Serratia or Serratia, as they are also called, belong to the family of intestinal bacteria (enterobacteria). The majority of pathogens are harmless to people with an intact immune system. However, they pose a great risk in hospitals and infant wards.
What are Serratia?
Serratia is the name of a rod bacterium that was discovered in 1819 by the Italian pharmacist and physicist Bartolomeo Bizio. He found it on rotten polenta and named it after Serafino Serrati, an 18th-century physicist he admired.
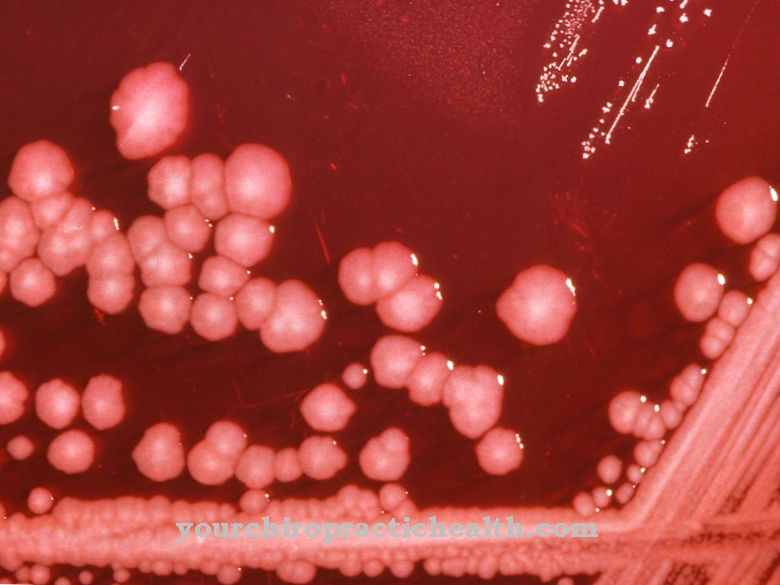
15 species belong to the genus Serratia. Serratia marcescens is the most common type of bacterium. It was given the names miracle bacillus and host fungus because it forms reddish pigments on hosts that resemble drops of blood. The discoloration was considered a divine miracle at the time.
Occurrence, Distribution & Properties
Serratia occur, except in the human and animal intestinal flora, in the soil, water and even in plants. The individual Serratia species differ in terms of the habitats they choose. Colored Serratia tribes prefer freshwater habitats such as spring water and wells, non-pigmented ones prefer the water of rivers.
Pathogens living on plants and vegetables have the task of breaking down the organic material. In addition, Serratia strains can be detected in foods such as eggs, poultry meat and dairy products.
Since the rod bacterium is found in all types of media around the world, it is almost impossible not to come into contact with it. Another way of transmission is from person to person. In order to become infected via droplets containing serratia, it is sufficient to cough briefly and sneeze on.
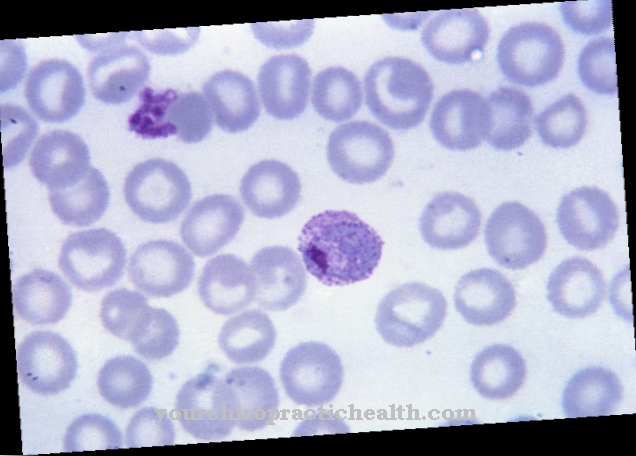
Serratia can live aerobically, but also anaerobically and is gram-negative. The pathogen moves with the help of tiny flagella. It does not form spores. Most Serratia cultures grown on solid media are reddish or pink in color. Some serratia types are non-pigmented. The discoloration is due to the prodigiosin produced by the serratia concerned.
The bacteria feed on carbohydrates such as glucose, fructose, galactose, maltose and some sugar alcohols. Acids and gases are produced as by-products. Some representatives of enterobacteria such as Serratia odorifera give off an intense potato-like odor.
Serratia are able to produce beta-lactamases. These enzymes make the use of beta-lactam antibiotics ineffective by breaking down their beta-lactam ring. Serratia bacteria grow optimally at temperatures between 20 and 37 ° C and a pH value of up to 9. They form the virulence factors gelatinase, DNAse, lipase, endotoxin and bacteriocin.
Serratia marcescens can cause the deadly white pox disease in Acrospora corals, which now threatens large parts of coral reefs worldwide. The coral death is triggered by Serratia pathogens that come from sewage that is discharged untreated into the sea water.
You can find your medication here
➔ Medicines to strengthen the defense and immune systemIllnesses & ailments
Serratia is completely harmless to most people. However, enterobacteria can cause serious infections in people with a weakened immune system and in newborns. This usually happens during hospital stays. Those affected come into contact with the bacterium in the intensive care unit.
The insertion of endoprostheses also carries a high risk of becoming infected with serratia. Enterobacteria enter the human body via contaminated infusion solutions and catheters. In the worst case, blood poisoning (sepsis) is the result.
The most dangerous to the human body are Serratia marcescens and Serratia liquefaciens. Sick people who are treated as inpatients are more at risk of contracting the pathogen than sick people who are treated on an outpatient basis. The infection rate is around two percent for urinary tract inflammation and one percent for blood poisoning and pneumonia (based on outpatient treatment). In addition, infants (premature babies) and nursing homes are sometimes infected with the bacterium. The causes are poor hygiene and insufficient disinfection of the implants and cannulas used.
Newborn children, especially premature babies, are at great risk because their immune systems are not yet fully developed. They also have thinner skin, so the serratia can enter their bodies more easily. People who take drugs intravenously also have an increased risk of contracting an infection caused by the bacterium.
Serratia can trigger various diseases. These include sepsis (blood poisoning), respiratory infections to pneumonia, urinary tract infections, meningitis (inflammation of the brain), wound infections, endocarditis (inflammation of the inner lining of the heart) and osteomyelitis (inflammation of the bone marrow).
Few species of Serratia can be effectively controlled with antibiotics. The pathogens are resistant to cephalosporins. In order to find the right drug, an antibiogram is made (resistance test). Proven remedies are acylaminopenicillins, aminoglycosides such as amikacin and ciprofloxacin. In addition, carbapenems (meropenem, imipenem) are helpful in the treatment of diseases caused by serratia.













.jpg)