Interleukins form a subgroup of cytokines, cellular messenger substances that control the immune system. The interleukins are short-chain peptide hormones with 75 to 125 amino acids. They mainly control the local use of leukocytes at inflammation sites, but they can also have systemic effects such as triggering a fever.
What are interleukins?
Interleukins (IL) are short-chain peptide hormones with 75 to 125 amino acids. They are one of several subclasses of the cytokines that control the immune system. As a messenger substance, interleukins have a similar range of uses as interferons, which also form a subclass of cytokines.
However, interleukins are particularly specialized in controlling leukocytes. Some interleukins also show systemic effects in that they can trigger a fever, for example, while interferons are more specialized in the defense against viruses and have anti-tumor properties. In contrast to neurotransmitters, interleukins and interferons are specialized in communication with cells of the immune system among themselves and with tissue cells. Their main effect usually takes place locally in the tissue.
In order to communicate with cells of the immune system or with tissue cells, interleukins do not have to penetrate the cells; they merely dock onto specific receptors on the cells, which is sufficient to induce the immune cells to proliferate, differentiate and become active.
Function, effect & tasks
Each of the more than 40 different interleukins performs a specific task. Overall, interleukins control the use of leukocytes, but also to some extent the use of T helper cells, monocytes and macrophages and other immune cells.
The basic tasks are to stimulate cells of the immune system to mature, to grow and to divide, i.e. to multiply, if necessary. This also includes the opposite process, the reversal of certain immune reactions. Interleukin-1 can generate a fever if certain conditions are met. IL-1, together with IL-6 and tumor necrosis factor, is one of the so-called pyrogens. The IL-2 specializes in the stimulation, proliferation and differentiation of T helper cells, B cells and natural killer cells. The most important task of the IL-3 is to emit stimulation stimuli that allow certain pluripotent stem cells to mature into erythrocytes, granulocytes or other cells of the immune system.
IL-4 also has the ability to transmit stimuli for proliferation and differentiation to T cells, but at the same time it also has an inhibitory effect on the activity of macrophages. IL-4 therefore also has an anti-inflammatory effect. Target cells of certain interleukins can be stromal cells or fibroblasts as well as all cell types that belong to the immune system, as with IL-17. In order to modulate the inflammatory processes in the skin, the interleukin-20 probably directly controls the immune response of the keratinocytes in the top layer of the skin.
A few interleukins, such as IL-28 and IL-29, recognize virus-infected cell lines. The IL-24 is probably the only interleukin that can recognize tumor cells and that has a tumor-inhibiting effect by inhibiting growth and inducing cell apoptosis, the self-induced cell death.
Education, occurrence, properties & optimal values
Most interleukins are released by cells with immunological relevance mainly in the intercellular area, where they can dock on the secreting cell itself or on other cells of the immune system. Only in a few exceptional cases do specialized interleukins occupy receptors on cells that do not belong to the immune system.
An exception is, for example, the IL-33, which is released in the lungs and skin, can dock to receptors of the IL-1 family. As with IL-4, IL-5 and IL-13, the target cells are mostly T cells and in some cases also eosinophils and mast cells. In principle, the communication between the cells is in the foreground with interleukins. It is mostly a small-scale, local communication, whereby in exceptional cases systemic effects are also achieved. Some interleukins are similar to growth factors because their effect on T cells, monocytes, and lymphocytes is comparable to that of growth factors.
Due to the high dynamics that result from the changing demands on the immune system, specifying a reference value or an optimal value for its occurrence in the body does not make sense. Problems can, however, arise due to reduced or excessive secretion, such as is observed in allergic reactions.
Diseases & Disorders
The very complex interaction of the individual components of the immune system causes a multitude of possible disorders, weakening of the immune response or an excessive reaction to certain challenges, which can lead to mild to serious symptoms.
In some cases, however, the secretion of the cytokines is not disturbed, but the problem is with disturbed receptors, to which interleukins and other cytokines cannot dock. The immune response to inflammation in the tissue is dominated by IL-1. As an inflammation-promoting signal substance, its activity can be pathologically increased, so that not only dead body tissue is phagocytosed and transported away, but also healthy cells are attacked and diseases such as rheumatism and osteoarthritis are caused in joints. In these cases an antagonist to the IL-1 can help, which curbs the immune response through the IL-1.
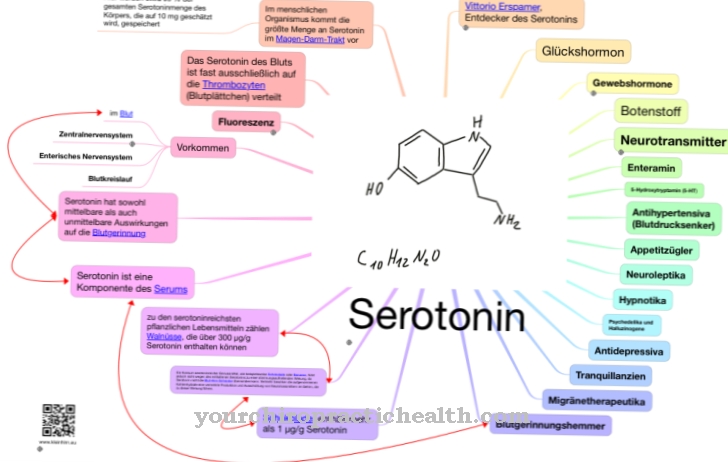
Antagonists to IL-1 can also be used for other autoimmune diseases such as Crohn's disease, MS and psoriasis. Because interleukins are made up of relatively short-chain proteins or polypeptides, most of them can also cross the blood-brain barrier. In some cases, specialized astrocytes take care of the transport. Even if there is no direct specificity of the individual interleukins with regard to schizophrenia and depression, clear connections can be found, for example, between the hypersecretion of IL-2 in schizophrenia and of IL-6 in depression. Interleukins and other cytokines exert a strong influence on neurotransmitters like dopamine, serotonin, adrenaline, noradrenaline and others.







.jpg)

.jpg)
.jpg)











.jpg)