It is certainly not an exaggeration to say that we all find it pleasant when we can enjoy fresh air again after a long stay in a warm room. This discomfort in overheated rooms is not only caused by the lack of oxygen, but is mainly caused by a build-up of heat in the body. But not all people react equally to the effects of heat. This can be seen very clearly, for example, in overcrowded school rooms, where children are often exposed to such heat build-up. If this exceeds a certain level, some children only feel uncomfortable, others have fainting spells, while some do not react at all.
Causes of Overheating in Babies & Infants

Hydration and a cooling bath can quickly put an end to overheating, because in such cases the lack of fluids is the main focus.
Several causes must be used to explain this different response. Some children are simply too warmly dressed, or their clothes are not breathable enough. The different thermoregulatory abilities of the individual child also play a role. The blood circulation in the skin and the secretion of sweat are not the same in every person. Finally, the ability of the nervous system to react is also of considerable importance. Mainly sensitive, easily excitable children often respond to minor heat build-ups with pathological reactions.
Experience has shown that small children are particularly at risk, especially because body temperatures rise relatively quickly to values of 40 degrees and above, especially in the first few years of life. While infants and older children have the ability to adjust to the same body temperature as adults, young children are less able to do this than larger ones for various reasons.
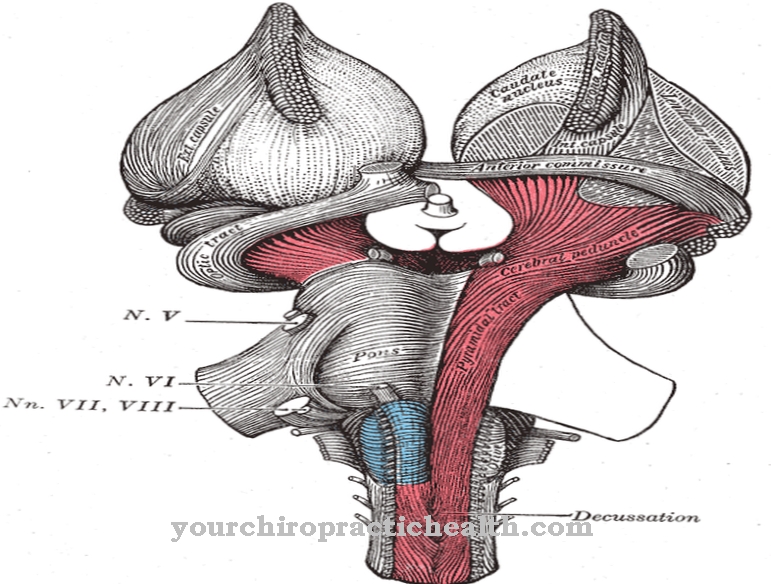
Body temperature is regulated by a special heat center in the brain. The most important are the physical processes in the organism, which consist in the alternation of blood circulation in the skin, in the evaporation of water, especially through the skin surface, but also through the lungs and finally in the generation of heat through muscle movement.
The infant is in a particularly unfavorable situation here. With him, the function of the hair-thin blood vessels is not yet fully developed. In addition, there is the inability to withdraw from an unsuitable shell of one's own accord or even to do active muscle work.
Incidentally, this inability to properly regulate the temperature relates to overheating as well as hypothermia, especially in premature births. However, while hypothermia occurs relatively rarely, it is precisely in families in which the child is looked after with special care that symptoms of overheating are common.
For many years, however, doctors have observed that infant mortality falls as a result of nutritional disorders during the summer months. However, there are several causes of infant mortality. On the one hand, germs can easily accumulate in food at elevated outside temperatures, on the other hand, infectious bowel diseases are particularly common in summer, and finally the repeatedly mentioned heat build-up plays a role that should not be underestimated.
In summer and winter, many parents wrap their babies in beds that prevent heat dissipation. It is also undeniable that children who live in overheated rooms, e.g. in loft apartments and eat-in kitchens, live, get sick more often.
In this context, it should be noted that brief overheating only results in increased temperatures, which, however, quickly equalize when the maintenance error is recognized and eliminated. Often, however, the parents do not notice anything unusual at first. Babies in a threatening condition are brought to the doctor again and again, especially during major heat waves. They suffer from excessive temperature, drowsiness, hardly reacting to their surroundings, have dry tongues and breathe in a rushed and panting manner, which is a typical sign of heat build-up.
treatment
Hydration and a cooling bath can put an end to this condition quickly, because in such cases the lack of fluids is in the foreground. The children do not have the opportunity to compensate for the build-up of heat through increased water release. Children who suffer or have suffered from diarrheal disease and therefore have reduced water and salt supplies are particularly at risk. However, dehydration and a lack of salt cause changes in the swelling of the tissue and increased blood thickening with a simultaneous slowdown in blood flow. These metabolic changes can cause severe clinical pictures with impaired consciousness and symptoms of intoxication within a few hours.
Any heat build-up in patients with a fever requires immediate action. The doctor must first ensure tolerable temperatures and good ventilation in the hospital room, remove heavy duvets and replace them with light blankets. For many years, open-air treatment for children with pneumonia in clinics has proven its worth. Even babies, if they are appropriately packed, can be brought outside at temperatures down to minus five degrees. This method has been used successfully in the treatment of severe pneumonia associated with whooping cough.
Very concerned parents and especially grandparents often make serious mistakes in an effort to do what is best for their child or grandchild. The widespread belief that drafts are harmful to children is particularly important. In such cases, infants who have already had temperatures of around 40 degrees at home are wrapped deeply in feather pillows and clad in warm woolen clothes, taken to the clinic. At most, the tip of the nose of the unfortunate little ones can be seen. No wonder that such children, especially on longer journeys, are brought in with considerable heat build-up.
Doctors & therapists in your area
Examples
For example, in July a feverish three and a half months baby was taken to hospital. He suffered from an otitis media and suddenly began to groan and breathe. The ambulance ride took about an hour. Nevertheless, in spite of its fever, the child was packed in thick blankets and pillows. The linen and pillows were heavily sweaty. The clinical thermometer registered 42 degrees, the baby was already unconscious. Despite all the measures taken immediately, the child died after just 12 minutes. Together with the underlying disease, overheating had caused death here. A case that is unfortunately not so rare, even if fortunately in most cases it is possible to compensate for the overheating that has occurred.
Another example may illustrate how dangerous heating pads can be at times, even if they don't burn you. For the mother of a six week old baby, the bedroom seemed too cold. So she put the child on an electric blanket at around 1 a.m. At about half past four she felt the temperature rise too high. The little face was noticeably pale, and liquid was dripping from his mouth and nose. Here, too, only death could be determined in the nearby hospital. The three and a half hours of overheating had been enough to cause the child's death, the investigation found.
A similar case occurred in a nine week old baby. When she got diarrhea again shortly after inpatient treatment for nutritional disorders (see also our article: Baby Nutrition and Eating Disorders Part 1), the doctor prescribed warmth on her stomach, among other things. The infant was last fed around midnight and was then covered with a heating pad and a damp compress. When the parents checked on the child four hours later, it was already dead. Although minor skin burns were found on the abdomen and thighs, the child died not from the burns but from the overheating.
prevention
In order to prevent such tragic accidents, parents and especially the often over-anxious grandparents should make some basic rules their own. The most important thing seems to be not to bring babies and toddlers to oven temperature because of fear. It is far healthier for children to sleep in unheated rooms than to expose them to dry, warm air.
During the summer heat, babies should only be lightly clothed and, if possible, kept in cool rooms. See also our article: Baby outside in summer and in the heat, Part 1. Ensure that you have sufficient fluid intake, although the amount must not be too large.
On very hot days, it is best to offer babies a few sips of tea outside of meals. A feverish child should never be wrapped in thick feather pillows. If you transport a feverish child outdoors, it is best to wrap it in a light blanket; this is also unnecessary in the ambulance. The principle is to always give the child the opportunity to naturally lower the excessively high temperature through evaporation, sweating and exercise.








.jpg)