A rheumatic endocarditis (post-infectious endocarditis) is an inflammation of the inner lining of the heart caused by an autoimmune reaction of the body to certain streptococci. Most often children and adolescents are affected by rheumatic endocarditis, which is rare in industrialized countries these days.
What is rheumatic endocarditis?
.jpg)
© Rasi - stock.adobe.com
As rheumatic endocarditis is an inflammatory change in the inner lining of the heart (endocardium) caused by an immunological dysregulation of the organism (autoimmune reaction) after an infection with beta-hemolytic streptococci of group A and belongs to the symptomatic spectrum of rheumatic fever.
In most cases, rheumatic endocarditis affects the mitral and aortic valves, especially the valve edges that are subject to greater mechanical stress. Damage to the heart valves is a long-term consequence of rheumatic endocarditis. Here, adolescents and children, especially between the ages of 5 and 17, develop rheumatic endocarditis after an inflammation of the tonsils or throat caused by streptococci.
causes
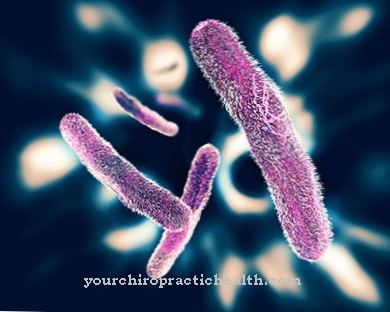
Rheumatic endocarditis (post-infectious endocarditis) is due to a dysregulation of the body's own immune system as a result of infection with group A beta-hemolytic streptococci.
Group A beta-hemolytic streptococci primarily cause inflammatory diseases of the pharynx such as tonsillitis (inflammation of the tonsils), pharyngitis (inflammation of the throat), scarlatina (scarlet fever) or otitis media (otitis media) and, in some cases, skin infections such as erysipelas or pyoderma ).
The rheumatic endocarditis is not due to colonization by streptococci, but rather to an autoimmune reaction of the organism. This forms so-called antibodies against specific protein components of the bacteria, which among other things resemble the proteins on the surface of the endocardial cells.
Since the antibodies also react incorrectly to endocardial structures (especially the heart valve), inflammatory changes occur, rheumatic endocarditis, which can thicken, roughen and stiffen the heart valves and ultimately limit their functionality.
Symptoms, ailments & signs
Rheumatic endocarditis is a symptom of rheumatic fever that can develop as a result of streptococcal infection. It usually takes two to three weeks before the first signs of inflammation of the inner lining of the heart appear. Palpitations (tachycardia) and irregular heartbeat (arrhythmia) occur.
The misdirected antibodies attach to the heart and trigger various reactions in the connective tissue, whereby the flaps thicken and the inner skin is roughened. This changes the murmur of the heart. Pain in the heart region and protruding neck veins are also possible. Since the heart no longer pumps adequately through the inflamed inner skin, it can lead to shortness of breath and reduced performance.
Often the valve leaflets stick together and contract due to the inflammation. As a result, they no longer close properly and lose their function as a valve; or they don't open wide enough, reducing blood flow from one chamber to the other. Since rheumatic endocarditis occurs as part of rheumatic fever, all the symptoms of this disease are also evident.
The typical symptoms are fever and a general feeling of illness. The joints are inflamed and painful, and the overlying skin is red and swollen. It usually starts with one joint and jumps to others. In addition, there are so-called rheumatoid nodules and red spots on the skin.
Diagnosis & course
An initial suspicion is based on rheumatic endocarditis (post-infectious endocarditis) on a previous infection with beta-hemolytic group A streptococci as well as characteristic symptoms such as abnormal heart murmur, high fever, tachycardia (increased heartbeat), general malaise and polyarthritis (joint pain) with pronounced pain to touch and shortness of breath.
The diagnosis of rheumatic endocarditis is confirmed by an echocardiogram (ultrasound of the heart) and an ECG, on the basis of which changes in the heart valves, an existing cardiac insufficiency or cardiac arrhythmia can be determined. The antibodies formed in the blood can be detected by a blood analysis. An increased CPR value, an increased concentration of white blood cells in the blood and an accelerated sedimentation rate (ESR) indicate rheumatic endocarditis.
After the start of therapy, rheumatic endocarditis usually subsides after 6 weeks (75 percent) or 3 months (90 percent), although the course can lengthen if the heart valve is heavily involved. If rheumatic endocarditis has not been treated, there is a 50 percent chance of recurrence with rheumatic endocarditis, which is also the most common cause of mitral valve stenosis.
Complications
Rheumatic endocarditis can cause heart valves to malfunction. This increases the risk of serious cardiovascular problems and heart attacks. The scarred changes in the heart valves permanently reduce the heart's function and thereby promote heart failure. The most serious complication of the inflammation of the inner lining of the heart is the spread of rheumatic fever to other regions and organs.
This can lead to secondary diseases such as acute polyarthritis and minor chorea. If the course is severe, multiple organ failure with fatal outcome is possible. If the inflammation is treated early, there are usually no major complications. However, antibiotics and anti-inflammatories are not free from side effects. Corresponding preparations can cause headaches, muscle and limb pain, skin irritations and gastrointestinal complaints.
Allergies and symptoms of intolerance can also occur. If cortisone is given, it can lead to an increase in blood fat, blood pressure and blood sugar. Possible long-term effects are osteoporosis or what is known as Cushing's syndrome. Heart surgery is always risky and can cause complications such as bleeding, cardiac arrhythmias and heart failure. Inflammation of the heart is life-threatening and represents a medical emergency that is accompanied by other complaints.
When should you go to the doctor?
With any form of endocarditis, it is important to see a doctor quickly. Because without treatment, it can only get worse. A visit to the family doctor is advisable as soon as the first symptoms appear. A general practitioner will identify the signs of post-infectious endocarditis. He can differentiate heart inflammation from other diseases with similar symptoms. If the fever is high, he can already prescribe antibiotics. In addition to a general examination, the family doctor will perform the first special tests. If the results indicate endocarditis, he will refer the patient to a heart specialist (cardiologist) as an urgent case.
They carry out more precise tests and start targeted treatment as quickly as possible. Unrecognized or untreated, the disease is often fatal because there is an acute risk of a heart attack. A stroke, pulmonary embolism or kidney embolism can also result from an untreated heart inflammation. If post-infectious endocarditis persists too long, the heart valves can be permanently damaged. In this case, surgery will be necessary.
Treatment & Therapy
A rheumatic endocarditis is primarily treated as part of antibiotic therapy (penicillin, but also macrolides) in order to kill any bacteria that may still be in the organism.
At the same time, the rheumatic complaints are treated with pain-relieving and anti-inflammatory drugs such as acetylsalicylic acid while at the same time protecting the body, especially the heart. In the case of pronounced rheumatic endocarditis, glucocorticoids and immunosuppressants are also used to reduce the overreaction of the immune system. If rheumatic endocarditis leads to severe heart valve damage due to the inflammatory changes, a surgical procedure (valve replacement) may be necessary.
In addition, after rheumatic endocarditis, antibiotic therapy is continued prophylactically as part of long-term therapy (usually monthly antibiotic injections) for the following five years. After rheumatic endocarditis has subsided, a thorough cardiological examination should be carried out in order to exclude possible damage to the heart valves or to be able to treat them early.
To prevent further inflammation of the pharynx, removal of the tonsils is also recommended. Endocarditis prophylaxis is recommended to those affected by rheumatic endocarditis before surgical and dental interventions.
You can find your medication here
➔ Medicines to strengthen the heart and circulatory systemprevention
There one rheumatic endocarditis is caused by an immunological dysregulation as a result of a streptococcal infection, preventive measures aim at an early and consistent treatment of the inflammatory diseases caused by streptococci such as tonsillitis (tonsillitis), scarlatina (scarlet fever) or otitis media (otitis media). Endocarditis prophylaxis before surgical or dental interventions also serves to prevent streptococcal infection and thus rheumatic endocarditis.
Aftercare
Rheumatic endocarditis (post-infectious endocarditis) is a bacterial autoimmune secondary disease. Follow-up care with complete healing is possible in principle. Because there is a risk of heart valve failure with this disease, rapid follow-up is very important. Taking antibiotics is essential. Here you should pay attention to the correct and regular intake.
In particularly severe cases, an additional intake of cortisone is necessary. Treatment with anti-inflammatory drugs, such as acetylsalicylic acid, is also recommended to reduce possible pain. In order not to put additional strain on the body and especially the heart, stress and physical work should be avoided and, in severe cases, bed rest should be observed.
After the disease with rheumatic endocarditis (post-infectious endocarditis), regular follow-up examinations are important in order to observe the healing process and, if necessary, to initiate further drug therapy. The rheumatic endocarditis (post-infectious endocarditis) heals after one to two months if the outcome is positive.
However, the prognosis depends very much on when the disease is recognized and whether the heart valve has been severely damaged. In severe cases, this can lead to chronic changes in the heart valve and, in extreme cases, require surgical intervention.
You can do that yourself
Rheumatic endocarditis is amenable to self-help, but requires treatment by specialists such as internists or cardiologists. Self-help in everyday life relates on the one hand to the acute illness, and on the other hand to aftercare and the prevention of a possible relapse of the illness.
The protection is an important factor with regard to the acute illness. Cooperation of the patient is crucial here. Physical exertion and sport should be avoided until the doctor allows them again. Inflammation of the body can often be positively influenced by sleeping in sufficient quantities and with plenty of fluids. Water and herbal teas are particularly recommended here. Do not use nicotine or alcohol. Protection from wind and weather is also important so as not to burden the body's weakened immune system.
Self-help is still possible even after surviving rheumatic endocarditis. On the one hand, to specifically build up your fitness again. This is best done in consultation with your family doctor or a specialized sports therapist in order to find the right exposure dose. Since rheumatic processes can also be influenced in a targeted manner by a healthy diet, it makes sense to switch these too. Mediterranean food with lots of fruit and vegetables instead of meat and sausage makes sense in this context. Sufficient drinking is also always important.



.jpg)







.jpg)

.jpg)
.jpg)











.jpg)