Barbiturates Once considered a miracle cure and used on a large scale. Today their use is severely restricted and they are considered dangerous. There are a number of good reasons for this. The following overview of the effects of barbiturates on the body, their areas of application as well as risks and side effects show why.
What are barbiturates?

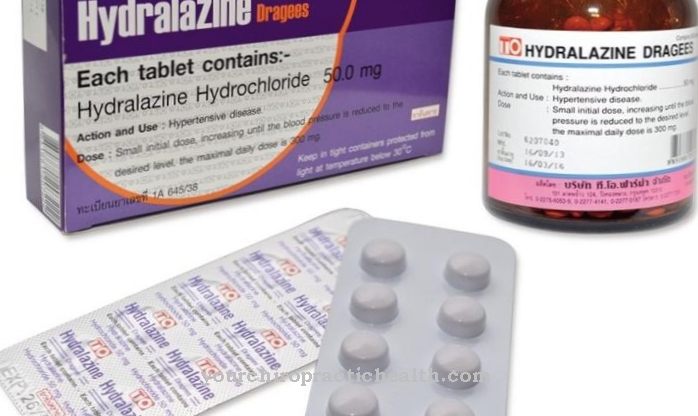
Barbiturate is the generic term for a variety of different drugs that have narcotic, hypnotic, anticonvulsant and sedative effects. Their name is derived from the barbituric acid from which they form derivatives. The chemist Johann Friedrich Wilhelm Adolf Ritter von Baeyer successfully produced barbituric acid for the first time in 1864. On this basis, Hermann Emil Fischer developed the first barbiturate with a sedative effect in 1903 and called it barbital.
Since this development, barbiturates have been among the most widely used sleeping pills and sedatives in German-speaking countries for many decades. Because they become addictive very quickly and there was a lot of poisoning through overdosing and abuse, they have not been approved as sleeping pills or sedatives in Germany since the early 1990s. Since then, they have only been used in the treatment of epilepsy and as anesthetics in operations.
There are three types of barbiturates: short-acting, which only produce an effect for a few minutes, medium-long-acting, whose effect lasts for a few hours, and long-acting, whose effect lasts for many hours. The classification is based on the duration of the respective effect.
Pharmacological effect
The pharmacological effect of barbiturates on the body and organs is extremely complex. They develop their effect via various receptors in the organism, the so-called GABA-A receptors. These are located in the nerve cells and there bind the neurotransmitter γ-aminobutyric acid. In this way, they directly influence the messenger substances that are responsible for the transmission of stimuli and excitations between the nerve cells.
After the barbiturate binds to these receptors, they practically take over their task and act as agonists to control the signal transmission between the individual nerve cells. They practically imitate γ-aminobutyric acid and take over its tasks. In this way, the barbiturates can inhibit or suppress pain signals, for example.
The dosage of the barbiturate also plays an important role in the effect. In lower doses they inhibit e.g. the AMPA receptor, which has a stimulating effect, and thus ensures sedation. In higher doses, they also inhibit sodium channels, which in turn are important for many other processes in the body. Ultimately, barbiturates lead to total anesthesia.
Medical application & use
In the past, barbiturates were mainly prescribed as sleeping pills or sedatives. However, as empirical values and studies soon revealed the extremely high potential for addiction and the dangerously high toxicity, these areas of application were finally banned. The barbiturates were replaced by far less dangerous drugs such as benzodiazepines.
Because of this fact, barbiturates are now basically only used for two areas of application: as an anesthetic and as an anti-epileptic. As an anesthetic, it is used in the form of thiopental for induction of anesthesia. The short-acting barbiturate thiopental lasts just under 10 minutes and works extremely quickly, which is why it is injected intravenously into the patient to induce anesthesia.
In the treatment of epilepsy, the long-acting phenobarbital is used, which works for about 10 to 18 hours. Due to its antispasmodic effect, it is often used both for the prevention and treatment of seizures in the context of an epileptic illness. It can also be used to combat seizures caused by contact with certain toxins such as strychnine or DDT.
In Switzerland, certain barbiturates such as pentobarbital are also used in active euthanasia permitted there. In veterinary medicine it is used as a means of euthanasia.
You can find your medication here
➔ Medicines for muscle crampsRisks & side effects
As already mentioned, the risks and side effects of taking barbiturates are extremely high. Regular consumption very quickly leads to severe addiction. Withdrawal is difficult and sometimes associated with severe symptoms such as anxiety, seizures and over-excitability. The liver also reacts to regular intake and breaks down the barbiturate faster and faster over time, which is why the effect becomes weaker and shorter. In the course of this, other drugs are broken down more quickly and therefore no longer work properly. Too high a dosage can also lead to severe poisoning, the symptoms of which range from impaired consciousness and dizziness to nausea and vomiting to amnesia and coma. The worst toxic effect, however, is central respiratory paralysis and cardiac arrest, which, without immediate treatment, lead to an insufficient supply of the brain with oxygen and ultimately to death. Other sedating agents such as alcohol or opiates also increase the effect of the barbiturates. Because of these strong side effects, barbiturates are now subject to the Narcotics Prescription Ordinance (BtMVV).
Barbiturates work very quickly and effectively, but unfortunately they are associated with many, sometimes even life-threatening, risks and side effects that by far exceed their positive properties. Therefore, with a few exceptions, their use is now prohibited for understandable reasons. Self-medication is therefore strongly discouraged.