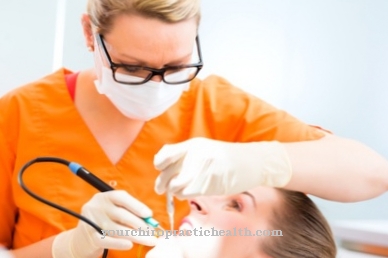
Elizabethkingia is a gram-negative bacterium from the flavobacteria family. Like the large number of other flavobacteria species, the bacterium is almost omnipresent in soil and water. Occasionally, the species Elizabethkingia meningoseptica occurs as a cause of meningitis in premature infants, babies and young children. Since November 2015, a mysterious wave of infections has been observed in Wisconsin, USA, which is caused by the bacterium Elizabethkingia anophelis and which until mid-March 2016 had affected over 50 people.
What is Elizabethkingia?
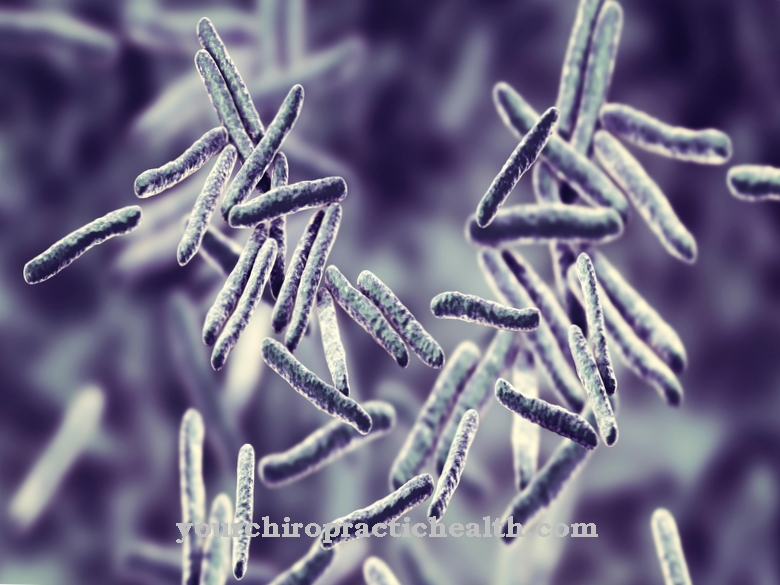
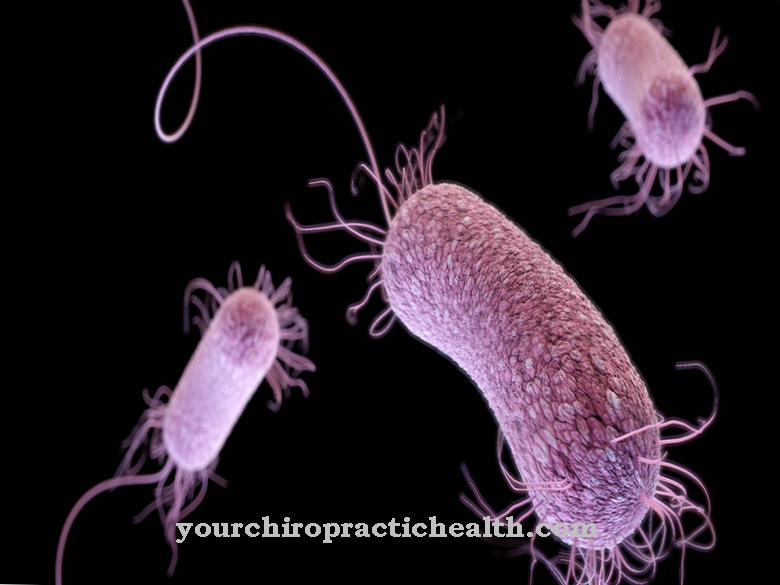
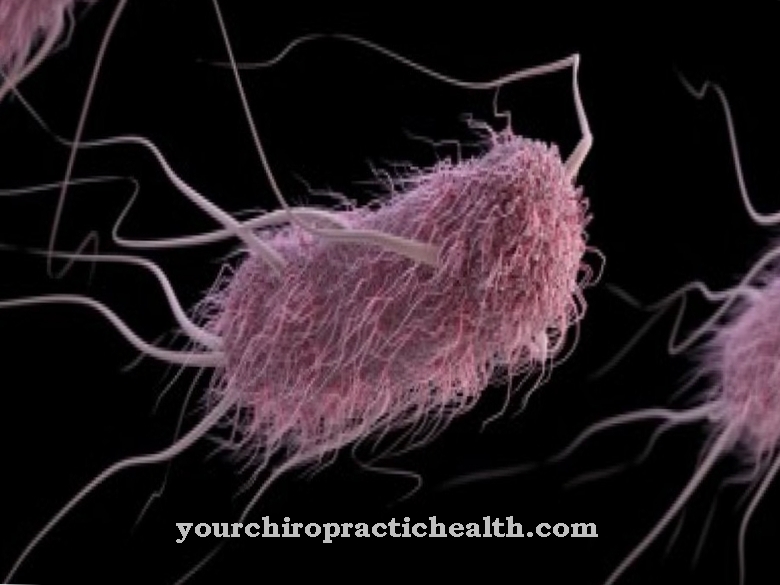
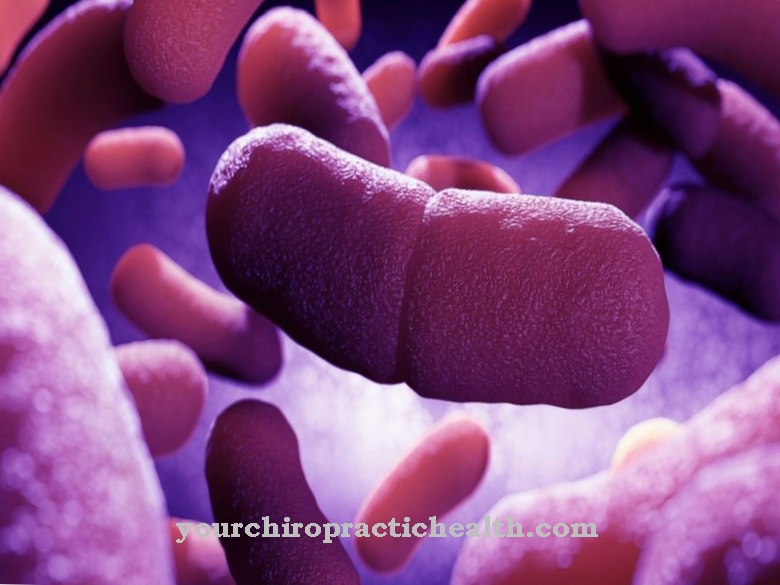
Elizabethkingia is a gram-negative, rod-shaped, slightly curved, immobile bacterium from the flavobacteria family (Flavobacteriaceae). The bacterium, which was discovered in 1960 by the American bacteriologist Elizabeth O. King, was given the name temporarily Flavobacterium meningosepticumwhich suggests the bacteria may be associated with meningitis and sepsis.
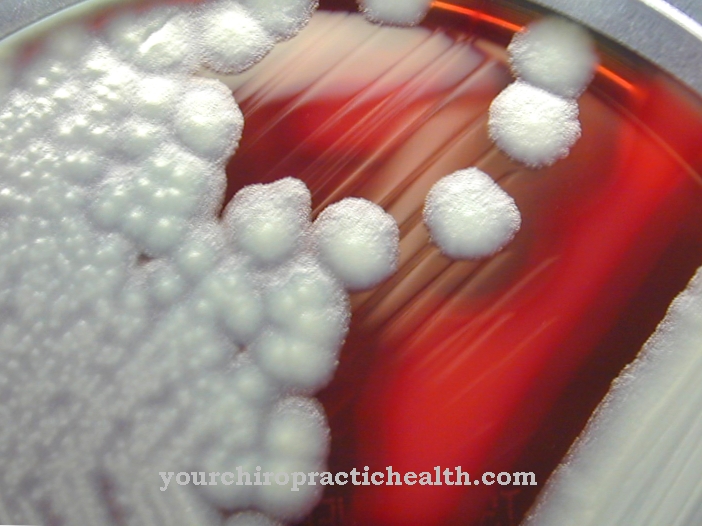
It was not discovered until 2005 that the bacterium, together with another species, created its own type of flavobacteria and was then named Elizabethkingia in honor of its discoverer. At least two subspecies, Elizabethkingia meningoseptica and Elizabethkingia anophelis, are known. The assignment of the bacterium to the flavobacteria means that, like the other members of the family, they have a yellowish color. The yellowish color that is caused by the flexirubin pigment can be seen well in larger colonies of flavobacteria.
Some strains of flavobacteria are aerobic and others are anaerobic. Elizabethkingia is an obligatory aerobic bacterium which is dependent on oxygen supply for its energy balance and which is almost omnipresent in nature, in the soil and in water.
Occurrence, Distribution & Properties
As explained above, the microbe Elizabethkingia can be found almost ubiquitously in the environment, especially in arable soils and in fresh or salt water lakes and in almost all stagnant bodies of water. It does not differ fundamentally in its occurrence from other members of the large family of flavobacteria. Only in rare cases does the bacterium have a facultative pathological effect.
Elizabethkingia only reproduces by sprouting, as the bacterium cannot develop spores.In bacterial cultures that have been established, the reactions to appropriate detection tests for the enzymes catalase, indole and oxidase are positive, while the reaction to the enzyme urease is negative. This means that colonies of Elizabethkingia have the enzymes tested positive by their own synthesis, while the enzyme urease is not produced as a result of the negative test.
The subspecies Elizabethkingia meningoseptica occasionally also occurs as a nosocomial germ, i.e. as a hospital-specific germ that is resistant to some of the known antibiotics. The bacterium has the ability to synthesize enzymes such as beta-lactamases and extended beta-lactamases (ESBL), which they can use to deactivate certain antibiotics.
There is an increased risk of infection in premature infants, babies and small children whose immune systems have been weakened or artificially suppressed. Dialysis patients also have an increased risk of infection. Typical clinical pictures that can be caused by the germ are meningitis (meningitis), pneumonia (pneumonia) and inflammation of the inner lining of the heart (endocarditis). Elizabethkingia meningoseptica can also cause sepsis, a systemically widespread inflammation.
Clinical equipment, tap water, and contaminated venous catheters can be considered major routes of infection. There is no direct risk of infection from person to person.
Meaning & function
The Elizabethkingia flavobacterium is just as ubiquitous as most other members of the flavobacteria family. That they appear as pathogens is relatively rare. However, no studies have yet become known that show that the bacterium is associated with other bacteria that colonize the skin or mucous membranes or are part of the healthy intestinal flora. It is very likely that the obligatory aerobic microbes have no immediate and special significance for the human body and health.
Illnesses & ailments
Despite their almost ubiquity, flavobacteria and Elizabethkingia are usually not pathogenic with the exception of the bacterium Elizabethkingia meningoseptica, which, as described above, can sometimes cause problems as a nosocomial germ.
Since November 2015, a special germ called Elizabethkingia anophelis has appeared in Wisconsin, USA. In the period from November 1, 2015 to March 16, 2016, 54 people over the age of 65 in Wisconsin were demonstrably infected with the germ. All sick people suffered from another disease at the same time, so that here, too, it is very likely that a weakened or heavily stressed immune system facilitated an infection.
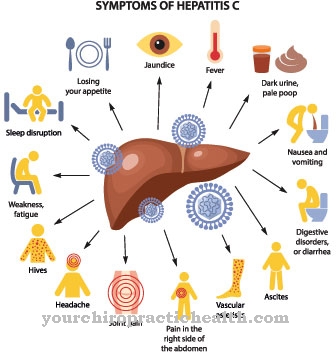
Common symptoms of Elizabethkingia anophelis infection are typically fever, shortness of breath, and chills. Most patients develop pneumonia.
Of the 54 infected people, 15 patients have already died, although the cause of death can also be due to an existing further disease. The authorities in the US are still looking for the causes of the infection. Obviously, Elizabethkingia anophelis responds to certain antibiotics, so that efficient treatment options are available.
Some evidence suggests that the pathogen is transmitted by mosquitoes. A similarly explosive case of a series of infections with Elizabethkingia was delivered a few years ago by a London hospital, in whose intensive care unit 30 out of a total of 900 patients were infected with the germ. After a long search, certain taps were identified as sources of infection. In contrast to the series of infections in London, which took place exclusively in the intensive care unit of a hospital, people outside of hospitals in Wisconsin were also infected, which makes it difficult to find the source or sources of infection.











.jpg)