Under the paracrine secretion medicine understands the hormone secretion in the interstitium, which affects cells in the immediate vicinity. The paracrine secretion is primarily used to differentiate tissue. For example, paracrine disorders can affect bone formation and affect the entire endocrine system.
What is Paracrine Secretion?

Paracrine secretion is a secretion pathway from glands and gland-like cells. Secretions such as growth factors or hormones are not transported endocrinically via the blood to the target tissues, but act on their immediate environment.
The autocrine secretion is a special form of this principle. With this secretion pathway, the secreted substances act back on the secreting cells themselves. For this purpose, the secreting cells are themselves equipped with receptors to which their own secretions can bind. Although secretions are basically designed to act outside the glandular cells, they have an intracellular effect. Paracrine secretions without an autocrine effect only show an effect on the immediately adjacent cells.
Some gland cells of the human organism are involved in endocrine and paracrine secretions at the same time. An example of such cells are the Leydig interstitial cells, which are located in the interstitium of the testicle. Paracrine and endocrine secretion processes usually complement one another rather than exclude one another. But they also have mutually polar properties.
The main task of paracrine secretion processes is to stimulate growth functions or differentiation processes.
Function & task
In the long term, hormones control the growth and function of individual cells, tissues and organs in the human body. In contrast, the autonomic nervous system only takes on the control of time-limited processes. The hormonal system thus has global life support tasks, as it influences organs and controls cell metabolism and the differentiation of individual cells.
The individual effects of all hormones are optimally coordinated and regulate each other to a certain extent by inhibiting or stimulating each other. In the human body, only tissue hormones and so-called cytokines are secreted paracrine. Cytokines are regulatory proteins, i.e. peptides. Above all, they control the immune response and are produced by various instances of the immune system, such as lymphocytes.
The immunological proteins do not always have a paracrine effect, but also have an endocrine effect. Their paracrine effect largely corresponds to the special form of autocrine secretion. The paracrine, autocrine and endocrine effects of the cytokines are network-like and form a homeostasis, i.e. a balance for the maintenance of complex organ functions and other processes in the organism.
In addition to the cytokines, the secretions of some endocrine cells are partly released in a paracrine way. The beta cells of the pancreas and some cells in the anterior pituitary gland secrete their hormones in addition to the endocrine form, for example paracrine, and thus act on the cells in the immediate vicinity after being released into the interstitium, which are equipped with a receptor for the respective hormone. Depending on its type and concentration, the secretion triggers a specific response after binding to the cells. The combination of paracrine and endocrine forms changes the effect of the signal substances released.
The regulation patterns in paracrine secretion mainly consist of the inhibition of the environment. Such environmental inhibitions prevent cells in tissue patterns that are directly adjacent to one another, for example, from differentiating into exactly the same form during differentiation.
In the case of the paracrine special form of autocrine secretion, on the other hand, the ultrashort feedback is the best-known regulatory mechanism. After secretion, the secretions bind to the receptor proteins of the secreting cell itself and thus inhibit their own production.
Illnesses & ailments
If too few or too many paracrine hormones are released, this has an effect on the entire hormone balance and thus also on the organs or tissue of the organism due to the close interaction of the secretion pathways.
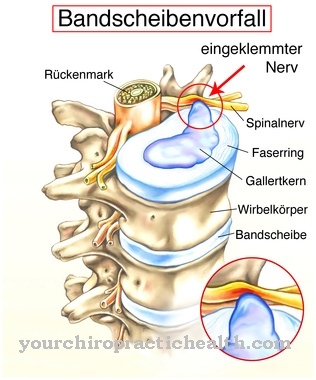
The individual symptoms of a hormone formation or secretion disorder are therefore diverse. The medical department of endocrinology deals with hormonal diseases and thus also disturbed paracrine secretion. As a rule, growth and development are disturbed when there is an endocrine or paracrine disease. For example, paracrine factors can play just as important a role in the development of osteoporosis as they do in metabolic disorders.
One of the most important discoveries is the relevance of paracrine autocrine processes in the development of cancer. In particular, secreted growth factors play a role here, which stimulate the tissue to grow when the intracellular signal cascade is disturbed. The molecular mechanisms of action of paracrine and autocrine substances, the receptors for these substances and the control loop for the release of growth factors have become a focus of cancer research in recent years.
Due to the autocrine growth control, the growth of a tumor, for example, is independent of external factors. Therefore, the autocrine-controlled growth control offers itself as a starting point for modern cancer therapy. The concentration of growth factors can for example be reduced by the administration of monoclonal antibodies. Blocking the respective receptors and thus interfering with paracrine autocrine body processes is also a promising therapeutic option for cancer.










.jpg)
.jpg)