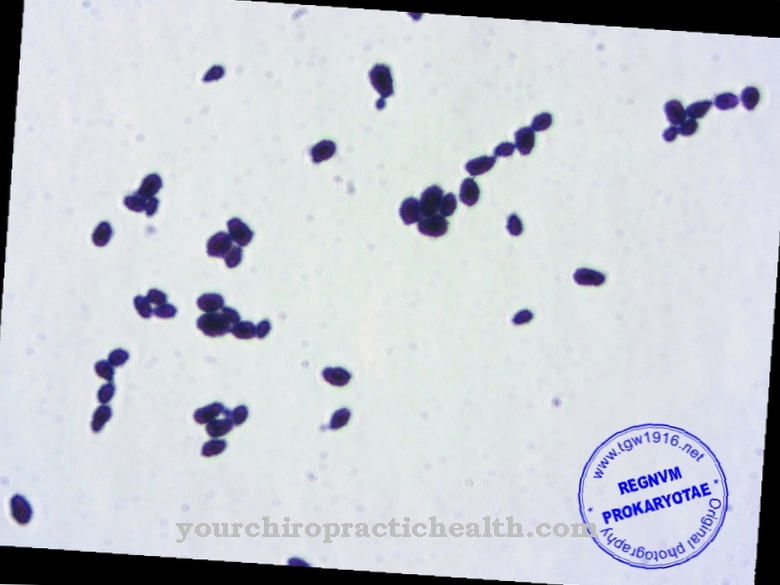
Staphylococcus epidermidis is a gram-positive bacterium that colonizes human skin and mucous membranes as a saprophage. The bacterium is not pathogenic for people with an intact immune system. However, it can become lodged on the polymeric plastic surfaces of implanted objects such as catheters and artificial heart valves, form a biofilm and cause the most severe nosocomial infections.
What is Staphylococcus Epidermidis?
The gram-positive and plasma-coagulase-negative bacterium Staphylococcus epidermidis feeds as saprophage on dead skin cells and other breakdown products from skin and mucous membranes. The fact that the bacterium is plasma coagulase-negative means that when it enters the body it cannot produce a substance that activates prothrombin, so that the bacterium cannot - like some related species - surround itself with a protective shield made of the body's own proteins.
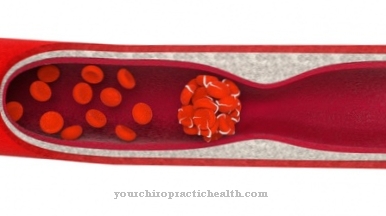
Staphylococcus epidermidis is therefore not pathogenic for people with an intact immune system. The bacterium, however, has the unpleasant property of being able to attach itself easily to implanted objects with a polymeric plastic surface. It then forms a multi-layered, well-adhering biofilm that is protected with a membrane-like glycocalyx made from exopolysaccharides. If the bacteria attach to endoprostheses, artificial heart valves and catheters, they can cause serious nosocomial infections.
Staphylococcus epidermidis can therefore be described as facultative pathogenic. Often such infections are difficult to treat when the bacterium is a multi-resistant strain that is insensitive to most antibiotics.
Occurrence, Distribution & Properties
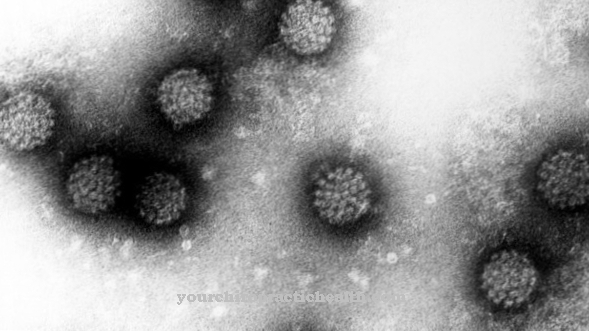
The bacterium Staphylococcus epidermidis is almost spherical and colonizes - as the name suggests - human skin and mucous membranes and is almost omnipresent there. The bacterium forms a large part of the local flora (normal flora) of the skin. The bacteria can also be found on food and in water. An effective and complete protection against external contact with the bacteria or against oral ingestion is practically not possible and also not necessary. The bacterium also has properties and functions that are useful for humans.
Its facultative pathogenicity lies in its ability to colonize invasively introduced materials with a polymer surface and to protect itself through a membrane-like structure, so that the bacterium cannot be reached by either the immune system or antibiotics. There are also strains in clinics that are resistant to penicillin and methicillin, as well as some other antibiotics. They are therefore counted among the dangerous multi-resistant germs that are difficult to control.
Meaning & function
The bacterium Staphylococcus epidermidis feed on flaking horn cells and other breakdown products of the body. The bacteria therefore dominate the composition of the local flora of the skin. The flora of the site normally represents a stable, dynamic equilibrium that results from a complex interaction of different microorganisms. For example, Staphylococcus epidermidis is also capable of effective defense reactions against competing bacteria such as Staphylococcus aureus. The bacterium with a high and feared pathogenicity can attack the immune system by destroying phagocytes and causing life-threatening infections.
Staphylococcus epidermidis can synthesize an enzyme that destroys the protective biofilm of Staphylococcus aureus and prevents the bacterium from building up a new protective film. Staphylococcus epidermidis knows how to include the body's own immune system in the complex defense process through appropriate stimulation.
These effects were demonstrated by Japanese researchers in 2010 for the area of the nasal mucosa. In the nasal mucous membrane, Staphylococcus epidermidis normally exercises a particularly dominant "predominance". In this case, the bacterium exercises an active, immune-supporting, important defense against infection, although it is classified as facultative pathogenic.
The effective defense against the bacterium Staphylococcus aureus by certain strains of Staphylococcus epidermidis is very likely the reason why some people seem immune to a dangerous infection by Staphylococcus aureus.
Illnesses & ailments
The greatest danger posed by the otherwise harmless and even useful bacterium Staphylococcus epidermidis is its ability to colonize artificial objects such as endoprostheses, catheters or artificial heart valves and to establish themselves in a protective, membrane-like biofilm. In particular, objects with surfaces made of polymeric plastics or metal are preferred by the bacterium for colonization.
The occupation of the objects can trigger a so-called foreign body infection, which can sometimes be severe. About 70 to 80 percent of all foreign body infections are caused by the bacterium Staphylococcus epidermidis. Such an infection is particularly feared in clinics, as it is mostly caused by bacterial strains with multi-resistance to penicillin, methicillin and other antibiotics and embody typical nosocomial infections.
If food is contaminated with the bacterium and offers good conditions for it to reproduce, consumption can cause nausea, vomiting, diarrhea and cramps. However, it is not an infection in the classic sense, because Staphylococcus usually cannot survive in the digestive tract. It is basically food poisoning, as the symptoms of the disease are caused by the toxins that the bacteria produced in the food before it was consumed. As a rule, the symptoms subside relatively quickly once the contaminated food has left the body due to the accelerated digestive passage.
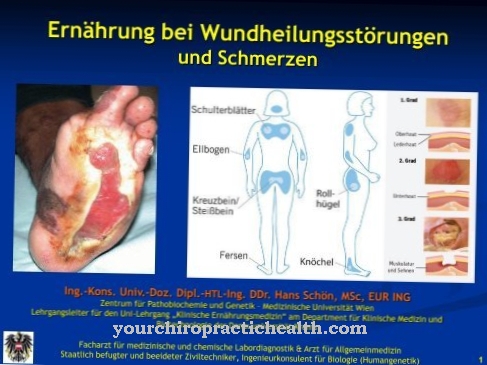
In people with a weakened or artificially suppressed (suppressed) immune system, Staphylococcus epidermidis can cause wound infections, boils, sinus infections, and other inflammatory diseases.
The biggest problem when an infection with Staphylococcus epidermidis occurs is the fact that the bacterium retreats into "hiding places" where it is not noticed by the immune system and therefore not combated. As soon as the conditions for a renewed infection are favorable for the bacterium, the bacterium settles again and creates new - often chronic - inflammation foci, which are difficult to combat due to the multi-resistance.






.jpg)
.jpg)



.jpg)