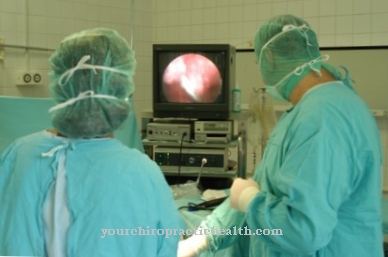
Hemodynamics describes the flow behavior of the blood. It deals with the physical fundamentals of the blood circulation and the factors that affect the blood flow, such as blood pressure, blood volume, blood viscosity, flow resistance, vascular architecture and elasticity.
What is Hemodynamics?

The fluid mechanics of the blood is influenced by various parameters. This regulates the blood flow to organs and body regions and adjusts them to their needs. The most important parameters for regulation are: blood pressure, blood volume, cardiac output, blood viscosity as well as vascular architecture and elasticity, which in medicine is referred to as the lumen of a blood vessel. It is controlled by the autonomic nervous system and the endocrine system with the help of hormones.
The hemodynamics not only determine the flow of blood, but also have an influence on the function of the endothelium and the smooth vascular muscles. The arterial blood vessels have a certain ductility due to their wall structure, that is, they can increase or decrease their radius.
If high blood pressure is registered, vasodilation, i.e. vasodilation, can be initiated. When vasodilatory substances such as nitric oxide are released, the radius of the blood vessel increases, which in turn reduces blood pressure and flow rate.This works the other way around in the same way with low blood pressure and vasoconstriction, the constriction of the vessels.
Function & task
The complex interaction of this system is of great importance for humans, so that a sufficient blood supply to the organs is guaranteed when one of the parameters is changed.
Under physiological conditions there is a laminar flow almost everywhere in the vascular system. This means that the liquid particles in the middle of the vessel have a significantly higher speed than the liquid particles at the edge. As a result, the cellular components, especially the erythrocytes, move in the center of the blood vessel, while the plasma flows closer to the wall. The erythrocytes migrate faster through the vascular system than the blood plasma.
The flow resistance in laminar flow is most effectively influenced by changing the vessel radius. This is described by the Hage-Poiseuille law. According to this, the current strength is proportional to the 4th power of the inner radius, which means that when the diameter is doubled, the current strength increases by a factor of 16. Tubular flow can also occur under certain conditions. Turbulences cause an increase in the flow resistance, which means more stress for the heart.
In addition, the viscosity of the blood also has an influence on the flow resistance. With increasing viscosity, the resistance also increases. Since the composition of the blood varies, the viscosity is not a constant variable. It depends on the viscosity of the plasma, the hematocrit value and the flow conditions. The viscosity of the plasma is in turn determined by the plasma protein concentration. If these parameters are taken into account, one speaks of the apparent viscosity.
In comparison, there is the relative viscosity, here the blood viscosity is given as a multiple of the plasma viscosity. The hematocrit influences the blood viscosity insofar as an increase in the cellular components causes the viscosity to rise.
Since the erythrocytes are deformable, they can adapt to different flow conditions. When there is a strong flow with high shear stress, the erythrocytes assume a form with little resistance and the apparent viscosity drops drastically. Conversely, it is possible that the erythrocytes collect to form aggregates like money rolls when the flow is slow. In extreme cases, this can lead to a blood stasis, or stasis.
The apparent viscosity is also influenced by the vessel diameter. The erythrocytes are forced into the axial flow in small blood vessels. A thin plasma layer remains at the edge, which enables faster movement. The apparent viscosity decreases with smaller vessel diameter and leads to a minimal blood viscosity in the capillaries. This is the so-called Fåhraeus-Lindqvist effect.
Illnesses & ailments
Pathological changes in the blood vessels can disrupt hemodynamics. This is the case, for example, with arteriosclerosis. The disease develops slowly and often goes unnoticed for years as the patient does not notice any symptoms. Deposits of blood lipids, thrombi and connective tissue form in the blood vessels. So-called plaques develop, which narrow the vascular lumen. This restricts the blood circulation and leads to secondary diseases.
Another risk is that cracks will form in the vessel wall as a result of the higher stress, which leads to hemorrhage and thrombus formation. In addition to the limitation of the lumen by the deposits, the actually stretchable blood vessels become rigid and hardening occurs.
Arteriosclerosis leads to various secondary diseases due to the circulatory disorder, depending on the location. The effects in the cerebral vessels are particularly threatening, as the result is a disruption of brain function. If arteries are completely blocked, a stroke occurs. Coronary artery disease can develop in the coronary arteries. Their spectrum ranges from an asymptomatic form to angina pectoris and heart attack.
Especially smokers often develop peripheral arterial occlusive disease (PAOD). Leg or pelvic arteries are affected and the shorter the walking distance the affected person will be able to cover as the severity increases. That is why PAVK is also known colloquially as "intermittent claudication".
The risk of arteriosclerosis does not only come from the narrowing of the lumen. The splitting off of arteriosclerotic plaques or thrombi can also lead to life-threatening complications, such as a pulmonary embolism or stroke. Smoking, high blood pressure, diabetes mellitus and high blood lipid levels are considered risk factors for arteriosclerosis.

















.jpg)

.jpg)