The Facial paralysis or Facial palsy is the paralysis of the 7th cranial nerve (nervus facialis), which enables the movement of the facial muscles. The paralysis usually shows on one side, typical is a drooping corner of the mouth and the lack of facial expression. Treatment of facial palsy is based on the cause.
What is facial paralysis?
.jpg)
© Henrie - stock.adobe.com
Facial paralysis or facial paralysis is a complete or partial paralysis or weakening of the facial nerve, so that the facial muscles can no longer be moved sufficiently.
A distinction is made between central and peripheral facial paralysis. Central facial paralysis is caused by damage to the origin of the nerve, namely the brain. The peripheral facial nerve palsy occurs through damage directly to the nerve.
Often, however, the cause of the paralysis is not known, in this case one speaks of idiopathic facial paralysis, that is: without a detectable cause. The idiopathic paralysis is also called Bell's palsy after the English doctor Charles Bell.
causes
The most common facial palsy is idiopathic, which means that in most cases the cause of the facial paralysis is unknown. Peripheral paralysis, when the damage is directly to the nerve, can have various triggers. There is often inflammation, such as otitis media or zoster oticus, a herpes infection on the ear.
Injuries such as fractures to the skull can also impair the functioning of the nerve. Tumors in the ear that press on the facial nerve as they grow can also be responsible for peripheral facial palsy. Central facial palsy is triggered by damage in the brain where the nerve originates. The facial nerve remains intact and is not itself damaged, it can only no longer transport information from and to the brain.
Common causes of central facial nerve palsy are a stroke or a brain tumor. In the case of a stroke, the area of origin of the facial nerve is damaged by bleeding or an undersupply; in the case of a brain tumor, the growing tumor presses on the area, so that the functions are disturbed and the facial nerve palsy occurs.
Symptoms, ailments & signs
Since the facial nerve supplies the facial muscles, a failure leads to characteristic, half-sided changes in facial expression. In the case of mild facial paralysis, the symptoms are only discreet; the asymmetrical changes become more clear in the case of more severe paresis. In terms of symptoms, peripheral and central facial paralysis can be distinguished from one another.
Both central and peripheral paralysis are associated with a drooping corner of the mouth and incomplete or incomplete eyelid closure on the affected side. Things like whistling, smiling or drinking become difficult or even impossible. The "Bell phenomenon" is the fact that when you try to close the eyelid, the typical upward turning of the eyeball becomes visible.
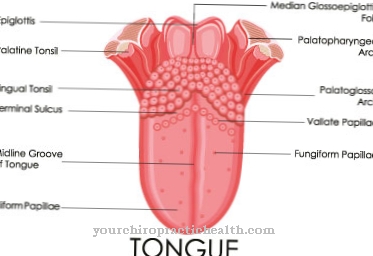
In the case of peripheral, in contrast to central paralysis, it is also not possible for the patient to frown on the affected side. Since the facial nerve is also responsible for some of the taste sensations on our tongue, taste disorders can result as a result of damage.
Another symptom is reduced saliva and tear secretion. In combination with incomplete eyelid closure, this harbors the risk of corneal damage due to drying out of the eye. Some patients also complain of hypersensitivity to noise with pain on the affected side behind the ear.
Diagnosis & course
The typical symptom of facial palsy is the unilateral sagging facial muscles. One corner of the mouth is drooping, one eye can no longer be completely closed and the forehead cannot be wrinkled. The entire facial expression looks slightly shifted. If there is a central facial nerve palsy, other complaints can also arise.
The flow of saliva becomes less and since the nerve also supplies the tongue, the ability to taste can be reduced (see taste disturbance). The formation of tear fluid can also be reduced, and the eye on the affected side becomes dry. The pronunciation also suffers from facial nerve palsy, as the lip and tongue muscles cannot articulate properly, i.e. the sounds can no longer be formed correctly.
The doctor sees the first indication of facial palsy from the obvious signs of paralysis. The patient's medical history as well as various tests, a blood test to rule out infections, x-rays of the skull, electromyography to measure nerve conductivity or a CSF examination (removal of fluid from the spine) provide further information.
These examinations first identify the cause and then the correct treatment for facial palsy.
Complications
The complications to be expected with facial paralysis (facial paralysis) depend on what caused the paralysis. Often, otitis media (otitis media) is the trigger for facial paralysis. The inflammation caused by bacteria can be accompanied by severe pain and a number of other complications.
Due to the proximity of the facial nerve to the ear, there is a risk that the infection could spread and permanent damage to the facial nerve in severe infections. Facial paralysis can also be the result of Lyme disease. The bacterium Borrelia Burgdorferi causing the infection is transmitted by ticks. The disease progresses in phases in different stages.
First, the so-called wandering redness (erythema migrans) as well as unspecific signs such as headache and body aches, a feeling of weakness and fever appear. In the next stage, paralysis along the puncture site or facial paralysis in conjunction with swelling of the lymph nodes may occur. Lyme disease can also cause permanent damage to the facial nerve.
In severe cases, facial expressions are permanently restricted, the face can look crooked and the corners of the eyes and mouth hang down. Occasionally, the shingles trigger, the herpes zoster virus, affects the ear and ear canal. The virus can then spread to the facial nerve and cause temporary paralysis. Permanent damage to the nerve is rare in these cases. However, the infection is usually extremely painful.
When should you go to the doctor?
If signs of facial paralysis are noticed, a doctor should be consulted. Most of the time the symptoms are due to a serious illness that must be clarified. Only a doctor can determine whether this is a facial nerve palsy. A doctor's visit is required at the latest when complications arise.
If, for example, an inflammation develops, this must be clarified immediately and treated if necessary. Medical advice is also required if symptoms of Lyme disease are added. Signs such as headache and body aches, fever, and the typical wandering redness indicate that the facial paralysis is an infectious disease that needs treatment.
People who suffer from facial deformities due to facial paralysis being treated too late should consult a specialist. The risk groups - including people who recently suffered from a herpes infection on the ear, an otitis media or a tumor in the ear - should speak to their family doctor immediately if the warning signs mentioned above occur. Patients who suffer from corresponding symptoms after a stroke or a brain tumor should consult the responsible doctor. Medical treatment is required in any case with facial paralysis.
Doctors & therapists in your area
Treatment & Therapy
About 70 percent of the facial paralysis that occurs heal completely. Treatment is always based on the cause. When facial palsy is caused by a bacterial infection, antibiotics are usually given. In the case of viral inflammation (triggered by viruses) so-called antivirals help, which prevent the virus from multiplying.
If the facial nerve is damaged by an injury, surgery can restore the nerve to function. Movement exercises are also necessary to train the facial muscles. Occupational therapists or physiotherapists are responsible for this. If the facial nerve palsy is caused by a pathological process in the brain, inpatient treatment is unavoidable.
The dryness of the eye that occurs with facial paralysis can be relieved with an ointment or artificial tear fluid. It is advisable to cover the eye with a bandage overnight to prevent it from drying out. If the facial nerve palsy is idiopathic, treatment is focused on alleviating the symptoms, with cortisone being used as a support.
Outlook & forecast
The cause of a fascial palsy (facial paralysis) determines the prognosis. The severity of the disease as well as the individual symptoms and the age of the affected patient also influence how the disease progresses. In general, it must be assumed that the chance of a complete cure decreases with age.
Especially with idiopathic facial paralysis, the chance of a cure is very good. If the therapy is carried out correctly, the symptoms decrease significantly in 90 percent of those affected. After about four months, more than two thirds of these patients can also be found to have completely healed. However, depending on the severity of the injury to the seventh cranial nerve, complete healing can take several years, although such long therapies are rare.
If it is a peripheral or central facial paralysis, then the prognosis looks bad. Of course, the extent of the damage is also decisive here. In the case of complete paralysis, treatment that was carried out too late or wrong medication, the prognosis is rather negative.
In many cases, this leads to incomplete regeneration, which is referred to as so-called defect healing. In retrospect, patients can still suffer from twitching, increased tension in the facial muscles or uncontrollable flow of tears. Under certain circumstances, however, it is conceivable to restore the destroyed nerve fibers in an operation.
prevention
Direct prevention of facial palsy is not possible as it most often occurs with an unknown cause. In the presence of a causative disease, immediate treatment is recommended in order not to damage the nerves and possibly prevent facial palsy.
Aftercare
With facial paralysis, in most cases there are no special follow-up options available to those affected. These depend primarily on proper treatment of the disease to prevent further complications. The focus is on identifying and treating the cause of facial palsy in order to prevent it from spreading to the entire body.
The earlier the disease is recognized, the better the further course of the disease. In most cases, facial palsy is treated with the help of drugs. Those affected must ensure that the dosage is correct and that it is taken regularly, although in the case of children, the parents in particular have to control the intake.
A doctor should be consulted in the event of side effects or uncertainties. Furthermore, some symptoms of facial paralysis can be treated with the help of physiotherapy. Many of the exercises from this physiotherapy can also be performed in your own home to restore muscle movement. As a rule, the life expectancy of the person affected is not restricted by the facial paralysis. It is often useful to have contact with other people affected by this disease.
You can do that yourself
In addition to medical treatment, those affected have several options for self-help.
In the case of paid therapies, it is advisable to discuss this with the health insurance company in advance. These include lymphatic drainage, acupuncture, physiotherapeutic measures and an appointment with an osteopath. The globules Aconitum C9 and Causticum C5 have proven themselves in homeopathy. The intake of vitamin B is also said to provide relief, but has not been statistically proven. The same applies to treatment with light showers.
Facial gymnastics and facial expressions can be carried out at any time. Not only the exertion, but also relaxing the muscles is important. Autogenic training and relaxing facial massages also have a positive effect on the emotional state of the person concerned. Those affected should integrate simple but effective exercises into their daily routine.
Grimaces, such as raising both eyebrows and corners of the mouth or forming a kissable mouth are just as helpful as pressing the lips and eyes together, wrinkling your nose and blowing up your cheeks or a balloon. Any facial expressions from the evil eye to expressing great joy are helpful.


.jpg)

.jpg)






.jpg)
.jpg)