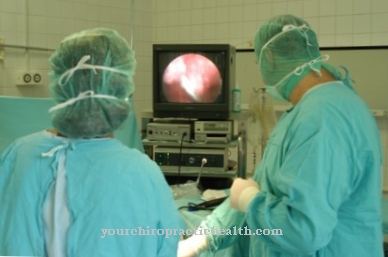
In the Epispadias there is a gap in the urethra. Boys are much more likely to be affected by the phenomenon than girls. Epispadias can be corrected surgically, and the procedure should be performed before puberty.
What is epispadias?

© kocakayaali - stock.adobe.com
Epispadias is a malformation of the urethra. This malformation mainly affects the male sex. The term Epispadie comes from the Greek and translates as: "Column above". Aptly, the disease is a congenital split in the urethra that lies on the back of the penis. This is to be distinguished from hypospadias.
This is also a split urethra, which, unlike epispadias, lies on the underside of the penis. The prevalence of epispadias in boys is around one in 300,000. In girls, the malformation is significantly less common. Medicine assumes one out of 400,000 people affected. There is a connection between the more common bladder exstrophy and epispadias. Bladder exstrophy is often associated with epispadias.
causes
Epispadias is a developmental disorder of the fetus during pregnancy. This disorder occurs in the third week of pregnancy and affects the cloacal membrane. The genital cusps of the fetus do not completely fuse in the area of the cloacal membrane. There is a gap due to the painting position. Medicine assumes a hereditary factor, as the malformation occurs more frequently in some families.
General growth delays in pregnancy are now considered a risk factor. In addition, taking medication during pregnancy can promote the malformation. In the case of epispadias as part of a bladder exstrophy, the malformation of the cloacal membrane is even more pronounced than in individual epispadias.
You can find your medication here
➔ Medicines for bladder and urinary tract healthSymptoms, ailments & signs
In boys, epispadias is either a gap on the back of the penis or an enlargement of the external urethral opening. In addition to epispadias, the limb can be shortened. Typically there is also too much foreskin. Usually the bladder is split too, causing urinary incontinence. Usually there is no erectile dysfunction. In girls, epispadias usually appear as a complete gap in the clitoris and bladder. The mound of venus is flat.
The urethra is wide and shortened. For gradual differentiation of epispadias, medicine uses the additions gladis, pubis, coronaria, glandis and penis. With gladis a urethral opening on the glans penis is meant. The word "coronaria" refers to the "Corona glandis". Penis means a localization on the penis shaft and “pubis” stands for a position above the penis root. On the other hand, an epispadia “totalis” is associated with an open bladder.
diagnosis
The doctor makes the diagnosis of epispadias via eye diagnosis. To determine the extent, he also performs ultrasound examinations or creates an elimination program. Due to incontinence, those affected by epispadias have to struggle with psychological problems from a certain age.
In order to avoid psychological complications, the malformation should be corrected as soon as possible. Correction before puberty is advisable so that the sex organs can develop normally during this time.
When should you go to the doctor?
Epispadias should be corrected as soon as possible. Most of the time, the malformation is diagnosed by a doctor right after the birth, who will then initiate the treatment routinely. If the symptoms are less pronounced, the epispadias is often only noticed after days or weeks. Parents who notice abnormalities in the genital area or even pronounced urinary incontinence in their child should speak to their pediatrician or family doctor.If treatment is not received, those affected often develop psychological problems.
Then therapeutic advice is definitely indicated. At the same time, of course, the malformation must also be corrected. If the diagnosis is made after puberty, a specialist in genital plastic surgery may need to be called in. After the procedure, regular check-ups should be carried out in order to identify any complications early on. Women who took medication during pregnancy are more likely to have a child with epispadias. If medication cannot be avoided, the growth of the fetus should be monitored particularly closely.
Doctors & therapists in your area
Treatment & Therapy
Like hypospadias, epispadias can only be treated surgically. Surgical treatment aims to produce a functional and visually largely normal penis or, in girls, a largely normal clitoris. In boys, the surgeon usually performs urethral surgery for this purpose. This procedure is possible from the first year of life. An age between one and four years is recommended for the procedure.
In girls, on the other hand, the surgeon reconstructs the mons pubis and unites the two halves of the clitoris that were separated by the cleft. The reconstructive operation should therefore take place at the youngest possible age so that social urinary continence can be achieved before puberty. If those affected cannot be relieved of the malformation by puberty, psychological problems often arise. In boys around the age of three, attempts are therefore made to reconstruct the non-existent sphincter muscle.
If this attempt is unsuccessful, the urine must be diverted from the urinary bladder in another way. How many interventions are required for correction depends mainly on the wound healing after the first operation. In the case of fistulas, scarred constrictions of the urethra or bulges in the urethral mucosa, for example, follow-up operations are due. Those affected therefore have to appear for regular check-ups after an operation, during which on the one hand the wound healing and on the other hand the success of the operation are checked.
These check-ups may take several years. Usually, after a correction, the penis or clitoris will develop normally even during puberty. Only in rare cases is a further intervention necessary to enable conventional development.
Outlook & forecast
An isolated epispadias is not associated with an increased risk of urinary tract infections. Secondary diseases can occur if the deformity is particularly severe or is located in a difficult-to-reach location. Epispadias in the area of the penis root can lead to problems with ejaculation.
The ejaculation problems cannot be completely eliminated even with comprehensive treatment. In female patients, epispadias can be associated with stress incontinence. There can also be problems with sexual intercourse. Other organs are usually not affected in either sex.
The prospect of recovery therefore depends on the gender of the patient and the severity of the epispadias. Apart from the defect, the patients are considered healthy, although psychological problems can occur in addition to the subsequent symptoms mentioned. If the epispadias is diagnosed and treated immediately after birth, surgical treatment usually improves any accompanying symptoms. If there are no further symptoms in the first few months after the operation, a cure can be assumed.
The prognosis is worse if the epispadias is not diagnosed because it occurs, for example, in the urethra. Then incontinence, infections and the resulting complications can occur in early childhood. In this case, too, an operation brings an improvement in the symptoms.
You can find your medication here
➔ Medicines for bladder and urinary tract healthprevention
So far it is largely unclear what causes epispadias. Since medication intake is likely to play a role during pregnancy, not taking medication is a preventive measure. If this waiver is not possible for health reasons, epispadias can hardly be prevented according to the current state of medicine.
Aftercare
In the case of epispadias, the patient usually has only very limited options for follow-up care. The person concerned is primarily dependent on a medical examination and treatment by a doctor in order to permanently alleviate the symptoms of epispadias. If the disease is not treated in time, it can lead to serious complications and complaints that can make the patient's life significantly more difficult.
First and foremost, an early diagnosis should therefore be made. The treatment of epispadias is usually supported by a surgical procedure. There are no particular complications, and the person affected should rest after the procedure and take care of their body. Only through strict bed rest can a full recovery occur.
As a rule, strenuous and stressful activities should also not be performed. In many cases, even after successful treatment, those affected are dependent on regular examinations by a doctor, above all to guarantee proper wound healing.
Care and support from one's own family or friends also has a positive effect on the course of the epispadias and can prevent psychological upsets. The life expectancy of the person affected is usually not restricted by this disease.
You can do that yourself
Patients with epispadias have no means of curing the disease. The body's self-healing powers or alternative methods are insufficient to alleviate the malformation.
In spite of the disease, care should be taken to ensure adequate fluid intake. This should not be neglected or restricted, as otherwise there is a risk of an undersupply of the organism.
In order to avoid sexual disorders after a correction of the urethra, this topic should be discussed intensively. The patient can inform himself comprehensively about the disease and also take advantage of advice. It is advisable to gain your own intimate experiences before sexual contact with another person takes place. If this is not enough, professional help should be sought.
Sex therapists help the patient to optimize their attitudes or behavior. An exchange with other patients can also be found helpful. Experiences can be discussed together and inhibitions can be broken down.
In an atmosphere of trust, many patients manage to talk about their everyday challenges. This allows mutual tips and hints to be exchanged. In addition, relaxation techniques are recommended to reduce stress. These strengthen mental strength and lead to the build-up of emotional resources.













.jpg)

.jpg)