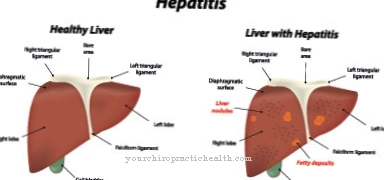
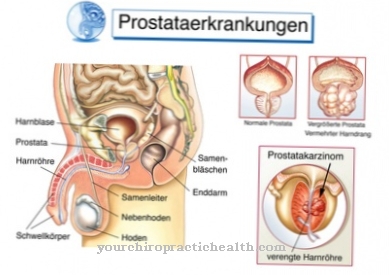
Hirschsprung's disease will also be congenital megacolon, Hirschsprung Disease or aganglionotic megacolon called. It is a disease of the colon. It is named after its discoverer Harald Hirschsprung, who first described the disease in 1886.
What is Hirschsprung's disease?

© LIGHTFIELD STUDIOS - stock.adobe.com
Hirschsprung's disease is included in the group of aganglionoses. Aganglionosis describes a congenital disease in which the nerve cells in the intestine are missing. This means that the bowel is generally disturbed in its mobility.
Hirschsprung's disease is congenital and occurs in about 1 in 5,000 newborns. Boys are more often affected than girls. Hirschsprung's disease is often seen in combination with Down's syndrome (around 12 percent of those affected also have Hirschsprung's disease).
Also in connection with other malformations such as cystic fibrosis are less common, but also occur. Usually only the rectum or the sigma is affected, with around five percent of those affected having a total of 40cm of the intestine. In another five percent of cases, there are no nerve cells in the entire intestinal section. In Hirschsprung's disease, the muscles in the intestine are overexcited.
As a result, it contracts convulsively and the section of the intestine is compressed. The bowel is no longer properly emptied when using the toilet, which leads to constipation. This in turn leads to stool congestion in the bowel and a megacolon, a chronic obstruction of the bowel. This leads to a bloated stomach and vomiting.
causes
The cause of ailments from Hirschsprung's disease is the lack of nerve cells in the colon. The ganglion cells are particularly affected here. This causes the intestinal section to contract convulsively. Due to the malformation of the nerve cells, more acetylcholine is released, an important neurotransmitter.
Causes of the disease that are remote from animals are a temporary reduced blood supply to the embryo, viral infections in the womb, maturation disorders or neuroblast immigration. Genetic changes can also be identified in connection with Hirschsprung's disease: Mutations in some genes could also be the cause.
Symptoms, ailments & signs
The first symptoms of Hirschsprung's disease usually appear in infancy. A distended stomach and the failure to settle the first bowel movement (meconium) are noticeable. Sometimes an intestinal obstruction even develops in the infant. However, there are also cases in which typical symptoms such as constant flatulence and chronic constipation only appear after the child has been weaned.
In these cases, only smaller areas of the colon are narrowed, so that the infants can still have a bowel movement by feeding on breast milk. This is possible under these conditions because the stool has a soft consistency due to the influence of breast milk and can still be transported through the small constriction of the intestine. However, this changes with the change in diet after weaning the infants.
The stool becomes firmer and thicker due to the fiber in the food. The transport no longer succeeds. The rectum remains empty because the feces can no longer pass through the constriction. The manure accumulates in front of the narrow point. The intestine expands more and more and becomes a so-called megacolon.
Some patients cannot have a bowel movement at all. Enormous amounts of feces remain within the intestines in the abdomen. Complications can include poisoning, intestinal perforations, purulent peritonitis and finally even potentially fatal sepsis (blood poisoning).
Diagnosis & course
The first signs of Hirschsprung's disease show up a few days after birth, when the normal meconium loss (so-called child bad luck) is absent in the newborn.
The stool in infants is called meconium. The doctor will then perform a rectal exam on the newborn. If a narrowed anal canal or an empty rectum can be observed here, these are further indications of a disease of Hirschsprung's disease. Hirschsprung's disease is rarely seen in adults.
When Hirschsprung's disease occurs in adulthood, the most common symptom is chronic constipation. If the diagnosis of Hirschsprung's disease is made in adulthood, it is usually the case that the affected section in the intestine is very short and is therefore only noticed late.
A serial suction biopsy from the mucous membrane in the rectum is required for diagnostic reliability: Tissue is removed from the intestine under general anesthesia, which can later be examined in the laboratory and thus adequately confirm the diagnosis of Hirschsprung's disease. If Hirschsprung's disease is left untreated, inflammation in the intestines can occur, such as enterocolitis, which can be fatal in around 40 percent of cases. It can also cause sepsis or peritonitis, an inflammation in the peritoneum.
Complications
With Hirschsprung's disease, those affected suffer from very unpleasant complaints. In most cases this leads to a bloated stomach and, not infrequently, to constipation. Furthermore, vomiting can occur, which significantly reduces the patient's quality of life.
In the worst case, it can also lead to an intestinal obstruction, which can be fatal for the person concerned. The symptoms of Hirschsprung's disease lead to considerable restrictions in everyday life for the patient. The anal canal is also narrowed, which can lead to pain when defecating. Various types of inflammation also occur in the intestine, which can lead to inflammation of the peritoneum.
As a rule, Hirschsprung's disease is treated with a surgical procedure. In most cases, there are no particular complications. In some cases, however, the creation of an artificial anus is necessary before an operation is possible. The procedure itself is carried out immediately after birth so that there are no complications or consequential damage in adulthood. Successful treatment will not reduce the patient's life expectancy.
When should you go to the doctor?
Since the disease occurs in many cases as early as infancy, parents of infants and young children should exercise increased vigilance. If there is little or no bowel movement, there is cause for concern and a pediatrician should be consulted. Simultaneous swelling of the stomach and intestines should also be examined and treated. If you experience unpleasant and persistent flatulence, constipation or chronic complaints, you need to see a doctor. If food is refused, the child shows behavioral problems or internal weakness occurs, a doctor should be consulted.
If children cry or cry over a long period of time, if they hardly react to the environment and if sleep disorders occur, a doctor's visit is necessary. Changes in the consistency of the excretions, pain in the organism or general malaise must be presented to a doctor. If there is a fever, severe internal restlessness and noticeable reddening of the skin, a doctor is required. A feeling of pressure inside the body often leads to discoloration of the skin and is to be interpreted as a warning signal, especially in children. In severe cases, an intestinal perforation occurs. Since there is a risk to life in these acute cases, an ambulance service must be contacted. Loss of consciousness is alarming and should be presented to a doctor immediately.
Treatment & Therapy
A definitive treatment of Hirschsprung's disease can only perform the surgical removal of the affected intestinal segment. However, this is risky with newborns, so that mostly temporary measures are taken first.
This includes the possibility of creating an artificial anus for the child. Another option is to flush the bowel regularly until the newborn child is stable enough to undergo surgery.
The temporary use of so-called intestinal tubes (a kind of catheter that is inserted into the anus) is a treatment option until an operation for Hirschsprung's disease is possible. However, this last option is rarely used.
You can find your medication here
➔ Medicines for constipation and intestinal problemsOutlook & forecast
The prognosis for Hirschsprung's disease can vary. Patients sometimes have no major impairments from the disease for a very long time. The prospects for the successful course of a treatment are good with early detection and the corresponding rapid patient care. In the case that only a few short pieces of intestine are affected, typical symptoms of the disease often take a long time to appear.
An operation is usually the method of choice. The operation for the disease generally shows very good results. However, as with any other surgery, some complications are possible. Although these complications are rare, they should be considered. As a rule, however, the benefits of the operation clearly outweigh the risks.
The general prognosis for patients is good in most of the cases, despite problems with continence and constipation. These problems can still occur even after surgical correction. In many cases, however, surgery is inevitable to prevent the life-threatening consequences of the disease. For affected children, however, the prognosis for Hirschsprung's disease is still unfavorable, although long-term survival can also be achieved in children through an intestinal transplant. A dreaded complication of Hirschsprung's disease is so-called Hirschsprung enterocolitis, which can be life-threatening.
prevention
There Hirschsprung's disease is a congenital disease, it cannot be prevented; it can only be remedied by surgery after a rapid diagnosis.
Aftercare
Hirschsprung's disease usually requires comprehensive, sometimes lifelong, aftercare. Immediately after the operation, the focus is on preventing wound infections, narrowing of the rectum and anus and tearing open the sutures (anastomotic leakage). In the long term, aftercare aims to avoid long-term effects such as incontinence, permanent constipation or intestinal inflammation.
Constrictions can develop, especially in the area of the surgical suture, which can lead to an intestinal obstruction. In order to identify possible late effects early on, a specialist regularly checks the width of the anal opening as part of the follow-up examinations that start just a few weeks after the operation. If the doctor notices a narrowing, a widening (bougiening) is necessary.
The parents of the affected children gradually expand the anal opening to the required width using metal pins (Hegar pins). The measure to be carried out daily at the beginning is mostly uncomfortable for parents and children, but it avoids constrictions that doctors can often only treat surgically later on.
In addition, in many cases the affected children need a longer time to take off their diapers. Overflow incontinence (urination disorder) can also play a role. Additional psychotherapeutic support takes care of possible emotional stress on those involved. Through nutritional counseling, children and parents learn a diet that aims for a loose stool that minimizes the risk of constipation.
You can do that yourself
The disease must be treated with medical intervention so that the infant does not become life-threatening. In this phase there are insufficient opportunities for self-help.Doctors' instructions and guidelines should be followed to avoid complications. The relatives of the child must be fully informed about the disease and its consequences. Any questions that arise must be clarified with the attending physician.
In addition, parents or legal guardians can find out about the disease themselves in specialist medical literature. There are various self-help groups for anorectal malformations across Germany that offer advice and assistance for patients and their relatives. There, patients and relatives receive tips for dealing with the disease in everyday life in an exchange of experiences. The focus of these groups is on promoting quality of life and building positive experiences. This stabilizes the psyche, which is an elementary component in coping with the disease in everyday life.
In the further course of life, nutrition is an essential element of self-help. It should be tailored to the needs of the patient. Pollutants are to be avoided and sufficient exercise promotes health. Fruits and vegetables should be consumed in sufficient quantities as they promote well-being.


.jpg)
.jpg)
.jpg)

.jpg)

.jpg)


.jpg)