typhus has been known since the middle of the 16th century and has been explored more and more over the centuries. It is a disease that is widespread worldwide to this day and is mainly due to poor hygiene. Around 20 million people worldwide develop typhoid fever every year, and the disease has a fatal outcome for around 200,000.
What is typhoid?

The disease is mainly common in developing countries and plays a minor role in Europe and North America. It is an infectious disease that manifests itself as fever and diarrhea.
It is transmitted by the "Salmonella Typhi" bacteria. During the incubation period (usually about 6-30 days), the pathogens penetrate the intestinal wall. They then enter the bloodstream via the lymphatic system and trigger the actual disease. The name of salmonella is derived from the ancient Greek word "typhos", which means "haze" or "fog". This term was used because patients complained of a "foggy state of mind".
Over time, the name of the pathogen officially became “Salmonella enterica ssp. enterica Serovar Typhi ”, whereby both terms are still used. The disease is often referred to as "typhus". A distinction is made between the actual "Typhus abdominalis" (abdominal typhus or abdominal typhus) and a weaker form of the disease, the so-called "Paratyphus".
causes
As mentioned earlier, the infection is caused by bacteria. After major typhoid epidemics at the beginning of the 20th century, research into the disease found that the transmission of the bacteria is mainly "faecal-oral". At this point in time, human awareness of hygiene was not very high.
The bacteria were often spread via food and drinking water. A practical example of this is the non-existent or poorly existing separation of latrines from cooking areas, drinking water supply or storage facilities. In addition, little importance was attached to washing hands. Intensive cleaning of hands after using the toilet, before operations or in relation to kitchen hygiene only became mandatory after this knowledge.
These are also the reasons why typhoid fever nowadays mainly occurs in poorer so-called third world countries that have poorer infrastructure. A direct transmission from person to person is possible but very unlikely. The greatest risk of infection is from smeared food or water. There is an increased risk of infection in children up to the age of nine or people with a weakened immune system.
Symptoms, ailments & signs
The most common symptoms of typhoid fever are headache, fever, fatigue and severe gastrointestinal discomfort. The course of the disease is basically divided into four stages, in which the symptoms sometimes vary.
In the initial stage, symptoms are often limited to common symptoms of a cold, such as headache and body aches and a slightly elevated temperature. In the following stages, the fever intensifies and settles at a high level. There is also an increase in gastrointestinal complaints in the form of abdominal pain, constipation or diarrhea.
Patients often suffer from anorexia and apathy or, in rare cases, even from impaired consciousness. A characteristic symptom during this period is a grayish coated tongue, which is called the "typhus tongue". In the final, most complicated stage, the intestinal complaints usually worsen and the general condition deteriorates due to fluid loss and weight loss.
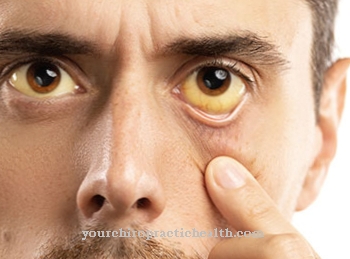
At this stage a typical form of diarrhea occurs called "pea-like" diarrhea. With this, the patient gradually excretes the pathogens. There is therefore a high risk of infection at this time. A rather rare but extremely characteristic symptom are "roseoles". This is a reddish skin rash in the form of spots on the stomach and upper body. In rare cases, spleen swelling occurs.
Complications
Complications during the untreated course of the disease cannot be ruled out, especially in the last two stages. The intestinal tract in particular is a major source of danger.Due to the heavy use of this area (weakened by nesting of the pathogen, diarrhea or constipation) there is an increased risk of intestinal bleeding or intestinal perforation (intestinal perforation).
The latter carries a high risk of a lethal outcome. Other complications that may occur are the formation of blood clots or thrombosis, inflammation of the bone marrow or heart muscle and meningitis (inflammation of the meninges). General damage to the muscle or bone system due to exhaustion cannot be ruled out either. Children under one year of age represent a special risk group. Infected people in this age group often develop complications despite treatment.
The "permanent eliminators" represent a particular danger. Usually, after overcoming the disease (regardless of whether with or without treatment), a patient can eliminate typhoid pathogens for up to 6 months. “Permanent excretors” are people who excrete pathogens for the rest of their lives without continuing to suffer from the disease themselves. This harbors a constant risk of infection for yourself and others.
Occasionally it happens that infected people become "permanent excretors" without ever developing symptoms of the disease themselves. According to studies by the World Health Organization (WHO), around three to five percent of those infected are “permanent exuders”.
When should you go to the doctor?
If you suspect a typhoid infection, it is of the utmost importance to consult a doctor immediately. It is irrelevant whether the suspicion of symptoms or possible infection is based on a trip to a particularly endangered country.
Treatment as early as possible is of enormous importance for the course of the disease. In this context, there is also the responsibility to pay attention to fellow human beings, since it is a contagious disease. Usually it is enough to go to a family doctor. If it becomes necessary to consult a specialist in the course of the illness, a referral can be made.
This may be necessary in the case of the aforementioned complications. As already mentioned, children under one year of age represent a special risk group. In such a case, the initial consultation of a specialist for this disease in children is recommended.
diagnosis
In the early stages of infection, diagnosis is difficult at first. The symptoms initially resemble more harmless illnesses such as the common cold, common fever or gastrointestinal infections. When the first symptoms appear, it is therefore extremely important to inform the attending physician about any previous trip to one of the aforementioned countries.
With this information and the existing suspicion of typhoid fever, therapeutic measures can be taken at an early stage. Otherwise an initial misdiagnosis cannot be ruled out. Typhoid fever is mainly diagnosed by detecting the pathogen in the blood.
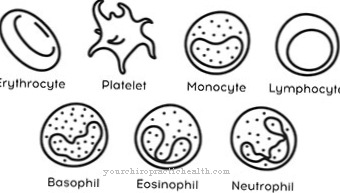
However, this is only possible after the incubation period and the penetration of the pathogen into the bloodstream. In the later course of the disease, when the bacteria begin to excrete in the stool, they can also be determined by examining the stool. At the beginning of the incubation period, a low number of leukocytes (white blood cells) may appear and this may indicate an infection.
Treatment & Therapy
Typhoid fever is generally treated with an antibiotic. In the past few decades, however, the pathogen has developed a very strong resistance to certain drugs. Therefore, new active ingredients are constantly being developed and used nowadays.
Apart from medication, patients are advised to drink enough fluids to accelerate the elimination of the pathogen. Do not take anti-diarrheal medication, as this makes it much more difficult for the bacteria to be eliminated.
The "permanent eliminators" are a specialty of the treatment. The pathogens often settle in these people in the gallbladder. If antibiotics do not help in such a case, surgical removal of the gallbladder must be considered.
Outlook & forecast
In Europe, North America and other countries with good medical care, the prognosis for typhoid fever is very good. With early and correct drug treatment, the death rate is less than one percent. In this case, the disease proceeds with little or no complications.
Consequential or long-term damage occurs only in the rarest of cases. Without appropriate treatment, the prognosis is much worse. There is a risk of the aforementioned complications and their consequences. It should also be noted that "permanent excretors" without treatment represent a long-term risk of infection for fellow human beings. The death rate increases significantly in these cases to up to twenty percent.
prevention
Typhus infection can in principle occur anywhere, so every person is exposed to a certain risk. A vaccination is possible as a preventive measure. This can be done either orally as a swallow vaccination or in syringe form. The oral vaccination is a live vaccination.
Here, weakened forms of the bacteria are introduced, which counteract the actual pathogen in the event of an infection. The second variant contains a dead vaccine, which mainly consists of dead cell parts of the bacteria that serve to fight an infection. Neither variant offers guaranteed protection.
Around sixty percent of those vaccinated have been shown to be protected. This usually lasts for one year. A vaccination is particularly useful when traveling to regions with poor hygiene. These include Asia, India, parts of South America and North Africa. During such a trip, increased caution with regard to hygiene can have a preventive effect.
This includes measures such as regular, thorough hand washing, boiling of drinking water and refraining from consuming raw food. By observing these behaviors, however, the risk of infection cannot be excluded, but only reduced.
Aftercare
Follow-up care for typhus includes a physical exam and a conversation with the doctor. As part of the aftercare, the symptoms will be examined again. Above all, the fever and the typical drowsiness must be clarified. If necessary, the patient can prescribe a drug or refer the patient to a specialist.
If the outcome is positive, the disease should subside after a few weeks. After the follow-up, the patient can be discharged. After a typhoid fever, the patient is immune for about a year. After this year is over, you should have another medical check-up. The same applies if the patient was exposed to a high dose of the pathogen.
A blood test shows whether there are still pathogens in the blood. In the case of chronic illnesses, a stool or urine sample may be sufficient evidence. If a chronic disease is suspected, an examination of the bone marrow can also be carried out, since the pathogens of typhoid and paratyphoid fever can still be found in the bone marrow weeks or months after recovery. The family doctor or an internist will take care of typhoid fever. If the symptoms persist, hospitalization is indicated.
You can do that yourself
Typhoid and paratyphoid fever are serious illnesses that require medical attention. If the typical typhoid symptoms occur on vacation or during a trip abroad, it is advisable to interrupt your trip. In Germany, the disease should be treated by an internist or general practitioner.
The pathogens are treated with antibiotics. The prescribed time intervals must be strictly observed when taking the medication. The medication should be continued until the end, even if the patient has recovered early. In order to avoid interactions, the doctor must be informed about any illnesses and the use of other medication. In addition, general measures such as rest and protection apply. Because the pathogens can settle in the gallbladder, attention must also be paid to any conspicuous symptoms that may persist beyond the actual disease.
The diet should be changed. Typhoid and paratyphoid patients best avoid raw and not well-cooked foods. Typhoid fever patients should also drink a lot. The electrolyte balance is balanced with isotonic drinks and a diet rich in vitamins and minerals. In order to avoid transmission of the pathogen to contact persons, good personal hygiene is also important. The doctor responsible can give further tips and advice on typhoid self-help.


.jpg)


















.jpg)



