At a Hyponatremia the sodium level in the blood is too low. It is one of the most common electrolyte disorders.
What is Hyponatremia?

© anaumenko - stock.adobe.com
Hyponatremia is when the sodium level is too low. This leads to a reduced concentration of sodium ions in the blood. The concentration drops to values below 135 mmol / l. In severe cases, life-threatening attacks of hyponatremia are even possible and require immediate hospital treatment. Hyponatremia is one of the most common electrolyte disorders.
It shows up in 15 to 30 percent of all patients who undergo inpatient therapy. The occurrence of hyponatremia extends the patient's hospital stay as the clinical prognosis deteriorates. But athletes can also be affected by the electrolyte disorder if they drink a lot of fluids before a competition. There are several forms of hyponatremia: these are hypovolemic, normovolemic and hypervolemic hyponatremia.
In the case of hypovolemic hyponatremia, the increase in sodium concentration is associated with a reduced blood volume. A typical distinguishing feature is the lower central venous pressure, which is noticeable through empty neck veins. Normovolemic hyponatremia is when the blood volume is normal with the increased sodium concentration.
Hypervolemic hyponatremia is a combination of increased sodium concentration and reduced blood volume. This increases the central venous pressure.
causes
In hyponatremia, it is initially assumed that there is a lack of sodium. However, the electrolyte disorder is triggered by a relative excess of water in the body. During this process, the organism no longer properly excretes pure water through the kidneys. In relation to the sodium concentration in the body, the excess water in the blood turns out to be too high.
The volume of the extracellular fluid is determined by the solution water of the sodium ions and their counterions such as chloride. In the intracellular fluid, on the other hand, potassium is predominant. In the case of a rapidly occurring sodium deficiency, the oncotic pressure drops. The water now flows into the body cells, in which there is initially a higher oncotic pressure, which results in an increase in the cell volume. This, in turn, can lead to an increase in pressure in the brain. The symptoms of the disease then correspond to the complaints that occur with increased intracranial pressure. However, if hyponatremia develops slowly, it does not happen.
The most common triggers for hyponatremia are excessive drinking of water, water overload from gastric lavage, psychogenic polydipsia, the use of certain medications such as diuretics or ACE inhibitors, as well as severe diarrhea and renal salt loss. However, diseases such as pituitary insufficiency, hypothyroidism or adrenal insufficiency are also possible causes.
Symptoms, ailments & signs
One problem with hyponatremia is its unspecific complaints, which often lead to misdiagnosis. These include muscle cramps, seizures, lethargy, loss of appetite, confused behavior, and disorientation. Even a coma is possible. With rapidly progressing hyponatremia, brain edema occurs. This manifests itself in tremors, nausea, headaches and epilepsy attacks.
On the other hand, if the electrolyte disturbance occurs slowly, the patient initially suffers from confusion and fatigue for two days. There are also changes in his personality. If the hyponatremia takes on a chronic form, gait disorders and frequent falls often occur. Since the electrolyte disturbance also has a negative effect on the mineralization of the bones, there is a tendency to bone loss (osteoporosis), which in turn increases the risk of bone fractures.
Diagnosis & course of disease
The diagnosis of hyponatremia is usually carried out by determining the serum sodium value. Other important parameters are the urine osmolality, the serum osmolality, the extracellular volume status and the urine sodium concentration. The determination of these parameters must be done as quickly as possible.
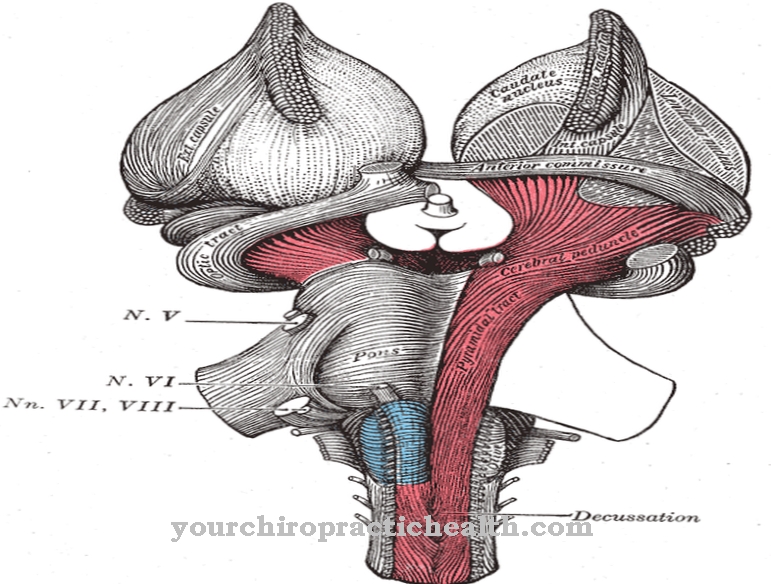
Exclusion diagnostics also play an important role. So it is important to rule out other diseases that may be responsible for the symptoms. These can be kidney or thyroid disorders. The course of hyponatremia depends on the extent of the electrolyte disturbance. In severe cases, complications such as central pontine myelinolysis, which damage the covering of nerve fibers within the brain stem, can occur.
Complications
The hyponatremia can cause various symptoms. The complications and symptoms usually depend on the actual level of sodium in the blood and for this reason can vary. The patient usually feels sick and has a loss of appetite. Furthermore, the person concerned appears confused and can no longer concentrate and coordinate properly. The muscles hurt and cramps and nausea are not uncommon.
In the further course of the hyponatremia, epileptic seizures and severe headaches can also occur in the patient. It is also not uncommon for gait disorders and fatigue to occur. The person concerned is also no longer resilient and feels defeated. The patient's quality of life is significantly reduced by the hyponatremia.
The treatment of hyponatremia always takes place causally and depends on the underlying disease. As a rule, there are no further complications. The symptoms can be resolved with the help of solutions and infusions. If the person concerned also has heart problems, these will be treated. The further course of the disease in most cases depends on the cause of the hyponatremia.
When should you go to the doctor?
If symptoms such as muscle spasms, seizures, and lethargy are noticed, the cause may be hyponatremia. A doctor's visit is indicated if the symptoms persist for more than a week or if they recur after a few months. Medical advice is required at the latest when additional symptoms appear. Nausea and vomiting, headaches and changes in behavior must be clarified immediately. If there are tremors or epilepsy attacks, friends and relatives or the person affected must call the emergency doctor himself. In severe cases, first aid must be provided until the doctor arrives.
Other warning signs that require clarification are tiredness, confusion and gait disorders. Common bone fractures are also indicative of hyponatremia and should be evaluated by a doctor. People diagnosed with sodium deficiency are particularly prone to developing hyponatremia. If the above symptoms occur after excessive consumption of water, gastric lavage, or during psychogenic polydipsia, medical advice is required. People who take diuretics or ACE inhibitors regularly should tell their doctor about any unusual symptoms.
Doctors & therapists in your area
Therapy & Treatment
Treatment of hyponatremia depends on the form and cause of the electrolyte disorder. If hypovolemic hyponatremia is present, volume substitution with isotonic NaCl solution takes place. If, on the other hand, it is the normovolemic form, sodium is administered slowly and partially. In the case of hypervolaemia, the supply of water to the patient's body is limited. In some cases, the administration of table salt can also be useful.
This is done either through the gastrointestinal tract or as an infusion. To avoid central pontine myelinolysis, it is important to slowly and carefully balance the sodium levels. Regular laboratory tests are required for this. In the case of mild hyponatremia, it is often sufficient to stop taking drugs such as thiazide diuretics. It also helps treat heart failure or limit excess water intake, depending on the underlying cause.
In the case of hypervolemic hyponatremia, a combination of saline and loop diuretics may be helpful. Some patients may need hemofiltration.
prevention
Athletes can prevent hyponatremia by avoiding too much water before a competition. In a competition, 150 to 300 milliliters of water are considered useful every 15 to 20 minutes, which corresponds to a small cup.
Aftercare
After treating hyponatremia, it is important for patients to find out about prophylaxis and follow-up options. The disease often occurs in combination with too much water intake. The aftercare is therefore about consciously paying attention to the amount you drink.
This is the only way for those affected to control their electrolyte balance. Those who suffer from the disease more often can minimize the risk by using dietary supplements with sodium. Doctors will prescribe these remedies and give patients precise instructions on dosage. Those affected should adhere to these so that they take the right amount.
These supplements are also available over the counter in pharmacies and drugstores. For individual follow-up care, however, patients should always speak to their doctor in order to avoid errors in dosage. Depending on the cause of the disease, follow-up care can also be extended to the subsequent therapy for the underlying disease.
This often includes follow-up examinations related to kidney problems or cardiovascular complications. Short-term solutions are more likely to be used following an acute illness. Longer-term follow-up treatments usually do not play a role. However, people should not forget to monitor their sodium intake.
You can do that yourself
Hyponatremia can be avoided in many cases. If those affected are athletes, they are advised not to take in excessive amounts of water before competitions. The water supply should rather be done every 20 minutes with 200 milliliters in order to create a balanced electrolyte balance. In most cases this corresponds to an ordinary cup of water.
When treating hyponatremia, people can limit the disease by taking sodium supplements. These can be prescribed by a doctor or purchased directly from a drugstore or pharmacy. However, the patient should always consult their doctor in order not to take in too high an amount of sodium.
If the disease has other causes, in most cases the underlying disease is treated first. As people often have kidney or heart problems due to hyponatremia, these organs should be checked regularly. This can prevent further complications. Furthermore, the hyponatremia in acute conditions can be treated by limiting the water supply. However, it should not be a long-term treatment option.


.jpg)
.jpg)


.jpg)