. Before an operation, the medication should be discontinued in good time after consulting your doctor. Naturopathic substances can also effectively accompany aftercare, garlic and onions are known for their blood-thinning effect.
In addition, preparations made from horse chestnut and comfrey can help with feelings of tension and heaviness in the legs. The goal of thrombosis follow-up is to prevent platelets from clumping again so that no blood clots can migrate to vital organs such as the heart.
You can do that yourself
There are many ways to reduce the risk of thrombosis with the help of simple everyday measures. Sufficient exercise ensures good blood flow in the legs and thus prevents a blood clot. Endurance sports such as cycling or swimming are particularly suitable. Short, jerky movements, such as those that occur when playing tennis, are less suitable.
In addition to an active lifestyle, a balanced diet should also be observed. Overweight should be reduced to normal weight if possible. In addition, alcohol and nicotine should ideally not be consumed. It is also important to always drink enough water.
It is advisable to avoid sitting or standing for long periods. For example, short walks or leg exercises while sitting can be carried out if long periods of sitting cannot be completely avoided. For longer flights, it is advisable to wear special compression or support stockings as a preventive measure. The stockings can also be worn in extreme heat or while sleeping. Cold showers or cold foot baths are also suitable to support the blood flow in the veins. Alternating showers can also stimulate blood circulation.
The birth control pill can pose a risk of thrombosis. Therefore, if possible, alternative contraceptive methods should be considered and clarified by a doctor.

.jpg)

.jpg)
.jpg)




.jpg)

.jpg)


.jpg)