The Nasal mucosa as a thin layer of tissue lines the entire nasal cavity without the nasal vestibule. It provides the first defense against bacteria, viruses or fungi invading the body. Inflammation of the nasal mucous membrane manifests itself as a runny nose (rhinitis).
What is the nasal mucosa?
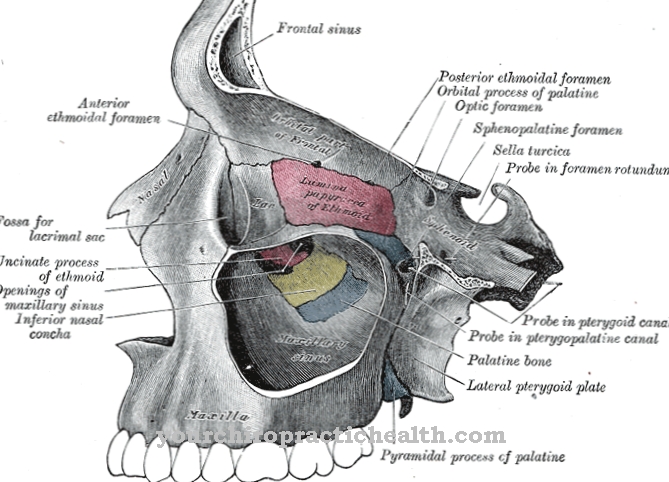
The nasal mucosa is a thin layer of tissue that forms mucus and lines almost the entire nasal cavity. The nasal vestibule is an exception. Instead of nasal mucosa, it is equipped with a cornified squamous epithelium. The nasal mucosa is divided into two regions. These are the regio olfactoria and the regio respiratoria. The olfactory region represents the olfactory mucous membrane and is located at the upper nasal entrance (meatus nasi superior).
It has special olfactory cells that serve to perceive smells. Otherwise, the respiratory region takes up almost the entire nasal cavity. It is equipped with a respiratory ciliated epithelium. The nasal mucous membrane is regenerated as part of the so-called nasal cycle. The nasal cycle represents the periodic swelling of the turbinates without the need for an external stimulus. It is controlled by the hypothalamus. With the help of the nasal cycle, the nasal mucous membrane stores moisture and at the same time humidifies the air we breathe.
Anatomy & structure
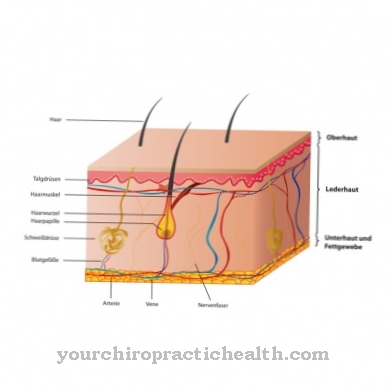
The nasal mucosa consists of three layers of tissue. This applies to both the respiratory mucous membrane of the nose and the olfactory mucosa. The respiratory nasal mucosa thus consists of the lamina propia, the basement membrane and a multi-row ciliated epithelium with goblet cells. The lamina propia is a thin layer of connective tissue located below the basement membrane. It contains a dense network of blood capillaries.
These are connected to a superficial venous plexus. The venous plexus regulates the change in volume of the erectile tissue and thus influences the modification of the air circulation. The basement membrane in turn consists of epithelial cells, which form the basis for the respiratory mucous membrane of the nose. The ciliated and goblet cells are formed from the basal cells. They are the only cells that get to the free surface. The basal cells are located in the basement membrane and are the stem cells for the regeneration of the ciliated and goblet cells. As gland cells, the goblet cells are responsible for the production of nasal secretions.
The olfactory mucosa in the upper nasal passage also consists of three layers of tissue. Two layers of this have a structure similar to that of the respiratory mucous membrane of the nose. These are also the lamina propia and the basement membrane. However, a specialized olfactory epithelium lies above the basement membrane. It consists of supporting cells and olfactory cells. The olfactory cells are neurons whose axons swim in the mucous layer. Below the supporting cells are the basal cells, which act as stem cells for the olfactory cells. The olfactory cells have a lifespan of 60 days and are repeatedly renewed from the stem cell reservoir.
Function & tasks
The nasal mucosa mainly serves to ward off infection. This task is carried out by the respiratory mucous membrane of the nose. First of all, pathogens are deposited through the mucus, which can then be transported away by the constant flicker. The nasal mucus consists of two layers. This is a thin layer of sol that lies under a discontinuous layer of gel.
The gel layer is transported through the cilia, which beat within the sol layer. At a pH of 7.5 to 7.6, the sol is transferred into the gel. The most important components of the nasal mucus are the mucins. They give the mucus its viscoelastic properties and are responsible for the immune response in various infections and the interaction with the existing microflora. The olfactory mucous membrane in turn has the task of absorbing odors and passing them on to the brain for processing. There the odor information is released for perception.
You can find your medication here
➔ Medicines for colds and nasal congestionDiseases
Diseases of the nasal mucous membrane are manifested either by increased mucus formation or by drying out of the nose. Often these symptoms are only symptoms of the underlying diseases. There are many reasons for increased mucus formation. It is a rhinitis, which is also known colloquially as a runny nose. There is often an infection with viruses. Of course there are also allergic forms of rhinitis.
The best-known example is the so-called hay fever, which occurs particularly in spring during pollen count. But other allergens also often trigger increased mucus formation in the nose. Sometimes a runny nose is triggered by harmless influences in the context of nasal hyperreactivity. Nasal hyperreactivity describes an oversensitive nose. It is caused by incorrect control of hormones, messenger substances and proteins. Chronic inflammation of the nasal mucosa can lead to polyps. Polyps are benign growths in the lining of the nose. However, they hinder nasal breathing and fuel further inflammatory processes. Therefore, nasal polyps should be surgically removed.
The causes of the chronic inflammation can be infections with viruses, bacteria or fungi. Allergic processes also play a role. Another problem of the nasal mucous membrane is its complete drying out. The beginning of a cold is often expressed in a dry nose. In this case, however, the problem is only temporary. When dry nose becomes a chronic condition, it can have serious health consequences.
Dry indoor air or extreme dust pollution often play a role in chronification. The dry nose manifests itself in obstructed nasal breathing, a feeling of dryness in the nose, deterioration in smelling ability or nosebleeds. Crusts and scabs form. Without treatment, the nose can lose its function completely. As a result, the susceptibility to infection increases. In rare cases, bacteria settle in the dry mucous membrane, which lead to unpleasant smells from the nose.
Typical & common nasal diseases
- Stuffy nose
- Nasal polyps
- Sinus infection







.jpg)
.jpg)

.jpg)