Of the peristaltic reflex is a movement reflex in the intestine. The reflex is triggered by pressure on the mechanoreceptors located in the intestine. The nervous system of the intestine is relatively autonomous, so that the reflex can still be observed in an isolated intestine. In diseases such as diabetes, the reflex can come to a standstill.
What is the peristaltic reflex?

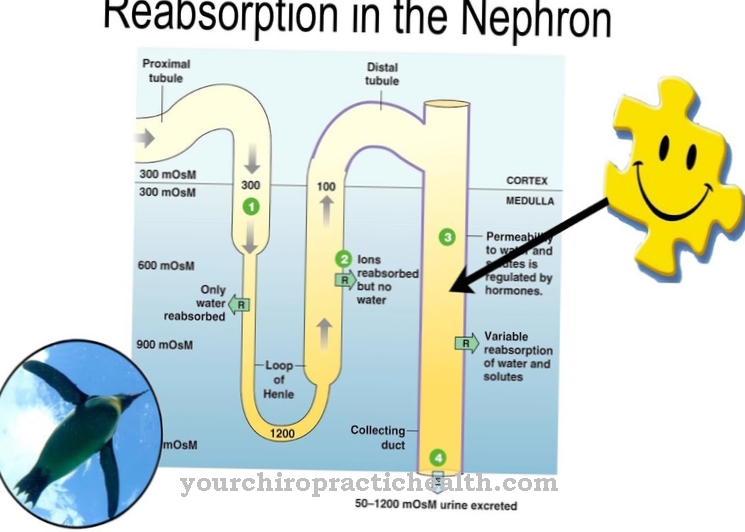
The movements of the intestine are called peristalsis. Different movement patterns of peristalsis are distinguished. The so-called pacemaker cells of the intestine, for example, control slow potential waves every second or minute.
During digestion, non-propulsive peristalsis occurs in the form of ring-shaped contractions. The intestinal contents are transported in the direction of the rectum via propulsive peristalsis. Continuous contractions in various intestinal areas prevent the contents of the intestine from moving upwards.
The peristaltic reflex is the triggering of the characteristic intestinal peristalsis by a stretching stimulus. Physiologically, the contents of the intestine give the stimulus to stretch to trigger the digestive movements. The fuller the intestine, the more the intestinal contents stimulate the so-called mechanoreceptors of the intestinal mucosa.
When a threshold potential is exceeded, the enterochromaffin cells in the intestinal walls release serotonin. It is a messenger substance of the enteric nervous system. The serotonin excites the nerve cells in the intestinal wall and thus triggers muscle contractions or relaxation. Thanks to the messenger substance, the reflex is independent of the central nervous system and can also be observed in the isolated intestine.
Function & task
In the human organism there are different nervous systems that act relatively independently of one another. In addition to the central nervous system, the vegetative nervous system should be mentioned. The enteric nervous system, together with the sympathetic and parasympathetic nervous systems, form the vegetative system. The enteric nervous system is the autonomic nervous system of the gastrointestinal tract, which is similar in structure to the brain. For this reason, the gastrointestinal tract is also known as the small brain.
Extrinsic sympathetic and parasympathetic nerve tracts monitor and regulate the intestinal motor skills, but ultimately the gastrointestinal tract is the only organ that is still able to work in isolation from the central nervous system. All motor functions of the anatomical structure are controlled almost autonomously.
Enteric motor skills are reflex motor skills. The digestion is therefore involuntary and independent of one's own decisions. The maintenance of all digestive movements is the job of the enteric nervous system.
Enteric nerve cells synthesize more than 25 transmitter substances for communication purposes. In theory, more than 1,000 different transmitter combinations are available to control gastrointestinal motor functions. Around 30 populations function as sensory neurons, motor neurons, and interneurons and harbor neurotransmitters.
The main function of the enteric nervous system is synaptically mediated activation and inhibition. Fast-arousing postsynaptic potentials are one of the most important transmission mechanisms. Acetylcholine is the primary neurotransmitter in the enteric nervous system. It activates postsynaptic nerve cells by binding to nicotinic receptors. Serotonin and adenosine triphosphate also participate in the mediation. Serotonin binds to 5-HT3 receptors.
The enteric nervous system regulates its effector systems through reflex circuitry. The peristaltic reflex forms the propulsive peristalsis. The IPAN (intrinsic primarily afferent neurons) in the enteric nervous system are stimulated by the mechanical pressure of the intestinal contents or by chemical stimuli and initiate a reflex circuit that causes a higher-lying contraction and a lower-lying relaxation of the circular muscles.
The projection polarity of the enteric motor neurons ensures proper functioning. Inhibiting and exciting motor neurons can be directly controlled by the IPAN. The IPAN can, however, also use an interposed interneuron for indirect activation. The interconnection runs over distances from millimeters to centimeters. Several of these circuits are activated in immediate succession.
The transport of the intestinal contents receives its modulation by activating or inhibiting synaptic contacts between the circuit elements.
You can find your medication here
➔ Medication for diarrheaIllnesses & ailments
Pathological hyperactivities of inhibiting nerve cells in the intestine cause the intestinal muscles to relax so extremely that there is almost atony. In extreme cases, the peristaltic reflex comes to a standstill. Even complete paralysis of the intestine can occur in this way. The peristaltic reflex can then no longer be triggered. The resident mechanoreceptors no longer register stimuli even when the intestinal wall is tight. The opposite condition can also have a disease value, for example in the case of a pathological hyperactivity of the excitation system. Such hyperactivity results in accelerated transportation and diarrhea.
Many intestinal diseases are associated with functional obstruction. Some of these diseases arise from neuronal degeneration, which can take on different dimensions. Generalized degeneration affects, for example, the inhibitory and excitatory nerve cell populations of the enteric nervous system. If the inhibiting nerves fail, the consequences are more serious than failure of the excitatory cells. The inhibiting nerve cells of the intestine maintain a braking effect on bowel movement.
The complete elimination of the inhibitory tone can result in clinical pictures such as Hirschsprung's disease, achalasia or stenoses of the sphincters. Each of these diseases can be rooted in local aganglionosis. With hypoganglionosis, intestinal pseudo-obstructions develop. These relationships play a role, for example, as causes of dysfunction in Chagas disease and cytomegalovirus infection.
Diabetes mellitus can also interfere with enteric circuits. In this case, the dysfunctions express themselves primarily in the slow emptying of the stomach, which can increase to an apparent paresis.
Neurological diseases such as multiple sclerosis do not attack the enteric but the central nervous system. All associated intestinal disorders have a sympathetic or parasympathetic cause and are not in the intestine itself.


.jpg)