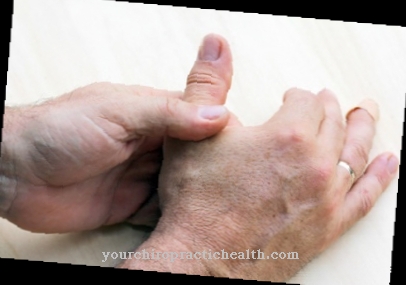
If the kneecap has slipped out of its V-shaped sliding bearing, this is called Patellar luxation designated. With a frequency of around 6 in 100,000, patellar dislocations are among the most common injuries to the knee joint.
What is a patellar luxation?

© elina33 - stock.adobe.com
As Patellar luxation is a dislocation (dislocation) of the kneecap (patella) in which the patella has usually jumped laterally (to the outside) out of the bony guide groove or its sliding bearing on the thighbone (femur).
Additional ligaments, bones and cartilaginous structures in the affected knee are often injured. In most cases, a patellar dislocation manifests itself in the form of pain in the anterior region of the knee, an extension deficit, joint effusion, and pressure pain on the lateral condyle (articular process) and medial retinaculum (tether) of the femur.
In addition, a distinction is made between initial dislocations as a result of external trauma (impact, blow, fall) and post-traumatic, chronically recurrent and habitual patellar dislocations without an existing trauma. In rare cases, congenital (congenital) dislocations of the kneecap can be identified.
causes
Depending on the specific triggering cause, different forms of Patellar luxation distinguished. In the case of a habitual dislocation, a system-related malformation of the plain bearing, the retaining straps, muscles and / or knee joint capsules results in instability of the kneecap.
In addition, acquired dispositions such as an enlargement of the Q-angle, a flat articular process of the femur, a patella alta (elevated kneecap), genu recurvatum (high knee), atrophies of the stabilizing muscles, femoral anterior torsions are associated with an increased risk of patellar luxation.
Reduced blood flow and bone necrosis in the area of the knee joint, in particular on the slide bearing or on the kneecap, can impair the adjacent cartilaginous structures and thus lead to instability of the kneecap and correspondingly to dislocations. In addition, external trauma or twisting accidents during sporting activities can cause the kneecap to slip out of its guide groove (traumatic patellar dislocation).
Symptoms, ailments & signs
The most noticeable and characteristic symptom of a popped kneecap is sudden, severe pain when moving. This is particularly noticeable below the knee and on the inside of the knee. Due to the severe pain, those affected can no longer move their lower leg and cannot put weight on the leg.
They usually automatically adopt a gentle posture. As a result, a striking deformation of the knee can also be seen directly from the outside. Paralysis rarely occurs. In a few cases the kneecap is so severely dislocated that it can only be returned to its original position by force.
The affected person can feel the kneecap slipping away. In addition, there may be visible swelling of the knee if joint effusions also occur. Sometimes bruises can be seen on the skin if the ligament is injured and bleeding occurs. In such cases, clearly audible pressure pain also occurs.
Various bone fractures and cartilage injuries can occur together with a patellar dislocation, which cause a number of other symptoms. In this way, pressure or movement pain can also be perceived in other areas of the affected leg. If the kneecap slides back on its own, the knee usually remains swollen. The pain can initially be perceived as weakened.
Diagnosis & course
As a rule, a Patellar luxation, especially an acute traumatic dislocation, can be diagnosed based on the characteristic symptoms.
The diagnosis is confirmed by an X-ray image, which also allows statements to be made about congenital causes and accompanying bone or cartilage injuries. Above all, a so-called patella défilée image, a target image with increasing flexion, is used to assess patellar laterization and possible cartilage damage (chondropathy). Arthroscopy can rule out unsafe cases and at the same time surgically remove minor cartilage and bone damage.
Magnetic resonance imaging (MRI) is used to more precisely estimate the cartilage damage and possible impairment of other soft tissues of the knee. If there is a joint effusion, a puncture should be carried out to rule out accompanying injuries. In the long term, after a patellar dislocation, retropatellar arthrosis (joint wear) is to be expected in many cases despite a good prognosis, as the previous stability of the kneecap cannot be restored even with consistent therapy.
Complications
Usually, the patellar dislocation results in a dislocation of the kneecap. This complaint is very painful, causing severe pain, especially in the knees. This pain can spread to other parts of the body. Furthermore, the knee pain at night can lead to sleep problems and thus to irritability of the person concerned.
The patients also suffer from an effusion on the knee and severe swelling due to the patellar luxation. Walking difficulties and restricted mobility are also expressed in relation to the clinical picture. Many everyday activities are only possible with greater difficulty, so that in many cases those affected depend on the help of other people in their lives. The pain of the patellar luxation can be limited with the help of medication.
However, long-term use of pain relievers can damage the stomach. Likewise, the person concerned is usually dependent on therapy in order to achieve complete healing. In severe cases, the patellar dislocation can also damage the cartilage. Surgical intervention is usually necessary to remove the destroyed cartilage.
When should you go to the doctor?
If visual changes in the knee joint are noticed, a doctor should be consulted. If you experience sudden pain or dislocation of the kneecap after a fall or accident, a doctor is required. Restrictions in the range of motion or poor knee resilience should be examined and treated. In some cases, bone structure irregularities appear after an unfortunate twisting motion of the leg or while engaging in sport or other physical activity. As soon as they are noticed, a relieving position should be adopted and the activity should be stopped. Sensory disturbances, paralysis of the leg or problems with blood circulation should be presented to a doctor.
Swelling, discoloration of the skin and sensitivity to pressure are signs of a health impairment. A doctor's visit is advisable so that there is no permanent damage when moving. If the kneecap is displaced without triggering momentum, a doctor is also required. The cause of the discomfort must be determined so that an optimal treatment plan can be created.
Limping, misalignment of the body or incorrect strain must be corrected by consulting a doctor. Otherwise there is a risk of lifelong damage and limitations to the musculoskeletal system. Insomnia, pain at rest or irritability should be presented to a doctor. Taking pain medication is only advisable after consulting a doctor, as there can be numerous complications.
Treatment & Therapy
The priority measure for a Patellar luxation is the reduction ("straightening") of the kneecap, which can also take place with painkillers in the case of pronounced pain. Further therapeutic measures in the case of patellar dislocations depend on the extent and causal trigger of the instability.
As part of conservative therapy, habitual patellar dislocations with less pronounced deviations in shape can be treated with physiotherapy to build up and strengthen the stabilizing muscles (especially vastus medialis muscles). If no improvement in symptoms can be observed after 3 to 6 months, surgical measures such as capsule rupture, arthroscopic division of the retinaculum or knee joint capsule tightening should be considered to correct the shape deviations.
In the case of traumatic patellar dislocations, minor form deviations are also initially treated conservatively. If these are accompanied by a joint capsule tear and / or hemorrhage, arthroscopic irrigation followed by physiotherapy is recommended.If the cartilage is detached or the medial patellar femoral ligament is ruptured, the cartilage fragments should be surgically attached and the ligament that stabilizes the kneecap should be replaced with the body's own material in a minimally invasive manner.
If the instability of the kneecap is based on cartilage damage, treatment is usually conservative, sparing the affected knee and, if necessary, using anti-inflammatory drugs. In the case of advanced cartilage wear, the triggering focus can be drilled ante- or retrograde to restore normal blood flow. To avoid so-called "joint mice" (free joint bodies), it may be necessary to surgically remove necrotic cartilage material. If necessary, a mosaic sculpture (cartilage transplantation) can be considered.
You can find your medication here
➔ Medicines for joint painOutlook & forecast
The prognosis of a patellar dislocation is generally favorable. If the health problems arise as a result of an accident, the kneecap is repositioned in a conservative treatment. This is followed by drug therapy to relieve existing pain. Normally the patient is discharged from treatment within a few weeks as symptom-free.
Many patients also receive physical therapy support. Movement sequences are optimized so that existing complaints are alleviated and a recurrence of the health irregularities is avoided.
In severe cases, surgery is necessary. Surgery puts you at increased risk of complications. Sudden inconsistencies can also occur in the subsequent wound healing process. The operation runs smoothly under optimal conditions. Physiotherapeutic support is also provided during the healing phase. These patients can be expected to recover within half a year.
If irreversible damage to the cartilage or the surrounding areas of the knee is documented, the prognosis worsens. Those affected can experience lifelong problems with locomotion. Coping with everyday life and performing sporting activities are then restricted. As a result, mental disorders can occur due to the emotional burden. There is also the possibility that professional tasks can no longer be adequately fulfilled.
prevention
In the case of congenital deviations in shape within the knee joint, prophylactic measures to reduce the risk of Patellar dislocations only possible to a limited extent. Consistent training of the stabilizing thigh muscles can, however, prevent reluxation of the kneecap.
Aftercare
In most cases of patellar luxation, those affected have only a few or only limited follow-up measures available. First and foremost, those affected must consult a doctor early on so that there are no further complications or further worsening of the symptoms. An early diagnosis usually has a very positive effect on the further course of the disease.
In most cases, patients are dependent on taking various medications that can relieve the symptoms. Those affected should pay attention to the prescribed intake in order to limit the symptoms accordingly. Consult a doctor first if there are side effects or if anything is unclear.
Furthermore, in the case of patellar dislocation, physiotherapy or physiotherapy measures may be necessary to alleviate the symptoms. Many of the exercises can also be repeated at home, which speeds healing. Regular checks by a doctor are also very important so that further damage can be recognized and treated at an early stage. The luxation of the patella usually does not limit the life expectancy of the person affected.
You can do that yourself
If the knee joint is discomfort after a fall or an accident, the person affected should consult a doctor as soon as possible. He needs medical care, as the damage to the knee joint cannot be sufficiently regenerated during the self-healing process of the organism.
In the case of a patellar luxation, the person affected should take sufficient care of himself and his body. Cooling compresses also help with swelling. Physical strain or overexertion should be avoided. The movement sequences must be optimized so that as few complaints or sequelae occur as possible. Unilateral physical strain and poor posture are to be compensated for immediately if possible. It is helpful to restructure the handling of everyday tasks. The support of people from the close environment should be used.
To ensure that the skeletal system and the joints are as little stressed as possible, obesity should generally be avoided. The weight should be in the normal range of the BMI. If you are overweight, it is important to change your lifestyle and diet. Excess weight can be lost through a balanced diet rich in vitamins. In addition, the consumption of harmful substances such as nicotine or alcohol is to be avoided.
In principle, it is advisable to work closely with a doctor and physiotherapist for this disease. This ensures that the healing process is optimal.

.jpg)
.jpg)

.jpg)