As Transfusion medicine This is a branch of medicine that deals with the production and provision of blood reserves and the maintenance of blood banks. After completing the regular medical degree and five years of further training, a medical professional is entitled to use the professional title of specialist in transfusion medicine.
What is transfusion medicine?
Transfusion medicine deals with the production and provision of blood reserves in blood banks. With its broad, interdisciplinary field of activity, modern transfusion medicine ensures a low-risk and patient-friendly supply of blood reserves in cooperation with almost all medical disciplines.
Many clinics in Germany have specialized in this branch of medicine. They are called the Institute for Transfusion Medicine and Transplant Immunology. These institutes not only provide conventional blood products, but also special cell therapeutics. In addition to a large blood bank, they have an associated immunohemaglobin laboratory, an HLA and platelet laboratory in the field of transplant immunology, and a stem cell laboratory. The transfusion specialists are also involved in post-operative patient care. Further areas are research and teaching.
Treatments & therapies
This medical specialty includes carrying out blood donations and the subsequent production of blood reserves, therapy with blood components and plasma derivatives, and the targeted removal of blood components for therapeutic purposes.
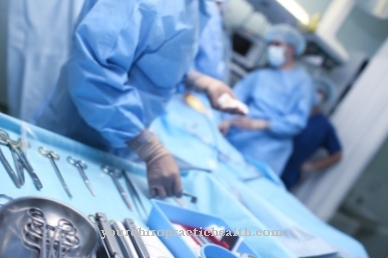
Transfusion medicine is always used when patients suffer from acute blood loss. The body is not able to compensate for this loss of blood naturally in order to regenerate sufficient blood or individual blood components. Typical areas of application are emergency medicine and operations that result in high blood loss, such as organ transplants. Diseases of the blood-forming system such as leukemia, bleeding disorders and anemia (anemia) are treated in this medical specialty. Blood reserves are also used in various cancer therapies.
Newborn or unborn babies in the womb need a blood transfusion due to anemia due to rhesus intolerance.However, transfusion medicine is also used for diseases that are not immediately associated with this specialty: cardiovascular problems, stomach and intestinal diseases as well as diseases of the nervous system, muscles, skin, blood-forming organs, connective tissue and the airways. The German Red Cross provides transfusion doctors with 10,400 blood units per day. The blood transfusion is carried out through a catheter placed before the procedure or through a hollow needle inserted into the vein.
It is also possible to donate blood (autologous blood transfusion). Here the donor and recipient are identical. Up to 900 milliliters of blood are drawn from the patient in one to three sessions four weeks before a planned procedure, in which there is a high level of blood loss with a 10 percent probability. During the surgical procedure, the patient is given his or her own blood donation. Thanks to the guidelines for the “production and administration of foreign blood products” and stringent legal requirements, transfusion medicine is very safe today. Only the risk of an intolerance reaction and slight side effects remain.
A blood or stem cell transfusion can cause immunological complications in the recipient. The patient's blood system reacts to the foreign substances in the donor blood or in the donor stem cells. Different blood groups in donors and recipients can trigger severe immune reactions such as cardiovascular disorders or anaphylactic shock. In rare cases, kidney failure can occur. If the blood groups of the donor and recipient match, minor, short-term side effects such as chills, fever, drop in blood pressure or nausea can occur.
Diagnosis & examination methods
Due to the strict legal regulations, non-immunological complications in transfusion medicine are as good as impossible. This risk area includes the transmission of pathogens such as HIV and hepatitis B or C.
Due to excessive blood transfer in large quantities, pulmonary edema or heart failure can occur. The most modern technology characterizes the laboratories in the specialist clinics and special institutes that ensure the supply of blood products. Only if the donated blood preparations are free of pathogens will they be approved for a blood donation. In order for transfusion medicine to be able to guarantee the safety of the recipient, it is not only necessary to have state-of-the-art technology, but also a careful selection of blood and stem cell donors. Strict guidelines from the German Medical Association determine who is eligible as a donor and who is not.
The donated blood is separated into its three components: red blood cells (erythrocytes), blood platelets (thrombocytes) and blood plasma. While the red blood cells ensure the supply of oxygen, the platelets play a key role in blood clotting. The plasma is the blood fluid. A whole blood donation is no longer common. The legal regulations forbid the mixing of different blood donations, because this is the only way to ensure that each individual blood supply remains traceable to the donor. The blood concentrates are stored in so-called blood banks. Clinics specializing in transfusion medicine maintain extensive in-house blood banks, while hospitals have blood banks with small capacities to meet their own needs.
The transfusion specialists have to plan the need for blood reserves precisely because red cell concentrates can only be stored for 42 days, while platelets can no longer be used after four days. Only blood plasma can be frozen for two years. This ensures that the recipient only receives the blood components that he really needs in the event of a blood transfusion. If it is certain that a patient needs a blood transfusion, the transfusion specialist will have a detailed discussion with the person concerned and obtain their consent.
Only in an emergency does a patient get a blood transfusion without their consent, for example if there is an acute risk of death due to high blood loss following an accident. The attending physician ensures that the patient receives the right transfusion preparation for him. A blood group determination and a compatibility test in the form of a crossmatch ensure that the donor and recipient match. A small amount of the patient's plasma is mixed in the laboratory with the red blood cells from the donor's intended concentrate (blood reserve).
The blood bags contain segments of tubing with small amounts of the donor blood for crossmatching. Immediately before the blood transfusion, the compatibility is checked again using the so-called bedside test, in order to rule out any remaining risks such as mix-ups.




.jpg)

.jpg)


.jpg)