A dyshidrotic eczema is a skin disease characterized by blisters on the palms of the hands, the sides of the fingers, and the soles of the feet. Its exact causes are not yet fully understood, but there is a connection with drugs and other substances, fungi, bacteria, viruses and psychological factors. Therapy predominantly focuses on individual triggers and treating the skin changes.
What is dyshidrotic eczema?

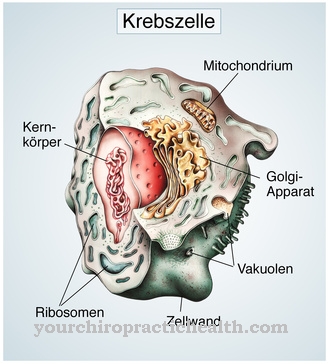
© oscity - stock.adobe.com
Dyshidrotic eczema is a dermatological disease that causes small blisters to develop on the palms of the hands and soles of the feet. The clinical picture represents a specific form of eczema and as such belongs to the inflammatory skin diseases. Other names for dyshidrotic eczema are Dyshidrosis or Dyshidrosis, Pompholyx or dyshidrotic eczema.
Two variants can occur with this skin disease: With dyshidrosis lamellosa sicca it shows only as a weak change of the skin. In the short course of the acute phase, the vesicles dry out by themselves and leave behind their empty shell. This also dries out and gradually dissolves from the skin in scales as new skin cells grow back. In the case of the Cheiropompholyx or Podopompholyx variant, on the other hand, the vesicles are larger, partially merge and form a larger target for infections.
causes
Researchers originally believed that a malfunction of the sweat glands was the cause of dyshidrotic eczema. The name of the disease, which basically means “bad sweat”, goes back to this fallacy. It is now known, however, that this cause is incorrect; the exact factors that cause dyshidrotic eczema are not known.
The specialist literature discusses, among other things, the relationship between dyshidrotic eczema and various drugs, other chemical substances, bacteria and fungi. Psychological factors such as stress may also play a role in the occurrence of the disease. People with a contact allergy or atopy are more likely to develop dyshidrotic eczema.
In these cases, however, the skin change must not be entirely due to one of the two skin diseases, but must exist independently of it; otherwise, despite the similar appearance, it is not dyshidrotic eczema but a contact allergy or atopy. In this context, good differential diagnostics are important.
You can find your medication here
➔ Medicines against redness and eczemaSymptoms, ailments and signs
Itching often occurs on the affected areas of the skin and is typical of all types of eczema. In dyshidrotic eczema, small blisters form under the skin on the palms of the hands, the sides of the fingers and the soles of the feet. They are filled with fluid and can stretch the tissue above. The liquid inside is yellowish or colorless.
Reddening of the skin around the blisters is also one of the typical symptoms. For long-term eczema, the skin may thicken, begin to flake, or form a leathery surface. As a result, the skin loses its elasticity, making it more prone to bleeding cracks.
These so-called rhagades usually heal without scarring. Since the skin on the hands and soles of the feet, where the blisters normally develop in dyshidrotic eczema, is constantly in motion, the healing process can take a long time. The affected areas often tear again and again, especially without the use of ointments.
Diagnosis & course
The external appearance of the skin changes is usually sufficient for the diagnosis to be made. Since allergic reactions can cause similar symptoms, the diagnosis often includes an allergy test for contact allergies. In the patch test or patch test, the most common allergens that could be triggers are applied to the skin and covered with a large patch.
After 48 and 72 hours, sometimes also after 96 hours, the diagnostician checks whether there is any change in the treated skin. A positive reaction means that there is an allergy. In addition to contact allergy, atopy is also considered in the differential diagnosis. It can cause atopic eczema, which is similar to dyshidrotic eczema.
In the course of the skin disease, the vesicles of dyshidrotic eczema can flow together; medicine calls this process confluence. In some cases, dyshidrotic eczema is associated with an infection that is primarily caused by viruses and fungi. The pathogens can penetrate the tissue, in particular via burst or scratched vesicles. The large blisters in the Cheiropompholyx and Podopompholyx variants are particularly prone to this complication.
Complications
The disease mainly causes discomfort on the skin. Blisters form, which in most cases are also associated with itching. Often there is also increased sweating on the skin, which seems uncomfortable for many patients.
The blisters can also burst, causing a liquid to leak out. The itching causes many sufferers to scratch, which usually only intensifies the itching. The quality of life decreases significantly as a result of the disease. Certain activities are also no longer possible for the patient, as contact with the skin would otherwise lead to pain.
Treatment of the symptom is carried out with the help of creams, ointments and medicines and in most cases leads to success relatively quickly. There are no further complications. In the case of allergies, the patient must forego the respective triggering substance so that the symptoms do not occur. As a rule, the disease can be narrowed down relatively well if a healthy diet is followed. Life expectancy is not restricted.
When should you go to the doctor?
If any unusual itching is suddenly noticed, a general practitioner should be consulted. At the latest when the characteristic blisters form under the skin, the dyshidrotic eczema must be clarified and treated. As the disease progresses, reddening and cracks in the skin may appear, which should be observed first - the doctor must be informed in the event of bleeding or infection. People who suffer from atopy or a contact allergy are particularly likely to develop dyshidrotic eczema.
Likewise people who regularly take certain drugs or chemical substances. Psychological factors such as stress can also promote the skin disease. Anyone who belongs to these risk groups should consult a doctor if the symptoms mentioned. The doctor will either be able to clarify the disease beyond doubt or refer the patient to an allergist.
In any case, several visits to the doctor are required before the dyshidrotic eczema can be diagnosed with certainty. If the eczema becomes infected, in the best case scenario, a dermatologist is consulted directly. In the event of major complications, the emergency medical service should be contacted.
Doctors & therapists in your area
Treatment & Therapy
Various ointments, creams and lotions are used for external treatment. They often contain glucocorticoids, a type of corticosteroid. The aim of the active ingredient is to inhibit the inflammatory reaction. Corresponding ointments are particularly suitable for shorter applications, as they can cause increased side effects with regular use over weeks and months.
Medicines containing 9-cis retinoic acid (alitretinoin) are a treatment option, even if glucocorticoid therapy is unsuccessful. Tannins may accelerate the drying out of the blisters on the hands and feet, and zinc ointment can also have anti-inflammatory effects. Adequate hygienic measures can help reduce the risk of complications caused by infections.
However, gloves and too frequent hand washing and disinfection - also at work - are considered problematic. Which treatment option is sensible varies from person to person. A decisive factor is the specific cause of the dyshidrotic eczema: If a causal treatment is possible, further therapeutic measures can take effect.
Outlook & forecast
The prognosis for dyshidrotic eczema is good. Although the exact cause is not yet complete, the individual triggers can be treated and treated with current medical options. In addition, there are various risk factors that promote the occurrence. If the patient manages to avoid this, he favors the further course. As soon as the active ingredients of prescribed medicines develop their anti-inflammatory effects, symptoms are relieved.
The treatment plan is developed according to the patient's individual complaints. In many cases the patient can actively influence the improvement of his symptoms through his hygiene and cleanliness behavior. The prospect of relief from the lesions worsens once the itchy rash is given in.
In these cases, the patient threatens the penetration of further pathogens into the organism. In severe cases, this can lead to blood poisoning. There is a life-threatening situation for the person concerned.
If there are psychosomatic reasons for the onset of the disease, the healing process can take several years. With seasonal causes, the patient experiences phases of complete freedom from symptoms. Eczema can return for life and at any time. The person concerned should avoid stress and coordinate the use of skin care products with the doctor so that no ingredients are used that would aggravate the symptoms.
You can find your medication here
➔ Medicines against redness and eczemaprevention
The prevention of dyshidrotic eczema can focus on typical triggers: Patients can avoid substances that act as triggers for them individually. Patients can also counteract psychological factors such as stress, for example with relaxation techniques and stress management training.
Aftercare
With this disease, the person affected is primarily dependent on direct treatment from a doctor. The measures or options for follow-up care are usually very limited, so that early detection and continued treatment by a doctor are in the foreground. Self-healing cannot occur, so that the person affected is always dependent on a visit to a doctor.
With this disease, the person affected should avoid infections if possible. A high standard of hygiene must be ensured, and the person affected should wash frequently. In the event of an infection, the main thing to do is to consult a doctor to treat it. Most patients are also dependent on taking medication.
The person affected should always ensure that they are taken regularly and that the dosage is correct in order to relieve the symptoms permanently and correctly. Should the medication cause severe side effects, a doctor should also be consulted before the medication is discontinued. In most cases, this disease does not reduce the life expectancy of those affected.
You can do that yourself
In dyshidrotic eczema, small blisters form on the hands and feet. The cause of this disorder has previously been attributed to a malfunction of the sweat glands, but this is not the case. The trigger for the disease is unclear, but a connection with medication, contact allergies, excessive hygiene and psychological stress is suspected. Affected people should always consult a doctor so that an allergy can be excluded and the symptoms treated professionally.
Due to the mostly unknown causes, an important contribution to self-help is to keep a diary to check whether there is a statistical connection between certain activities and acute attacks of the disease. If new blisters develop a few days after stressful situations, for example an exam or an argument with the supervisor or family member, psychological factors should be considered as triggers. Those affected can then learn relaxation techniques to better cope with negative stress.
A food diary can also be used to determine whether a food allergy could possibly be a contributory factor. In these cases, the person affected may have to change their eating habits.
The bubbles should never be scratched open. Antihistamines in drop form, which are available over-the-counter in pharmacies, help against severe itching. The healing process can also be accelerated in many cases by applying a thick layer of zinc ointment to the affected areas in the evening. Cotton gloves or cotton socks should be worn so that the ointment can work overnight.

.jpg)